In 2026, the ability to manage days in ar is more critical than ever for healthcare and business organizations seeking financial stability. Delays in collecting payments can strain cash flow, disrupt operations, and limit opportunities for growth.
With digital transformation reshaping the industry, organizations face increasing pressure to accelerate collections and optimize their revenue cycles. Staying ahead means adapting to new standards and expectations for payment efficiency.
This guide delivers a clear, actionable approach to managing and reducing days in ar. You will gain practical steps to strengthen cash flow and streamline operations.
We will break down what days in ar means, how to calculate it, identify common causes of delays, and share proven strategies for improvement. Explore how technology is changing the landscape and what future trends to watch as you work towards financial excellence.
Understanding Days in AR: Definition, Importance, and Benchmarks
Understanding days in ar is essential for financial leaders aiming to drive operational efficiency and maintain healthy cash flow. This metric measures the average time it takes for organizations to collect payment after delivering services or issuing invoices. In both healthcare and business settings, days in ar serves as a vital performance indicator reflecting the effectiveness of revenue cycle management. For example, clinics might track days in ar to monitor how quickly they receive payments from insurers, while medical device companies use it to gauge liquidity. For a deeper dive, see Days in Accounts Receivable (A/R) – RCM Metrics for industry perspectives on this KPI.
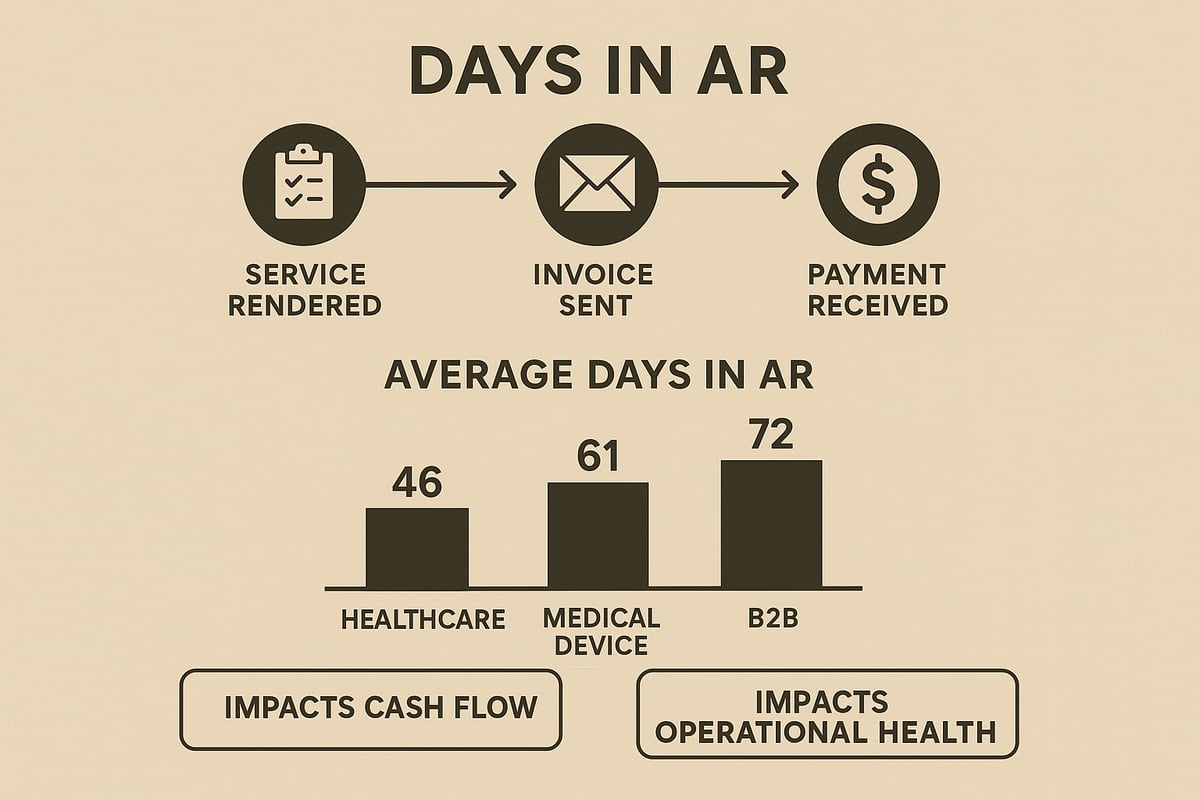
What Are Days in AR?
Days in ar represents the average number of days it takes an organization to collect outstanding payments after providing a service or issuing an invoice. This metric is crucial in both healthcare and business sectors, where efficient revenue cycle management directly impacts liquidity and the ability to fund daily operations. For instance, a medical clinic may monitor days in ar to ensure timely payments from insurance companies, while a medical device manufacturer uses it to assess overall financial health. Ultimately, days in ar reveals how effectively revenue is being converted into cash.
Why Days in AR Matter in 2026
In 2026, days in ar takes on greater significance as industry expectations rise and digital transformation accelerates. Extended days in ar can lead to increased operational costs, cash flow constraints, and challenges in meeting payroll or funding expansion. High-performing organizations now target days in ar below 30 to 40, while figures above 50 indicate inefficiency. Imagine a scenario where delayed collections disrupt supply orders or hinder staff hiring. By keeping days in ar low, organizations enhance financial stability and remain competitive in a rapidly evolving landscape.
Industry Standards and Benchmarks
Benchmarks for days in ar vary by industry, specialty, and payer mix. In healthcare, optimal days in ar typically fall under 30 to 40, with values above 40 signaling the need for process improvements. Larger organizations or those with diverse payer mixes may see slight variations. Below is a comparison table:
| Industry | Optimal Days in AR | Warning Level |
|---|---|---|
| Healthcare | <30-40 | >40 |
| Medical Supplies | <35 | >45 |
| B2B Services | <40 | >50 |
Organizations maintaining low days in ar often report improved cash flow and stronger revenue cycle health, reinforcing the importance of ongoing monitoring and benchmarking.
Key Metrics Related to Days in AR
To gain a complete picture of financial performance, it is important to track metrics alongside days in ar. These include Days Sales Outstanding (DSO), collection rates, denial rates, and patient AR over 90 days. Each metric offers unique insights and, together, they highlight areas for targeted improvement. For example, practices using automation have reduced their days in ar by up to 76 percent, underscoring the value of metric-driven decision making. By monitoring these interconnected indicators, organizations can make informed decisions that drive sustained financial health.
Step-by-Step Guide: How to Calculate Days in AR Accurately
Calculating days in ar with precision is essential for understanding your organization's financial health. By following a consistent, step-by-step approach, you can accurately measure performance, reveal process issues, and uncover opportunities for improvement. Let’s break down the process into five clear steps, each building on the last.
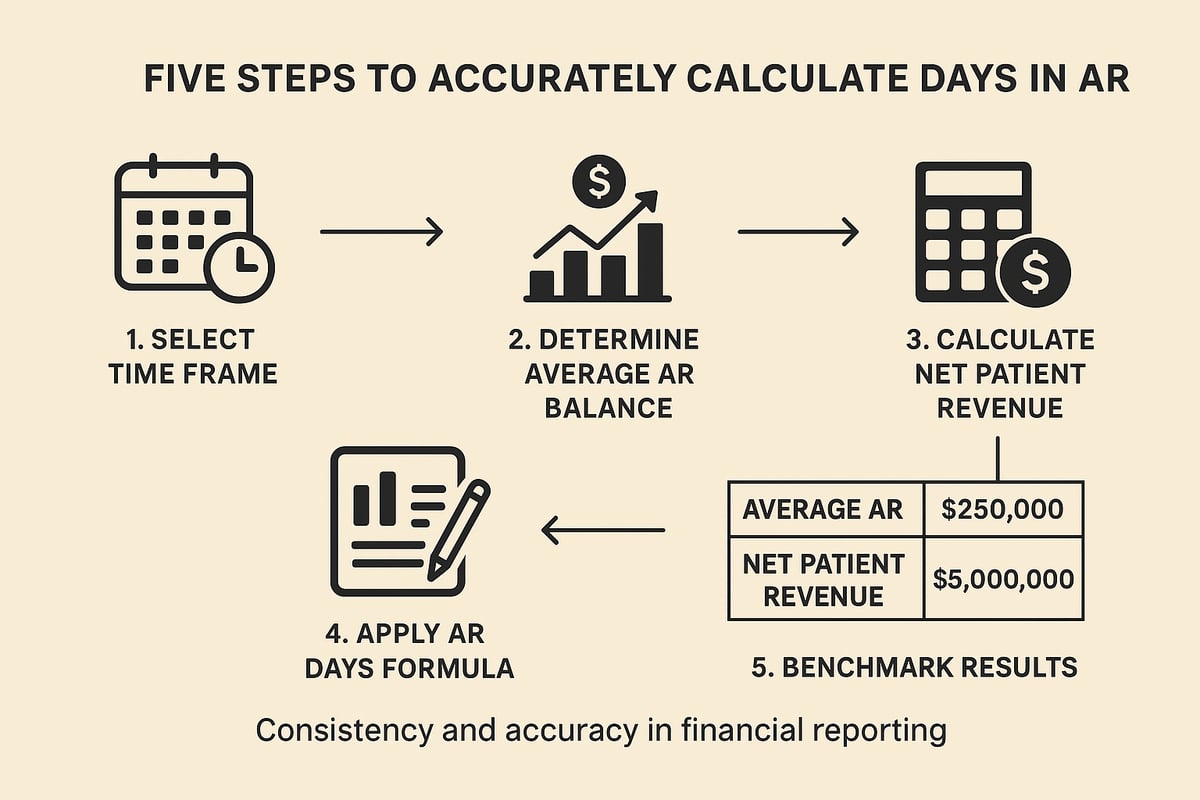
Step 1: Select Your Time Frame
The first step in calculating days in ar is to choose a consistent reporting period. This could be monthly, quarterly, or annually, depending on your organization's needs. Using a regular time frame allows you to compare performance over time and benchmark against industry standards.
For instance, a monthly calculation (30 days) gives quick insights, while a quarterly view (90 days) helps spot trends. Always match the time frame to your reporting and analysis goals. If your AR balance at the start of January was $120,000 and at the end was $100,000, using a monthly window ensures comparability. Consistency is key to making your days in ar data actionable.
Step 2: Determine Average AR Balance
Next, calculate your average AR balance for the chosen period. The formula is simple: (Beginning AR + Ending AR) divided by 2. Include both insurance and patient receivables, but exclude credits or prepayments.
For example, if your AR started at $120,000 and ended at $100,000, the average is ($120,000 + $100,000) 2 = $110,000. If you notice your average AR rising over several periods, it could signal collection issues. Accurate reporting of AR balances is crucial for a trustworthy days in ar calculation and for identifying process bottlenecks.
Step 3: Calculate Net Patient Revenue or Net Credit Sales
Now, determine your net patient revenue or net credit sales for the period. This figure should reflect charges for services rendered, minus any adjustments, discounts, or write-offs. Do not include cash payments for old claims, non-patient income, or prepayments.
Suppose your total charges for the month are $180,000, with $10,000 in adjustments. Your net patient revenue is $170,000. Always align the revenue period with your AR balances. This alignment ensures your days in ar result truly represents how quickly you collect payments for recent services.
Step 4: Plug Into the AR Days Formula
With your numbers ready, use the formula:
AR Days = (Average AR ÷ Net Revenue) × Number of days in period
For example, if your average AR is $110,000, net revenue is $170,000, and your period is 30 days:
AR Days = ($110,000 ÷ $170,000) × 30 = 19.4 days
A result of 19.4 means it takes about 19 days on average to collect payment. For more tips on refining your process, see Streamlining Your Billing Process. Accurate days in ar tracking guides informed revenue cycle decisions.
Step 5: Analyze and Benchmark Results
Finally, compare your calculated days in ar to industry benchmarks. Less than 30 days is excellent, 30 to 40 is acceptable, and above 40 signals a problem. Use your findings for internal reporting and to drive performance improvements.
For example, if your days in ar exceed targets, investigate root causes and adjust workflows. Regular calculation and trend analysis help you stay proactive. Organizations that benchmark consistently often see quicker improvements and more stable cash flow.
Common Causes of Extended AR Days and How to Avoid Them
Understanding why days in ar extend beyond benchmarks is crucial for financial health. Organizations face a variety of challenges that can delay collections and disrupt cash flow. Let’s explore the main pitfalls and practical ways to avoid them.
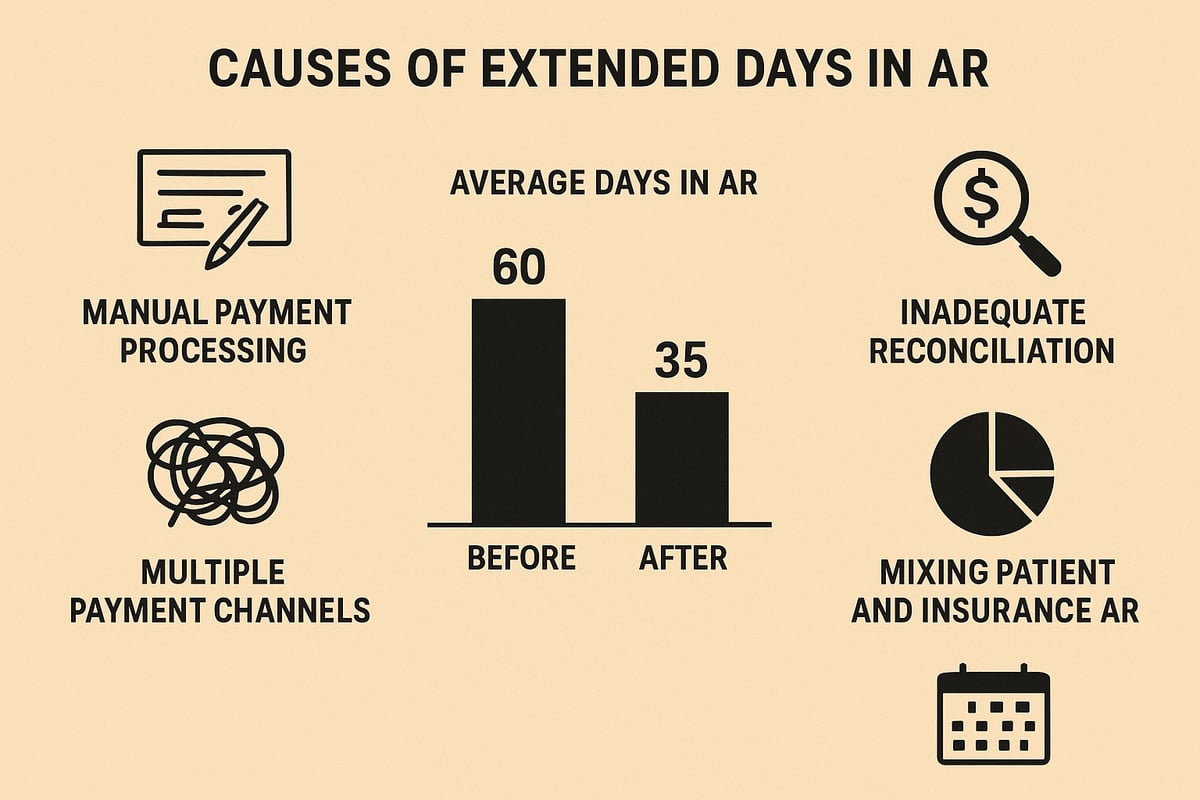
Manual Payment Processing and Data Entry Errors
Manual workflows are a leading cause of extended days in ar. Staff spend hours sorting paper checks, entering data by hand, and tracking down mismatched payments. This not only delays posting but also increases the risk of errors.
For example, if a payment is applied incorrectly, it may take days or weeks to identify and correct, which pushes out collection timelines. According to industry data, automation can reduce days in ar by up to 76 percent.
To solve this, organizations should digitize payment workflows and automate repetitive tasks. For deeper insight into how underpayment and bottlenecks impact days in ar, see Common Healthcare Underpayment Issues.
Multiple Payment Channels and Fragmented Systems
Managing payments from insurance, government, and patients across separate platforms can create confusion. Staff may need to log into multiple systems, slowing down reconciliation and increasing the risk of missed payments. This fragmentation leads to inconsistent updates, making it difficult to track days in ar accurately.
Unified AR platforms can help by consolidating all payment channels into a single interface. Integration reduces manual effort and ensures payments are posted quickly. To avoid delays, prioritize systems that support all payer types and enable seamless data flow. Regularly review your payment channels and look for integration opportunities.
Inadequate Payment Posting and Reconciliation
Another major contributor to prolonged days in ar is inefficient payment posting. If payments are not matched to the correct claim or invoice, accounts remain open longer than necessary. Lack of standardized posting procedures leads to errors and delayed updates.
For instance, when payments are posted days after receipt, organizations lose visibility into real-time cash flow. Best practices include automating the reconciliation process and using clear procedures for payment posting. AI-powered tools can further reduce manual intervention and speed up collections. Regular audits of posting accuracy are recommended to maintain efficiency.
Mixing Patient and Insurance AR
Combining patient and payer accounts receivable can mask collection issues. Patients typically pay more slowly than insurers, so blending these categories inflates average days in ar and hides underlying problems.
Tracking patient and insurance AR separately allows organizations to identify which segment is driving delays. For example, if patient AR is consistently over 90 days, targeted follow-up and payment plans may be needed. Segmenting reports by source provides actionable insights for collection strategies and helps lower overall days in ar.
Ignoring Seasonal Fluctuations and Payer Variability
Seasonal patterns and payer-specific timelines have a direct impact on days in ar. For instance, year-end deductible resets often lead to temporary spikes in outstanding balances. Similarly, different payers have unique processing times, which can skew short-term results.
Failing to account for these factors can result in misinterpreted metrics and misguided decisions. Trend analysis over several periods, broken down by payer, provides a clearer picture. This approach ensures that temporary fluctuations do not trigger unnecessary changes and helps maintain steady progress in reducing days in ar.
Proven Strategies to Reduce Days in AR Effectively
Effectively reducing days in ar is vital for organizations seeking to strengthen cash flow and maintain operational resilience. By adopting a combination of technology, process standardization, analytics, and ongoing staff development, organizations can address common bottlenecks and drive sustainable improvement. Below are proven strategies to optimize every stage of accounts receivable management.
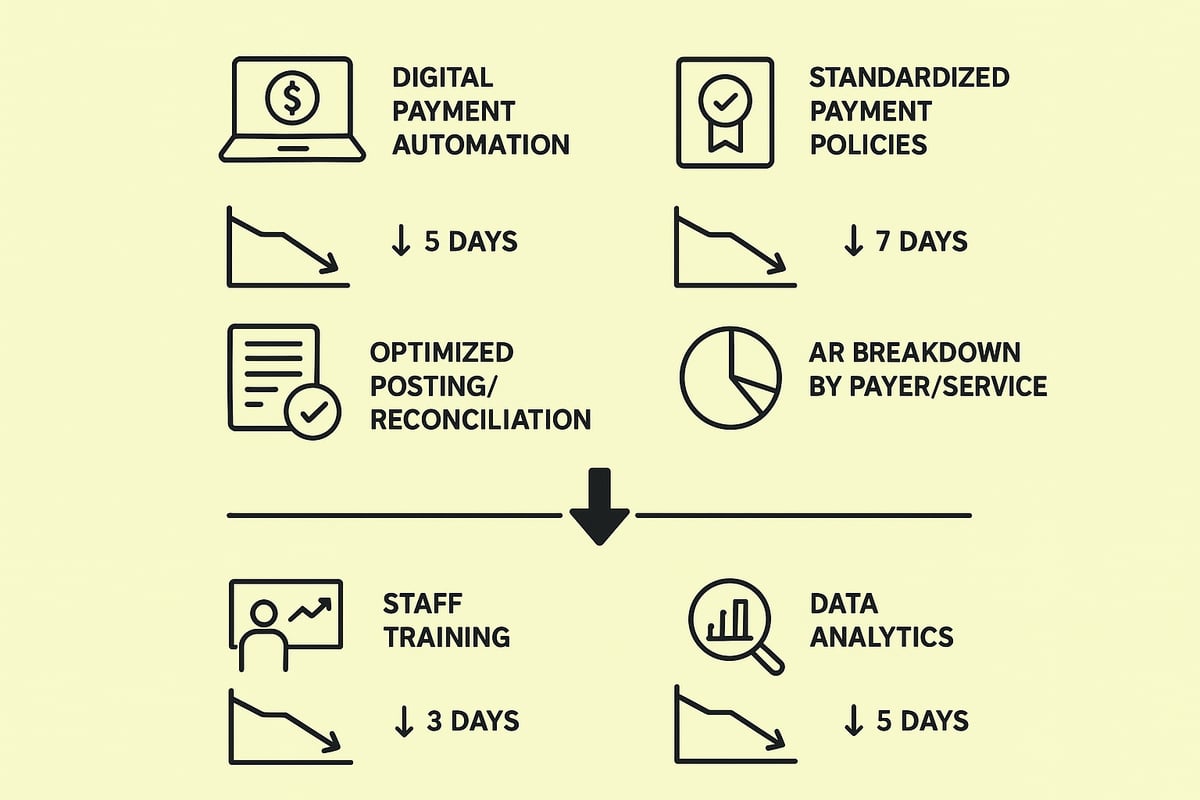
Implement Digital Payment Solutions and Automation
Embracing digital payment solutions and automation is a cornerstone for reducing days in ar. Electronic payment platforms enable instant billing, secure transactions, and automated posting, which minimizes manual errors and accelerates cash flow. For example, integrating online bill pay and mobile payment portals can significantly shorten collection cycles.
Organizations that automate their AR processes often see up to a 76% reduction in days in ar, supported by real-world data. To learn more about how automation can transform AR cycles and cash flow, see Improving Cash Flow in Healthcare: Strategies for Reducing Patient Accounts Receivable Days through Automation.
Initial investments in digital tools often yield long-term returns, including higher collection rates, better patient satisfaction, and more predictable revenue streams.
Standardize Payment Acceptance Policies
Establishing clear and consistent payment acceptance policies is fundamental to managing days in ar. When staff and customers understand payment expectations, confusion and delays decrease.
Effective policies outline acceptable payment methods, timelines, and procedures for overdue accounts. For instance, offering automated payment plans or requiring up-front payments for specific services can drive timely collections.
Regularly reviewing and updating these policies ensures alignment with evolving industry standards. Organizations that standardize payment processes consistently report improved transparency and reduced days in ar.
Optimize Payment Posting and Reconciliation
Streamlining payment posting and reconciliation is essential for accurate and timely AR management. Automated posting procedures, supported by AI and machine learning, can match payments to claims efficiently, reducing manual effort and errors.
Dashboards and real-time reporting provide visibility into the process, allowing staff to identify discrepancies and act swiftly. For example, organizations leveraging automation have achieved notable reductions in days in ar due to faster account updates.
Staff training on new posting systems further enhances accuracy, ensuring every payment is properly accounted for and reconciled.
Break Down AR Days by Payer and Service Line
Analyzing days in ar by payer and service line uncovers valuable insights for targeted action. Segmenting AR data allows organizations to pinpoint slow-paying insurers or high-risk departments, enabling focused follow-up and resource allocation.
Regular reporting by payer or service line highlights trends and outliers, helping teams prioritize collections where they will have the most impact. This granular approach to days in ar ensures continuous improvement and supports proactive revenue management.
By understanding payer-specific patterns, organizations can tailor their engagement strategies for optimal results.
Invest in Staff Training and Performance Monitoring
A well-trained team is crucial for reducing days in ar. Ongoing education on AR processes and new technologies equips staff to handle tasks efficiently and accurately.
Establishing clear performance metrics fosters accountability and encourages continuous improvement. Regular audits and feedback sessions help identify knowledge gaps and reinforce best practices.
Organizations that prioritize staff development often see improved collection rates and lower days in ar. Engaged employees are more likely to embrace change and contribute to process optimization.
Leverage Data Analytics for Continuous Improvement
Harnessing data analytics empowers organizations to monitor, evaluate, and refine their AR strategies. Key metrics such as AR aging, denial rates, and collection percentages provide a comprehensive view of days in ar performance.
Real-time dashboards and automated alerts facilitate rapid response to emerging issues. For example, data-driven organizations can quickly adjust workflows to target bottlenecks and prevent backlogs.
Periodic reviews and data analysis ensure that AR processes remain agile and aligned with organizational goals, driving ongoing reduction in days in ar.
The Role of Technology and Automation in AR Management
Technology is rapidly reshaping how organizations approach days in ar, unlocking new levels of efficiency and control. From unified AR platforms to AI-powered automation, the right tools can transform revenue cycles, reduce delays, and elevate financial performance. Let’s explore how these advancements drive measurable improvements in days in ar management.
Unified AR Platforms and System Integration
A unified AR platform brings all payment channels together, replacing fragmented systems that often slow down days in ar. Integrating AR with EHR, ERP, and practice management systems eliminates manual data entry and creates seamless payment tracking. This results in fewer errors and faster processing times.
Organizations using unified AR platforms benefit from enhanced visibility and control over their revenue cycle. They can quickly identify bottlenecks, monitor trends, and streamline workflows. For a holistic approach, consider End-to-End Revenue Cycle Management solutions that tie every step of AR together, accelerating cash flow and optimizing days in ar.
AI-Powered Payment Matching and Reconciliation
Artificial intelligence is revolutionizing the way organizations manage days in ar. AI-driven payment matching automates the identification and reconciliation of incoming payments with outstanding invoices or claims. This reduces manual workload, minimizes errors, and accelerates cash posting.
Predictive analytics tools can analyze historical data to flag potential payment delays and identify patterns, allowing proactive intervention. Automated denial management and real-time claim status updates further reduce AR aging. When AI is applied strategically, organizations see measurable gains in staff productivity and a significant reduction in days in ar.
Digital Acceleration and Customer Experience
Digital payment solutions are transforming the customer experience and speeding up days in ar. User-friendly online portals, mobile payments, and self-service options empower patients and clients to pay quickly and conveniently. This reduces overdue balances and increases payment rates.
Statistics show that increased digital adoption drives lower days in ar, as payments are processed more rapidly and with fewer errors. By offering multiple digital options and integrating them into the AR workflow, organizations enhance satisfaction and improve their bottom line. A focus on digital experience is key to faster collections and healthier cash flow.
Real-Time Reporting and Dashboard Visibility
Transparent, real-time reporting is essential for managing days in ar effectively. Customizable dashboards display up-to-date AR metrics, including aging, denial rates, and collection percentages. Automated alerts notify teams of potential issues before they escalate.
Organizations that leverage real-time data can make faster, more informed decisions and proactively manage their AR. Integrating reporting into daily workflows ensures that teams stay aligned and can quickly address problem areas. This level of visibility supports ongoing improvements in days in ar and overall financial health.
Future Trends: Automation, AI, and Beyond
Looking ahead to 2026, the future of days in ar management points to even greater automation and advanced AI. Emerging technologies, such as blockchain for secure transactions and robotic process automation (RPA) for repetitive tasks, are gaining traction. Predictive analytics will continue to forecast payment trends and optimize resource allocation.
The shift towards fully digital, end-to-end revenue cycles is accelerating. Forward-thinking organizations are investing in scalable solutions to stay ahead of industry changes. By embracing these innovations, they position themselves for sustained reductions in days in ar and long-term financial success.
Frequently Asked Questions About Managing Days in AR
Healthcare and business leaders in 2026 face new questions about days in ar as financial environments change. Below, we answer the most pressing questions to help you benchmark, monitor, and improve your AR performance with confidence.
What Is a Good Days in AR Benchmark in 2026?
Benchmarks for days in ar vary by industry, payer mix, and organization type. High-performing healthcare organizations usually maintain days in ar under 30 to 40 days. If your metric is above 40, this signals a need for review. Factors such as specialty, claim complexity, and practice size can influence your target. The table below summarizes common benchmarks:
| Industry | Excellent | Acceptable | Red Flag |
|---|---|---|---|
| Healthcare | <30 days | 30–40 days | >40 days |
| Medical Supplies | <35 days | 35–45 days | >45 days |
| General B2B | <35 days | 35–45 days | >45 days |
Organizations who consistently monitor days in ar and adjust processes often outperform their peers.
How Often Should AR Days Be Calculated and Reviewed?
Regular calculation of days in ar is vital for early detection of issues. Most organizations review this metric monthly to quickly spot negative trends. Quarterly reviews help identify seasonal patterns, while annual analysis supports long-term planning. Align review frequency with business cycles for best results. Automated tools and dashboards can streamline ongoing tracking. Consistent review of days in ar allows teams to act quickly and continuously improve revenue cycle outcomes.
What Are the Risks of High AR Days?
Persistently high days in ar can threaten both financial health and organizational reputation. Cash flow shortages may delay payroll, stall investments, or require costly borrowing. Operationally, you might see supply chain disruptions or inability to fund growth. Reputational risks include strained payer relationships and reduced negotiating power. For healthcare providers, common valuation pitfalls can further complicate matters, as highlighted in Healthcare Accounts Receivable Valuation Pitfalls to Avoid in 2026. Proactively managing days in ar helps safeguard stability and trust.
How Can Organizations Get Started with AR Optimization?
Begin by conducting a thorough audit of your current days in ar and related processes. Map workflows, identify bottlenecks, and benchmark against industry standards. Prioritize automation and standardization of payment policies to accelerate collections. Involve cross-functional teams to ensure buy-in and accountability. For practical ideas, explore Strategies to Reduce Accounts Receivable Turnaround Time for actionable steps. Use a checklist to monitor progress and adjust strategies as needed. Improving days in ar is an ongoing journey, but the right start sets the stage for long-term success.
As you’ve seen, mastering days in AR is crucial for maintaining strong cash flow and operational efficiency, especially with the rapid changes we’re all facing in 2026. Whether you want to streamline processes, leverage automation, or empower your team for proactive financial health, applying the right strategies can make a real difference. If you’re ready to take your AR management to the next level or need tailored guidance to boost your organization’s performance, let’s connect. You can Book a Consultation to explore your unique challenges and start building a more efficient, profitable future together.

