Healthcare organizations face mounting pressure to maintain financial stability while delivering exceptional patient care. One of the most significant challenges impacting their bottom line is the growing number of claim denials. Understanding and implementing effective denial management processes has become essential for providers seeking to maximize revenue, reduce administrative burden, and maintain operational efficiency. Organizations that develop systematic approaches to identifying, analyzing, and preventing claim denials position themselves for sustainable financial growth while minimizing the hours spent on manual rework.
Understanding the Financial Impact of Claim Denials
Claim denials represent more than administrative inconveniences. They directly affect cash flow, staff productivity, and overall organizational health. Research indicates that the average denial rate across healthcare organizations ranges from 5% to 25%, with many denied claims never being reworked due to resource constraints.
The financial consequences of poor denial management extend beyond the immediate loss of revenue. Organizations must factor in the additional costs of appeals, staff time devoted to rework, delayed payments, and potential write-offs. Each denied claim requires an average of $25 to $117 to rework, creating a substantial hidden expense that compounds over time.
Key financial impacts include:
- Lost revenue from claims that are never resubmitted
- Increased administrative costs for appeals and resubmissions
- Cash flow disruptions affecting operational planning
- Staff burnout from repetitive manual processes
- Strained relationships with payers and patients
When organizations fail to address denials systematically, they often experience a snowball effect where problems compound, staff morale declines, and revenue continues to erode.

Common Root Causes Behind Claim Denials
Effective denial management begins with understanding why claims get rejected in the first place. The causes typically fall into several distinct categories that require different prevention strategies.
Registration and Eligibility Errors
Patient registration errors account for a significant percentage of preventable denials. These mistakes often occur at the front end of the revenue cycle when demographic information, insurance details, or authorization requirements are incorrectly captured or verified.
Common registration issues include misspelled patient names, incorrect insurance identification numbers, expired coverage information, and missing prior authorizations. Each of these errors creates avoidable downstream problems that result in claim rejections.
Coding and Documentation Deficiencies
Clinical documentation and medical coding accuracy remain persistent challenges for healthcare organizations. When clinical staff fail to document services completely or when coders select inappropriate codes, claims face increased scrutiny and higher denial rates.
The transition to value-based care and increasingly complex coding requirements has amplified these challenges. Organizations must ensure their coding teams stay current with regulatory changes while clinical staff understand documentation requirements that support accurate code assignment.
| Denial Category | Average Percentage | Primary Prevention Strategy |
|---|---|---|
| Registration/Eligibility | 30-35% | Real-time insurance verification |
| Coding/Documentation | 25-30% | Clinical documentation improvement |
| Authorization | 15-20% | Automated authorization tracking |
| Timely Filing | 10-15% | Claim submission monitoring |
| Duplicate Claims | 5-10% | Submission scrubbing technology |
Medical Necessity and Authorization Issues
Payers increasingly scrutinize whether services meet medical necessity criteria. Claims submitted without proper prior authorization or adequate supporting documentation frequently face denials, even when the care was clinically appropriate.
Healthcare organizations must establish robust processes for obtaining authorizations before services are rendered and documenting medical necessity according to payer-specific requirements. The complexity of varying payer policies makes this particularly challenging without automated support systems.
Building a Systematic Denial Management Process
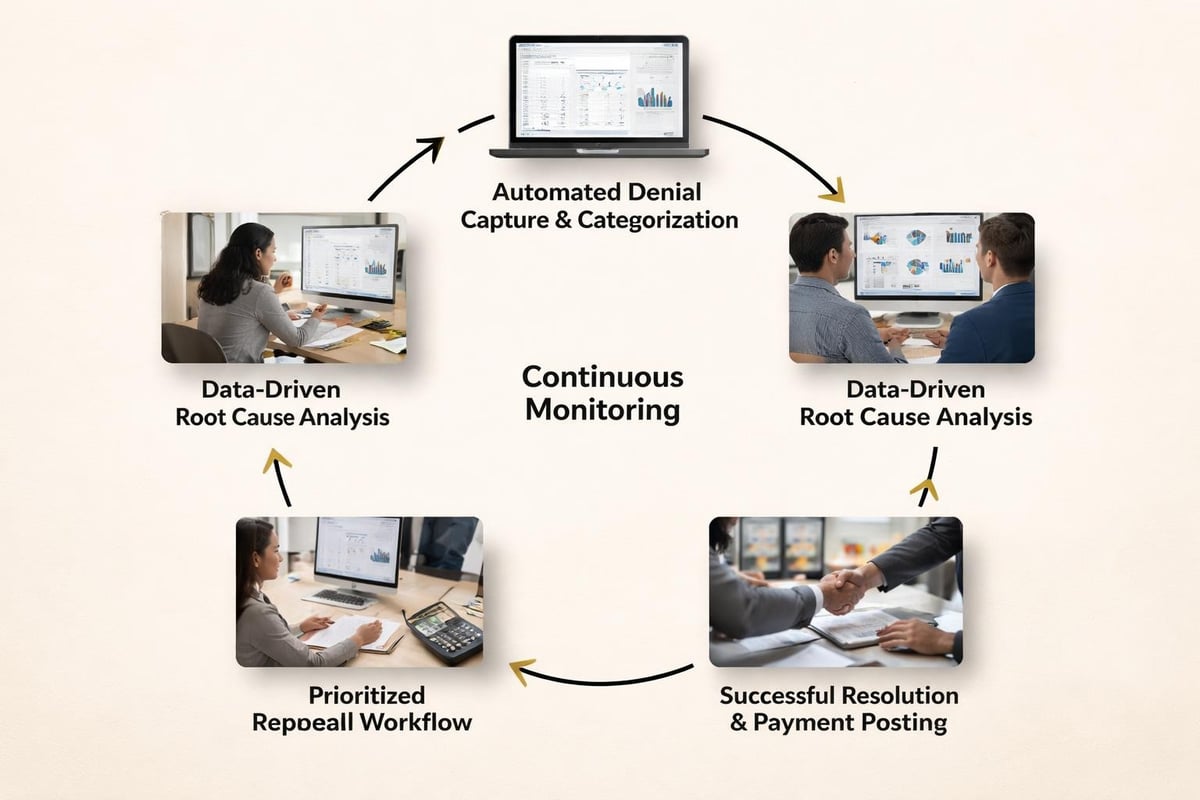
Organizations that excel at denial management implement structured processes that span prevention, identification, analysis, and resolution. This systematic approach transforms denial management from reactive firefighting into proactive revenue optimization.
Denial Identification and Categorization
The first step involves establishing mechanisms to identify all denials quickly and categorize them accurately. Many organizations struggle because denials arrive through multiple channels including electronic remittance advice, explanation of benefits statements, and correspondence from payers.
Implementing technology solutions that aggregate denials from all sources into a single platform enables comprehensive visibility. Denial management processes should include automated categorization based on denial reason codes and business rules that route different denial types to appropriate team members.
Essential categorization elements include:
- Primary denial reason code
- Payer and plan information
- Service date and claim submission date
- Financial impact and patient responsibility
- Appeal deadline and priority level
Root Cause Analysis and Trend Identification
Simply working denials individually addresses symptoms rather than underlying problems. Organizations must analyze denial patterns to identify systemic issues that require process improvements.
Regular trend analysis reveals whether specific payers, providers, service types, or registration locations generate disproportionate denial volumes. These insights enable targeted interventions that prevent future denials rather than simply recovering revenue from past mistakes.
Advanced organizations leverage data analytics to predict denial risk before claims are submitted, allowing for proactive correction of issues. This predictive approach represents the evolution from reactive denial management to intelligent revenue cycle optimization.
Technology Solutions That Transform Denial Management
Manual denial management processes cannot scale to meet the volume and complexity demands of modern healthcare revenue cycles. Organizations that continue relying on spreadsheets and manual tracking face diminishing returns as claim volumes grow.
Artificial Intelligence and Machine Learning Applications
Artificial intelligence revolutionizes denial management by automating pattern recognition, predicting denial risk, and recommending optimal resolution strategies. Machine learning algorithms analyze historical denial data to identify subtle patterns human reviewers might miss.
AI-driven automation solutions can prioritize which denials to work based on likelihood of successful appeal, financial impact, and resource requirements. This optimization ensures staff focus their efforts where they can generate the greatest return on investment.
Natural language processing capabilities enable automated analysis of denial reason narratives, extracting structured data from unstructured text. This automation eliminates hours of manual review while improving accuracy and consistency in denial categorization.
Integration and Workflow Automation
Effective denial management requires seamless integration across multiple systems including electronic health records, practice management platforms, clearinghouses, and payer portals. Disconnected systems create information silos that slow response times and increase errors.
Integrated platforms automatically route denials to appropriate team members based on denial type, expertise requirements, and workload balancing. Workflow automation ensures appeals are prepared according to payer-specific requirements and submitted before deadlines expire.
Organizations implementing revenue cycle management solutions with robust integration capabilities report significant improvements in first-pass resolution rates and staff productivity. The elimination of manual data entry and system switching allows team members to focus on complex problem-solving rather than administrative tasks.
Prevention Strategies That Reduce Denial Rates
While effective appeals processes recover revenue from existing denials, prevention strategies deliver superior returns by avoiding denials altogether. Organizations should allocate resources proportionally between working denials and preventing future occurrences.
Front-End Revenue Cycle Optimization
The most cost-effective denial prevention occurs at the front end of the revenue cycle. Investing in accurate patient registration, real-time eligibility verification, and automated authorization management prevents costly downstream denials.
Real-time eligibility verification systems confirm insurance coverage at the point of scheduling and registration, identifying issues before services are rendered. This proactive approach allows staff to address coverage gaps, collect appropriate patient payments, and obtain necessary authorizations.
Critical front-end prevention tactics:
- Automated insurance verification at scheduling
- Point-of-service payment estimation and collection
- Authorization tracking and automated renewal alerts
- Patient demographic validation against payer records
- Coverage limitation identification and communication
Clinical Documentation Improvement Initiatives
Clinical documentation improvement programs bridge the gap between clinical care delivery and accurate revenue capture. These initiatives educate providers about documentation requirements that support medical necessity, appropriate code assignment, and compliant billing.
Concurrent documentation review identifies deficiencies while patients are still in care, allowing for real-time corrections. This approach proves more effective than retrospective reviews after claims have been submitted and denied.
Organizations should establish feedback loops that inform clinicians when their documentation patterns generate denials. This education helps providers understand the revenue cycle implications of their documentation choices without compromising clinical judgment.
Measuring Denial Management Performance
Organizations cannot improve what they do not measure. Establishing comprehensive performance metrics enables tracking progress, identifying areas requiring additional attention, and demonstrating return on investment from denial management initiatives.
Key Performance Indicators
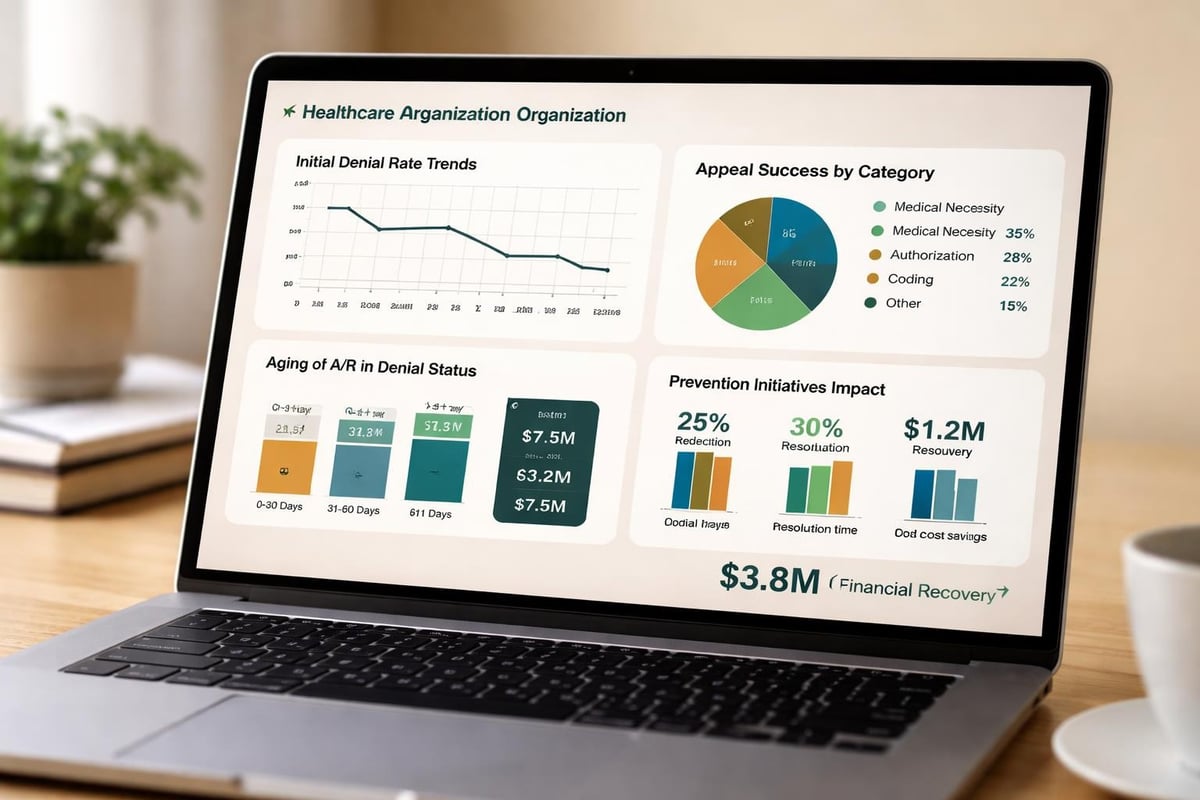
Effective denial management dashboards track metrics across prevention, identification, resolution, and financial recovery. Leading organizations monitor both volume-based and financial metrics to gain comprehensive visibility into program performance.
| Metric | Target Range | Measurement Frequency |
|---|---|---|
| Initial Denial Rate | Less than 5% | Monthly |
| Appeal Success Rate | Greater than 65% | Monthly |
| Days in Denial AR | Less than 30 days | Weekly |
| Denial Write-off Percentage | Less than 2% | Monthly |
| Prevention Rate Improvement | 10% quarterly reduction | Quarterly |
| Cost per Denial Worked | Decreasing trend | Monthly |
Continuous Improvement Methodology
High-performing denial management programs embrace continuous improvement methodologies that systematically identify opportunities, implement changes, and measure results. This disciplined approach ensures sustained gains rather than temporary improvements that fade over time.
Regular team meetings should review performance metrics, discuss challenging cases, and identify process improvement opportunities. Creating a culture where denial trends are analyzed collaboratively rather than used for individual blame encourages open communication and knowledge sharing.
Organizations should celebrate wins when denial rates decline or appeal success rates improve. Recognizing team contributions reinforces the importance of denial management and maintains momentum for ongoing improvement efforts.
Staffing and Training Considerations
Successful denial management requires skilled team members who understand both clinical and financial aspects of healthcare operations. Organizations must invest in recruiting, training, and retaining talent capable of navigating complex payer requirements and regulatory environments.
Role Specialization Versus Generalization
Organizations face strategic decisions about whether denial management staff should specialize in specific denial types or develop generalized capabilities across all categories. Each approach offers distinct advantages depending on claim volume, complexity, and organizational structure.
Specialization enables deep expertise in particular payer policies or clinical areas, potentially improving resolution rates for complex denials. However, this approach may create workload imbalances and reduce flexibility when volume fluctuates across categories.
Generalization provides greater staffing flexibility and broader perspective on systemic issues. Team members who work various denial types often identify cross-category patterns that specialists might miss. The tradeoff involves potentially lower expertise depth for highly technical denials.
Ongoing Education and Development
The healthcare revenue cycle evolves constantly with regulatory changes, payer policy updates, and coding revisions. Denial management teams require continuous education to maintain effectiveness in this dynamic environment.
Organizations should allocate dedicated time for staff training on new regulations, emerging denial trends, and technology enhancements. Professional development opportunities not only improve technical capabilities but also demonstrate organizational investment in staff success, supporting retention.
Cross-training between denial management and other revenue cycle functions creates valuable perspective and career development pathways. Understanding upstream processes helps denial staff identify prevention opportunities, while exposure to denial work helps front-end staff appreciate the consequences of registration errors.
Payer Relationship Management
While technology and process improvements drive denial management success, effective payer relationships remain critically important. Organizations that cultivate collaborative partnerships with major payers often achieve better outcomes than those maintaining purely adversarial approaches.
Strategic Communication Channels
Establishing regular communication channels with payer representatives enables proactive problem-solving rather than reactive dispute resolution. Monthly or quarterly meetings to review denial trends, discuss policy changes, and address systemic issues can prevent future denials.
Many denial management challenges stem from misunderstandings about policy requirements or documentation expectations. Direct dialogue clarifies these requirements and identifies opportunities for education that benefits both parties.
Organizations should document payer conversations and agreements to ensure consistency when appealing denials or requesting policy clarification. This documentation protects against changing interpretations and provides evidence supporting appeals.
Data-Driven Negotiation
Comprehensive denial data provides leverage in payer negotiations regarding contract terms, documentation requirements, and dispute resolution processes. Organizations that present objective evidence of denial patterns demonstrate professionalism and strengthen their negotiating position.
When specific payer policies generate disproportionate denials compared to industry benchmarks, data-driven discussions can lead to policy modifications or clarifications that reduce future friction. Payers generally prefer addressing systemic issues over processing repetitive appeals for the same problems.
Compliance and Regulatory Considerations
Denial management processes must balance revenue recovery goals with strict compliance requirements. Organizations face significant risks when appeals include inaccurate information or when prevention strategies inadvertently violate regulatory standards.
Documentation Integrity
The pressure to overturn denials never justifies documentation manipulation or misrepresentation. Organizations must establish clear policies prohibiting retrospective documentation changes solely to support appeals unless clinically appropriate and properly documented as addendums.
Compliance monitoring should include regular audits of appealed claims to verify that supporting documentation was created contemporaneously with care delivery. Patterns of documentation created specifically for appeals warrant investigation and corrective action.
Regulatory Reporting Requirements
Various regulations require healthcare organizations to track and report denial data. Understanding these requirements ensures compliance while avoiding duplicative data collection efforts that waste resources.
Organizations should integrate regulatory reporting requirements into their denial management workflows, capturing necessary data elements during routine processing rather than conducting separate data collection exercises. This integration improves efficiency while ensuring accuracy and completeness.
Outsourcing Versus In-House Management
Organizations must decide whether to manage denials internally or partner with specialized vendors. This strategic decision involves weighing cost considerations, control preferences, expertise availability, and integration requirements.
Evaluating Outsourcing Options
Denial management outsourcing can provide access to specialized expertise, scalable resources, and proven technology platforms without significant capital investment. Vendors focused exclusively on revenue cycle management often maintain deeper payer knowledge and more sophisticated analytical capabilities than individual organizations can develop independently.
However, outsourcing introduces coordination challenges, potential quality control issues, and reduced direct control over processes. Organizations must carefully evaluate vendor capabilities, cultural fit, and technology integration requirements before making outsourcing decisions.
Hybrid models combining in-house management for certain denial categories with vendor support for others offer flexibility. Organizations might retain complex or high-value denials internally while outsourcing high-volume, lower-complexity categories to vendors who can process them efficiently at scale.
Building Internal Capabilities
Organizations choosing in-house denial management gain greater control, deeper organizational knowledge, and potentially stronger integration with clinical operations. Internal teams develop expertise specific to organizational workflows and payer mix that external vendors might not replicate.
Building internal capabilities requires significant investment in staff recruitment, training, technology, and ongoing management. Organizations must assess whether they can achieve competitive performance levels compared to specialized vendors and whether denial management represents a strategic priority worthy of this investment.
Healthcare organizations partnering with experienced consultancies can accelerate internal capability development while maintaining control. This approach combines external expertise with organizational ownership, creating sustainable long-term solutions.
Future Trends Shaping Denial Management
The denial management landscape continues evolving as regulatory requirements change, payer policies shift, and technological capabilities advance. Organizations must anticipate emerging trends to position themselves for continued success.
Predictive Analytics and Prevention
The evolution from reactive denial work to predictive prevention represents the most significant trend shaping denial management. Advanced analytics identify denial risk before claim submission, enabling proactive correction rather than retrospective appeals.
Machine learning models trained on historical denial patterns can flag claims likely to face rejection based on subtle combinations of factors. This capability allows organizations to review flagged claims, correct issues, and improve first-pass acceptance rates.
Real-time decision support integrated into clinical documentation and coding workflows provides immediate feedback when documentation deficiencies or coding selections increase denial risk. This just-in-time guidance prevents errors at their source rather than discovering them after denials occur.
Value-Based Care Implications
The continued shift toward value-based payment models introduces new denial categories and complexities. Quality metric deficiencies, bundled payment reconciliations, and risk adjustment documentation requirements create denial scenarios beyond traditional fee-for-service rejections.
Organizations must expand denial management capabilities to address these emerging challenges. Traditional approaches focused solely on claim-level denials prove insufficient when value-based contracts involve retrospective reconciliations and quality-based payment adjustments.
Emerging denial categories in value-based care:
- Quality measure performance shortfalls
- Risk adjustment documentation deficiencies
- Episode payment reconciliation disputes
- Readmission penalty disagreements
- Care coordination requirement failures
Automation and Robotic Process Automation
Robotic process automation eliminates repetitive manual tasks that consume denial management staff time without adding value. Bots can automatically gather supporting documentation, prepare standard appeals, submit claims to payer portals, and update multiple systems without human intervention.
Organizations implementing RPA for denial management report significant productivity improvements, allowing staff to focus on complex cases requiring critical thinking and judgment. The technology handles routine tasks with greater speed and accuracy than manual processing.
Integration between RPA and artificial intelligence creates increasingly sophisticated automation capable of handling progressively complex scenarios. This combination represents the future of denial management, where technology manages routine work while humans focus on exceptions and strategy.
Effective denial management directly impacts healthcare organization financial performance, operational efficiency, and staff satisfaction. By implementing systematic processes, leveraging advanced technology, and prioritizing prevention alongside resolution, organizations transform denial management from a cost center into a strategic revenue optimization function. Nero and Associates, Inc. helps healthcare organizations implement comprehensive denial management solutions that combine AI-driven automation, process optimization, and performance-based consulting to maximize revenue recovery while eliminating thousands of hours of manual work.

