Healthcare revenue cycle management continues to evolve in 2026, yet one fundamental principle remains constant: the quality of your claims submission directly impacts your organization's financial health. Clean claims represent the gold standard in medical billing, serving as the cornerstone of efficient revenue collection and sustainable cash flow. Understanding what constitutes clean claims and implementing strategies to maximize their submission rate can transform your organization's financial performance while reducing administrative burden and accelerating reimbursement timelines.
Understanding Clean Claims in Healthcare Revenue Cycle Management
A clean claim is a medical billing submission that passes through the entire adjudication process without requiring additional information, clarification, or correction. These claims contain complete, accurate information that meets all payer requirements on the first submission, allowing for seamless processing and timely reimbursement.
The difference between clean claims and initial claim denials serves as a critical performance indicator for healthcare organizations. When a claim qualifies as clean, it flows through the payer's automated systems without triggering manual review or rejection. This efficiency translates directly into faster payment cycles and reduced administrative costs.
Key Components of Clean Claims
Patient Demographics and Insurance Information
- Correct patient name, date of birth, and contact information
- Valid insurance policy numbers and group identifiers
- Accurate coverage period and authorization details
- Current contact information for all parties
Provider and Facility Data
- National Provider Identifier (NPI) numbers
- Tax identification numbers
- Place of service codes
- Rendering and referring provider information
Clinical Documentation
- Appropriate diagnosis codes (ICD-10-CM)
- Procedure codes (CPT/HCPCS)
- Medical necessity documentation
- Supporting clinical notes when required
Organizations that focus on these foundational elements position themselves for stronger financial outcomes and operational efficiency.
The Financial Impact of Clean Claims Submission
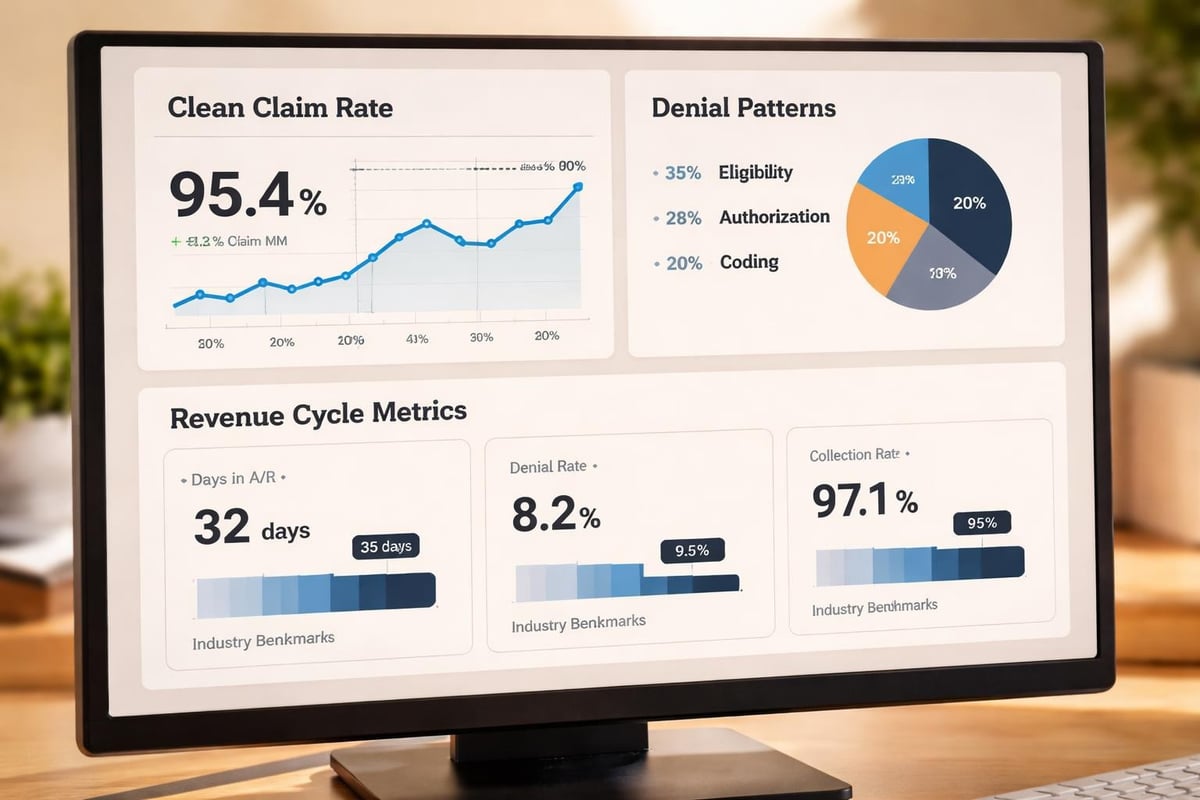
The clean claim rate serves as one of the most powerful metrics in healthcare revenue cycle management. Calculating clean claim rate involves dividing the number of claims paid on first submission by the total claims submitted, then multiplying by one hundred to express as a percentage.
Industry benchmarks suggest that high-performing organizations achieve clean claim rates above ninety-five percent. However, many healthcare providers struggle to reach this threshold, leaving significant revenue and efficiency gains on the table.
| Performance Level | Clean Claim Rate | Typical Impact |
|---|---|---|
| Optimal | 95-99% | Maximum cash flow, minimal rework |
| Strong | 90-94% | Good performance, room for improvement |
| Average | 85-89% | Moderate delays, increased costs |
| Needs Improvement | Below 85% | Significant revenue delays, high overhead |
Each percentage point improvement in clean claim rates translates to measurable financial benefits. Organizations reduce staff time spent on claim rework, accelerate cash collection, and minimize the risk of claim denials becoming write-offs.
Cost Implications of Claim Rework
When claims fail to qualify as clean on first submission, they trigger a cascade of costly activities. Staff must research the issue, gather missing information, communicate with providers or patients, correct the claim, and resubmit. This process can cost between twenty-five and fifty dollars per claim in administrative overhead alone.
The delayed revenue compounds these costs. Clean claims typically receive payment within fourteen to thirty days, while problematic claims may take sixty to ninety days or longer. This extended timeline strains working capital and may require organizations to rely on credit lines or other financing mechanisms.
Best Practices for Maximizing Clean Claims Submission
Achieving consistently high clean claim rates requires a systematic approach that addresses people, processes, and technology. Organizations must examine their entire revenue cycle workflow and identify opportunities for improvement at every touchpoint.
Front-End Revenue Cycle Optimization
The foundation of clean claims begins before the patient encounter. Best practices for preventing claim rejections emphasize the critical importance of accurate data capture at registration.
Registration Process Enhancement
- Verify insurance eligibility and benefits in real-time
- Collect complete and accurate demographic information
- Obtain required authorizations before service delivery
- Confirm patient financial responsibility and payment policies
- Document any special billing requirements or limitations
Staff training plays a vital role in front-end success. Registration personnel must understand not just what information to collect, but why each data element matters to the claims process. This knowledge transforms data collection from a rote task into a strategic revenue cycle activity.
Technology Integration and Automation
Modern revenue cycle management relies heavily on technology solutions that reduce manual processes and human error. Organizations implementing advanced systems see measurable improvements in clean claim rates.
Eligibility verification systems automate insurance coverage checks, flagging potential issues before services are rendered. These solutions integrate with scheduling systems to verify coverage at the time of appointment booking, allowing sufficient time to resolve discrepancies.
Claim scrubbing technology represents another powerful tool in the clean claims arsenal. These systems analyze claims against payer-specific rules before submission, identifying errors that would trigger rejections or denials. By catching issues proactively, organizations can correct problems and maintain their clean claim submission rates.
At Nero and Associates, Inc., we help organizations implement artificial intelligence and automation solutions that eliminate thousands of hours of manual revenue cycle processes while improving accuracy and outcomes.

Coding Excellence and Clinical Documentation
Medical coding accuracy directly influences whether claims qualify as clean upon submission. Even minor coding errors can trigger claim rejections or denials, disrupting cash flow and increasing administrative costs.
Ensuring Coding Accuracy
Clean claim rate benchmarks and best practices highlight the importance of strong coding practices and regular audits. Organizations should implement comprehensive coding quality programs that include:
- Regular coder education on coding updates and payer requirements
- Peer review processes to identify and correct patterns
- Automated coding assistance tools
- Specialty-specific coding expertise when needed
- Clear communication channels between coders and clinical staff
The relationship between clinical documentation and coding cannot be overstated. Physicians and other providers must document services with sufficient detail and specificity to support accurate code assignment. Incomplete or vague documentation forces coders to make assumptions or query providers, delaying claims submission.
Medical Necessity and Supporting Documentation
Payers require claims to demonstrate medical necessity for the services billed. This requirement means that diagnosis codes must appropriately support the procedures performed. When these elements align correctly, claims pass through as clean submissions.
Organizations should develop documentation improvement programs that educate clinical staff on payer requirements. These initiatives bridge the gap between clinical practice and billing requirements, resulting in cleaner claims and fewer denials related to medical necessity.
Payer-Specific Requirements and Relationship Management
Each insurance payer maintains unique claim submission requirements, and successful organizations adapt their processes accordingly. Understanding and accommodating these variations is essential for maintaining high clean claim rates across all payer types.
Managing Payer Complexity
Commercial Payers
- Network participation requirements
- Authorization protocols
- Timely filing limits
- Specific modifier usage rules
Government Programs
- Medicare coding guidelines and local coverage determinations
- Medicaid state-specific requirements
- Compliance with federal regulations
- Special reporting requirements
Workers' Compensation
- First report of injury documentation
- Causality relationships
- Fee schedule adherence
- State-specific forms and processes
Organizations benefit from maintaining detailed payer requirement documentation and training staff on these nuances. Some providers assign dedicated personnel to manage relationships with major payers, ensuring smooth communication and rapid resolution of any claim issues.
Strategies to maximize reimbursements through clean claims emphasize the value of proactive payer relationship management. Regular communication with payer representatives helps organizations stay current on policy changes and resolve systemic issues that might affect claim acceptance rates.
Monitoring Performance and Continuous Improvement
Achieving excellence in clean claims submission requires ongoing measurement, analysis, and refinement. Organizations must establish robust monitoring systems that track performance and identify improvement opportunities.
Key Performance Indicators
| Metric | Definition | Target |
|---|---|---|
| Clean Claim Rate | First-pass acceptance percentage | Above 95% |
| Days in A/R | Average collection timeline | Below 30 days |
| Denial Rate | Percentage of claims denied | Below 5% |
| Net Collection Rate | Revenue collected vs. expected | Above 95% |
These metrics provide a comprehensive view of revenue cycle health. When monitored regularly and analyzed thoughtfully, they reveal patterns and trends that guide improvement initiatives.
Root Cause Analysis
When clean claim rates fall below target levels, organizations must investigate the underlying causes. Common issues include:
- Registration errors in patient demographics or insurance information
- Coding inaccuracies or incomplete documentation
- Missing authorizations or referrals
- Billing system configuration problems
- Lack of knowledge about payer-specific requirements
Systematic root cause analysis identifies whether problems stem from individual performance issues, process gaps, or technology limitations. This understanding enables targeted interventions that address the actual source of the problem rather than symptoms.
Staff Training and Organizational Culture
Technology and processes provide the framework for clean claims success, but people ultimately determine outcomes. Organizations must invest in comprehensive staff development programs that build knowledge and reinforce the importance of accuracy.
Building Revenue Cycle Competency
Effective training programs address both technical skills and conceptual understanding. Staff need to know not just how to perform tasks, but why accuracy matters and how their work affects organizational outcomes. This deeper understanding fosters engagement and accountability.
Training Components
- Initial onboarding covering fundamental revenue cycle concepts
- Role-specific technical training on systems and processes
- Regular updates on payer requirement changes
- Quality feedback sessions highlighting performance trends
- Cross-functional education promoting understanding across departments
Organizations that excel at clean claims submission cultivate a culture where accuracy is valued and celebrated. They recognize high performers, share success stories, and create accountability for quality outcomes.
For organizations across small and medium-sized businesses to enterprise operations, building this culture requires intentional leadership and consistent reinforcement of quality standards.
The Role of Clearinghouses and Technology Partners
Many healthcare organizations leverage clearinghouses and technology partners to enhance their clean claims submission rates. These intermediaries provide valuable services that catch errors and optimize claims before they reach payers.
Clearinghouses offer claim scrubbing services that apply payer-specific rules to identify potential rejection issues. They also provide real-time eligibility verification, batch claim submissions, and electronic remittance processing. By centralizing these functions, clearinghouses help organizations manage the complexity of multiple payer relationships.
However, organizations should view clearinghouses as tools that complement rather than replace internal quality processes. The most successful providers maintain strong internal controls while leveraging external partners for additional validation and efficiency.
Financial and Operational Benefits Beyond Payment Speed
While faster reimbursement represents the most obvious benefit of clean claims, organizations realize numerous additional advantages. Understanding what clean claims mean and how to achieve them reveals these broader organizational benefits.
Reduced Administrative Burden
Clean claims require minimal staff intervention after submission. This efficiency allows revenue cycle teams to focus on higher-value activities like denial management, payer contracting, and strategic improvement initiatives rather than repetitive claim rework.
Improved Cash Flow Predictability
When the majority of claims process cleanly on first submission, organizations can forecast cash flow with greater accuracy. This predictability supports better financial planning and reduces reliance on credit facilities to manage operational cash needs.
Enhanced Payer Relationships
Consistently submitting clean claims builds credibility with payers and may result in preferential treatment when issues do arise. Payers recognize organizations that demonstrate operational excellence and may expedite payments or provide additional support.
Staff Satisfaction and Retention
Revenue cycle staff experience less frustration when working in environments with strong clean claim rates. Reduced rework and clearer processes contribute to job satisfaction, which in turn supports retention in an industry facing widespread workforce challenges.
Organizations exploring ways to recover underpaid claims find that strong clean claim practices create a solid foundation for identifying and pursuing legitimate underpayments.
Integration with Broader Revenue Cycle Strategy
Clean claims submission does not exist in isolation but rather forms one component of a comprehensive revenue cycle management strategy. Organizations must consider how clean claims practices integrate with other critical functions.
Patient financial clearance processes set the stage for clean claims by ensuring patients understand their financial obligations and payment options. Strong financial counseling reduces the likelihood of patient-responsibility denials and improves overall collection rates.
Denial management programs complement clean claims initiatives by analyzing rejected claims to identify systemic issues. Insights from denial analysis inform process improvements that prevent future problems and elevate clean claim rates.
Contract management ensures that fee schedules and reimbursement rates align with payer agreements. When combined with clean claims practices, effective contract management maximizes revenue capture and identifies underpayment opportunities.
The consulting solutions for healthcare revenue cycle management offered by experienced firms help organizations develop integrated strategies that optimize all revenue cycle components simultaneously.
Emerging Trends and Future Considerations
The healthcare revenue cycle landscape continues to evolve, with several trends shaping the future of clean claims management. Organizations that anticipate these changes position themselves for sustained success.
Artificial Intelligence and Machine Learning
Advanced AI systems analyze historical claim data to predict which claims may face rejection or denial. These predictive models allow organizations to proactively address issues before submission, further improving clean claim rates.
Machine learning algorithms continuously refine their accuracy based on actual outcomes, becoming more effective over time. As these technologies mature, they will play an increasingly central role in revenue cycle operations.
Value-Based Payment Models
The ongoing shift toward value-based reimbursement changes the nature of clean claims. Organizations must adapt their processes to handle quality metrics, episode-based payments, and risk-sharing arrangements while maintaining traditional fee-for-service billing for other payers.
Interoperability and Data Exchange
Enhanced data exchange between providers, payers, and patients promises to reduce errors and improve claim accuracy. As interoperability standards mature, organizations will benefit from more seamless information flow and reduced manual data entry.
Regulatory Changes
Healthcare regulations continue evolving, requiring organizations to adapt their processes accordingly. Staying current with regulatory requirements and implementing changes quickly helps maintain clean claim rates despite shifting compliance landscapes.
Clean claims represent far more than an operational metric; they embody the efficiency and excellence that drive sustainable healthcare operations. By focusing on accurate data collection, robust technology implementation, comprehensive staff training, and continuous process improvement, organizations can achieve clean claim rates that accelerate cash flow, reduce administrative costs, and support financial stability. Nero and Associates, Inc. partners with healthcare organizations to implement revenue cycle management solutions that eliminate manual processes, increase operational efficiency, and improve bottom-line performance through proven automation and integration strategies.

