Clinical documentation serves as the foundation of healthcare delivery, capturing every patient interaction, treatment decision, and outcome in a format that supports quality care, regulatory compliance, and financial sustainability. As healthcare organizations face increasing pressure to demonstrate value while managing costs, the quality and accuracy of clinical documentation has never been more critical. In 2026, the intersection of documentation practices with artificial intelligence, automation, and revenue cycle management creates unprecedented opportunities for organizations willing to modernize their approach.
The Critical Role of Clinical Documentation in Modern Healthcare
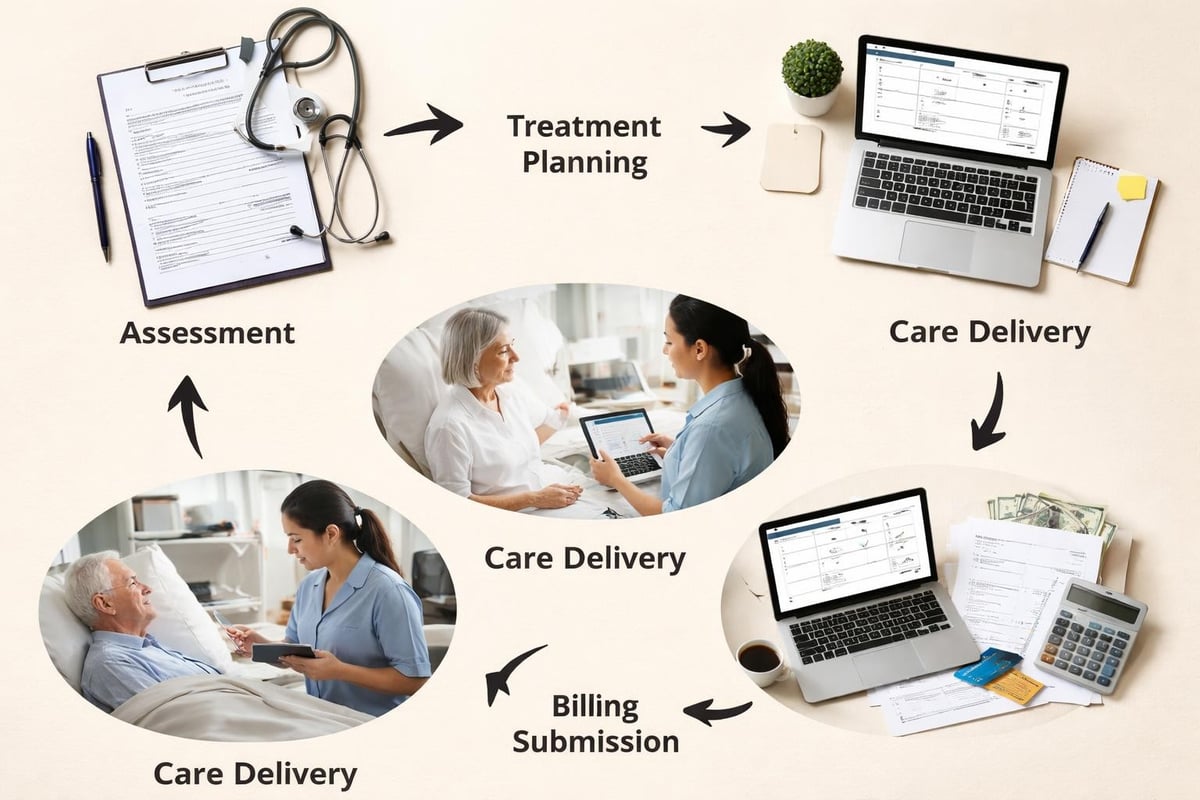
Clinical documentation represents far more than simple record-keeping. It functions as the primary communication tool among healthcare providers, the legal record of care delivery, and the foundation for reimbursement. When executed properly, comprehensive documentation supports continuity of care, reduces medical errors, and provides the data necessary for quality improvement initiatives.
The Agency for Healthcare Research and Quality provides research-backed insights into how clinical documentation technologies can reduce administrative burden while improving patient outcomes. Healthcare organizations that invest in robust documentation systems position themselves to capture accurate reimbursement, defend against liability claims, and meet increasingly stringent regulatory requirements.
Key functions of clinical documentation include:
- Supporting clinical decision-making through comprehensive patient histories
- Enabling accurate coding and billing for services rendered
- Providing legal protection for providers and organizations
- Facilitating research and quality improvement initiatives
- Ensuring compliance with federal and state regulations
- Communicating critical information across care teams
Documentation Standards and Compliance Requirements
Healthcare organizations must navigate a complex landscape of documentation requirements that span multiple regulatory frameworks. The Centers for Medicare and Medicaid Services establishes baseline expectations, while specialty-specific organizations and state licensing boards add additional layers of requirements. Understanding these standards is essential for healthcare organizations focused on financial and operational excellence.
The AAPC’s Clinical Documentation Reference Guide emphasizes that accurate documentation must be timely, complete, and specific enough to support the level of service billed. Documentation deficiencies can result in claim denials, audit findings, and significant revenue loss.
| Documentation Standard | Primary Focus | Key Requirement |
|---|---|---|
| CMS Guidelines | Medicare/Medicaid billing | Medical necessity justification |
| Joint Commission | Patient safety | Accuracy and completeness |
| HIPAA | Privacy protection | Secure access controls |
| Meaningful Use | EHR implementation | Structured data capture |
| Specialty Board Requirements | Clinical quality | Evidence-based protocols |
Optimizing Clinical Documentation for Revenue Cycle Performance
The relationship between clinical documentation quality and revenue cycle outcomes cannot be overstated. Every claim submission depends on documentation that accurately reflects the complexity of care provided, the medical necessity of services, and compliance with payer-specific requirements. In 2026, healthcare organizations lose billions annually to preventable documentation errors.
Revenue cycle management success begins at the point of care. Physicians and clinical staff must understand how their documentation choices directly impact reimbursement. Vague or incomplete notes result in downcoded claims, while missing elements trigger denials that require costly appeals processes.
Common Documentation Deficiencies That Impact Revenue
Clinical documentation improvement programs consistently identify recurring patterns of deficiencies that undermine revenue capture:
- Insufficient specificity in diagnosis documentation, preventing assignment of the most accurate ICD-10 codes
- Missing links between diagnoses and treatment plans, raising questions about medical necessity
- Incomplete procedure descriptions that fail to justify the level of service billed
- Absent or inadequate documentation of complications, comorbidities, and severity indicators
- Timing gaps between service delivery and documentation completion
Organizations implementing systematic documentation improvement see measurable improvements in case mix index, reduced denial rates, and accelerated cash flow. The key lies in creating feedback loops that educate clinicians about documentation's financial impact while streamlining the documentation process itself.
Modern revenue cycle solutions leverage natural language processing and artificial intelligence to flag potential documentation gaps in real-time. These tools analyze clinical notes as they're created, alerting providers to missing elements before the encounter is closed. This proactive approach prevents denials rather than reacting to them after submission.
Leveraging Technology to Reduce Documentation Burden
The administrative burden of clinical documentation has reached crisis levels, contributing significantly to provider burnout and reducing time available for direct patient care. Studies consistently show that physicians spend nearly two hours on documentation tasks for every hour of patient contact. This imbalance undermines the core mission of healthcare while creating inefficiencies that impact organizational performance.
Artificial intelligence and automation technologies offer transformative potential for addressing documentation burden. Ambient documentation systems capture natural clinical conversations, automatically generating structured notes that require only physician review and approval. Speech recognition technology has matured beyond simple dictation to context-aware systems that understand medical terminology and suggest appropriate phrases.
Automation and Integration Solutions
Organizations that eliminate thousands of hours of manual processes through strategic automation investments see measurable improvements in provider satisfaction, documentation quality, and operational efficiency. The key lies in selecting technologies that integrate seamlessly with existing electronic health record systems while supporting clinical workflows rather than disrupting them.
Effective documentation automation strategies include:
- Template optimization that captures required elements without excessive clicking
- Voice recognition systems tailored to specialty-specific vocabularies
- Smart forms that populate based on previous entries and clinical context
- Integration between clinical and billing systems to ensure documentation supports coding
- Mobile documentation solutions that enable note completion at the point of care
Research from the National Center for Biotechnology Information emphasizes standardized medical definitions as critical for interoperability between documentation systems. When clinical data flows seamlessly from documentation to coding to billing, organizations reduce errors while accelerating revenue realization.
| Technology Solution | Primary Benefit | Implementation Consideration |
|---|---|---|
| Ambient AI Documentation | Reduces documentation time by 60-70% | Requires workflow adaptation |
| Advanced NLP Tools | Improves coding accuracy | Integration with existing EHR essential |
| Mobile Documentation | Enables real-time note completion | Security protocols critical |
| Template Libraries | Ensures completeness | Must allow for customization |
| CDI Software | Identifies improvement opportunities | Requires staff training |
Clinical Documentation Improvement Programs
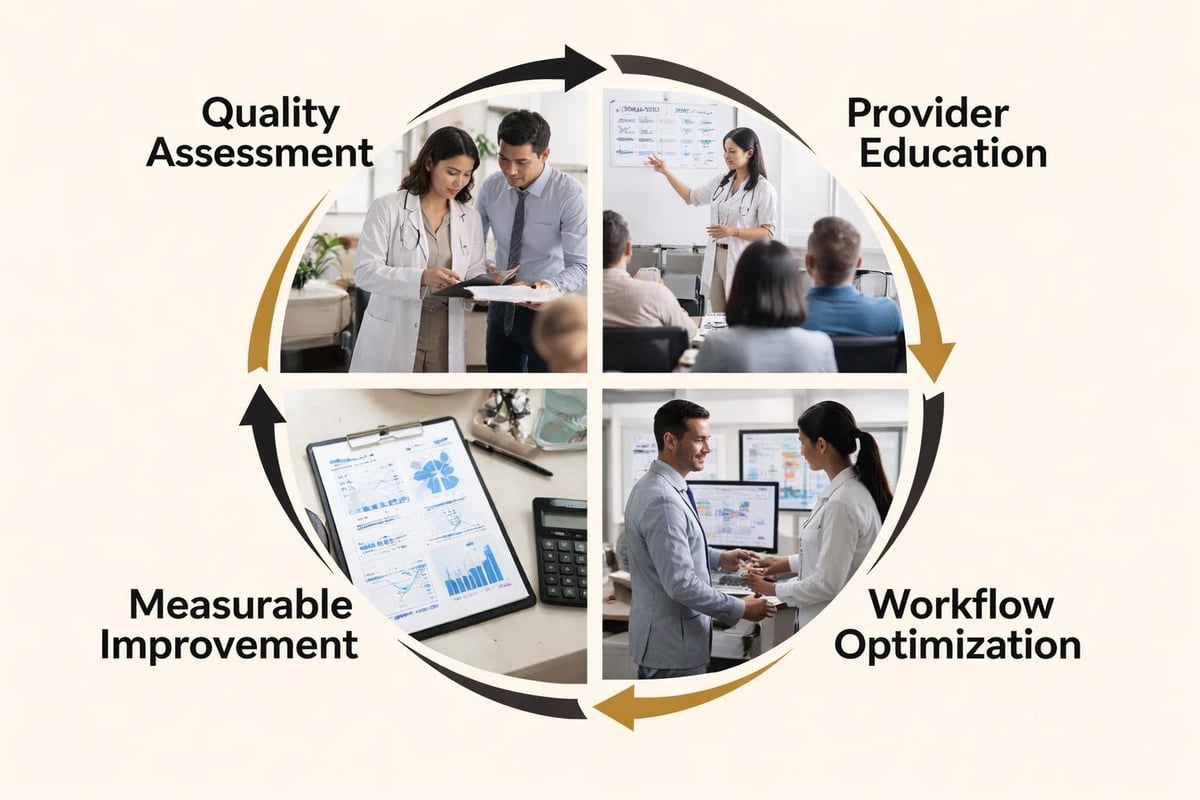
Structured clinical documentation improvement programs create systematic approaches to elevating documentation quality across entire organizations. These programs typically combine technology solutions, provider education, and ongoing monitoring to drive sustainable improvement.
Successful CDI programs assign dedicated specialists to review documentation, identify gaps, and query providers for clarification before claims submission. This concurrent review model prevents denials while educating clinicians about documentation best practices through immediate, specific feedback.
Building a CDI Program That Delivers Results
The most effective clinical documentation improvement initiatives align clinical, financial, and operational stakeholders around shared goals. Rather than positioning documentation as primarily a revenue concern, successful programs emphasize how improved documentation supports better patient care through enhanced communication and more accurate problem lists.
Implementation begins with baseline assessment. Organizations must understand their current state before setting improvement targets. Key metrics include:
- Query rate and response time
- Denial rate by documentation deficiency type
- Case mix index trends
- Documentation completion timeliness
- Provider-specific documentation patterns
Following baseline establishment, CDI programs typically roll out in phases, beginning with high-volume services or specialties with significant documentation challenges. This focused approach allows teams to refine processes before expanding organization-wide.
Provider engagement represents the most critical success factor. Clinicians must understand why documentation matters and how improved practices benefit their patients. Wolters Kluwer’s Documentation in Action resources provide practical examples that help clinicians connect documentation choices to patient outcomes.

Training and Education Strategies for Documentation Excellence
Even the most sophisticated technology solutions cannot compensate for lack of provider understanding about documentation requirements and best practices. Comprehensive training programs must address both the technical aspects of documentation and the underlying clinical reasoning that supports accurate representation of patient complexity.
Documentation basics as outlined by Upstate Medical University emphasize that effective clinical notes must be factual, accurate, complete, timely, and reflective of the patient's current status. These fundamental principles apply regardless of specialty or practice setting.
Training approaches should vary based on role and experience level. New providers require foundational education about documentation standards, while experienced clinicians benefit more from focused training on specific deficiency patterns identified through their documentation reviews.
Effective Educational Methodologies
- Case-based learning that presents real documentation examples with discussion of strengths and weaknesses
- Comparative analysis showing how different documentation approaches impact coding and reimbursement
- Specialty-specific workshops addressing unique documentation requirements for different service lines
- Regular feedback sessions reviewing individual provider metrics and improvement opportunities
- Peer learning forums where high-performing documenters share effective strategies
Organizations should measure training effectiveness through pre- and post-education documentation quality assessments. Tracking metrics like query rates, documentation completeness scores, and coding accuracy provides objective evidence of improvement and identifies providers requiring additional support.
The Future of Clinical Documentation in 2026 and Beyond
The clinical documentation landscape continues to evolve rapidly as artificial intelligence capabilities expand and regulatory requirements become more sophisticated. Recent research, including studies on AI-generated medical notes using the PDQI-9 framework, demonstrates that machine-generated documentation is approaching human quality in many contexts.
However, technology alone cannot solve documentation challenges. The most successful organizations in 2026 combine advanced tools with strong governance structures, comprehensive training programs, and cultures that value documentation quality as integral to excellent patient care.
Emerging trends shaping clinical documentation include:
- Predictive analytics that identify high-risk documentation patterns before they result in denials
- Natural language generation that creates draft documentation from structured data inputs
- Voice-first interfaces that eliminate keyboard and mouse interaction during documentation
- Blockchain-based verification ensuring documentation integrity and preventing tampering
- Interoperability advances enabling seamless documentation sharing across health systems
Organizations positioning themselves for future success invest now in documentation infrastructure, recognizing that quality documentation serves as both a defensive necessity and a competitive advantage.
Measuring and Monitoring Documentation Quality
What gets measured gets managed. Organizations serious about documentation improvement implement comprehensive metrics programs that track quality indicators across multiple dimensions. These measurement frameworks provide the data necessary to identify improvement opportunities, track progress, and demonstrate value from documentation initiatives.
Critical documentation quality metrics include:
| Metric Category | Specific Indicators | Target Benchmark |
|---|---|---|
| Completeness | Required elements present | 98%+ |
| Timeliness | Notes completed within 24 hours | 95%+ |
| Specificity | ICD-10 codes to highest specificity | 90%+ |
| Accuracy | Agreement between documentation and coding | 95%+ |
| Compliance | Query response rate | 90%+ |
| Financial | Clean claim rate | 95%+ |
Regular reporting cycles ensure visibility into documentation performance at individual, department, and organizational levels. Dashboard tools provide at-a-glance status updates while detailed reports enable deep-dive analysis of concerning trends.
The American Academy of Family Physicians offers evidence-based resources that support efficient documentation practices, helping organizations establish realistic benchmarks based on specialty and practice type.
Effective measurement programs balance accountability with support. Rather than using metrics punitively, leading organizations frame documentation performance as a development opportunity, providing resources and coaching to help providers improve.
Integrating Documentation Into Broader Operational Excellence
Clinical documentation cannot be optimized in isolation. It connects to virtually every aspect of healthcare operations, from scheduling and registration through discharge and follow-up care. Organizations achieving documentation excellence recognize these interdependencies and address documentation improvement as part of comprehensive operational transformation.
Enterprise organizations turning scale into advantage leverage centralized documentation standards, shared technology platforms, and cross-facility learning to drive consistency and efficiency. This systematic approach prevents duplication of effort while accelerating the spread of best practices.
Integration opportunities exist throughout the care continuum. Pre-visit planning tools ensure documentation begins with complete patient histories. During encounters, clinical decision support systems suggest documentation elements based on presenting symptoms and planned interventions. Post-visit, automated coding suggestions based on documentation content streamline the transition from clinical to revenue cycle operations.
Human capital management strategies must address documentation requirements during hiring, onboarding, and ongoing performance management. Job descriptions should specify documentation expectations, new employee orientation must include comprehensive documentation training, and performance reviews should incorporate documentation quality metrics alongside clinical outcomes.
Organizations that view documentation holistically rather than as an isolated clinical task create sustainable competitive advantages. They reduce costs through decreased denials and appeals, save time through automated documentation workflows, and improve outcomes through better clinical communication-the core promise of transformation-focused consulting approaches.
Optimizing clinical documentation requires balancing clinical quality, operational efficiency, and financial performance through strategic technology investments, comprehensive training, and systematic measurement. Organizations seeking to transform their documentation practices while achieving broader operational excellence benefit from partnering with experienced consultants who understand healthcare's unique challenges. Nero and Associates, Inc. helps healthcare organizations implement performance-based solutions that eliminate manual processes, increase revenue capture, and create sustainable documentation improvement-delivering measurable results that impact your bottom line while supporting your mission of exceptional patient care.

