As the healthcare landscape transforms at an unprecedented pace, physician groups find themselves at the core of delivering high-quality care in 2026. Yet, navigating the demands of multidisciplinary teams and emerging technology can feel overwhelming.
This comprehensive guide is designed to help physician groups understand, adapt, and lead effectively in this dynamic environment. Inside, you will discover the latest team structures, integration strategies, technology trends, patient engagement approaches, and compliance essentials.
Ready to enhance collaboration, boost patient outcomes, and drive efficiency? Use this guide as your trusted roadmap for success in the evolving world of healthcare teams.
The Evolving Structure of Physician Groups in 2026
Physician groups in 2026 continue to transform rapidly, adapting to new care models, expanding roles, and evolving leadership structures. Understanding these changes is essential for thriving in a complex healthcare environment.

Key Roles within Modern Physician Groups
Modern physician groups rely on a diverse set of professionals. Core roles include physicians, nurse practitioners, physician assistants, care coordinators, and administrative staff. In recent years, there has been a notable rise in non-physician providers, expanding their scope of practice and responsibilities.
Behavioral health specialists are now routinely integrated into primary care teams, improving access to mental health services. According to a 2024 AMA report, nurse practitioners and physician assistants comprise over 30% of clinical staff in physician groups. This shift impacts workflow, allowing for more comprehensive care delivery and increased patient access.
Team-based care models have become the standard, ensuring every member contributes to patient outcomes. The evolving composition of physician groups supports a more holistic, patient-centered approach.
Multidisciplinary and Cross-Functional Teams
The growth of multidisciplinary teams is reshaping how physician groups operate. These teams blend expertise from primary care, specialty medicine, pharmacy, social work, and IT professionals. Such integration fosters collaborative problem-solving and more effective chronic disease management.
For example, teams focused on chronic disease often include both clinical and social support roles, ensuring medical needs are addressed alongside social determinants of health. This structure has led to improved patient outcomes and higher satisfaction rates.
Despite these benefits, physician groups must address challenges like communication barriers and role clarity. Clear protocols and regular team meetings help ensure everyone understands their responsibilities and can contribute fully.
Centralized vs. Decentralized Team Models
Physician groups are increasingly evaluating whether centralized or decentralized team structures best fit their needs. Centralized models consolidate decision-making and processes, often suiting large health systems with multiple locations. Decentralized models empower local teams, providing flexibility and faster response to unique community needs.
Independent practices and rural physician groups often favor decentralized models to remain agile. According to a 2025 MGMA survey, 60% of large groups are now shifting toward hybrid structures that blend centralized oversight with decentralized execution. For more insights on how operational strategies are evolving, the 2026 US Health Care Outlook offers valuable context.
Choosing the right model allows physician groups to optimize resource allocation, streamline workflows, and enhance patient care.
Leadership and Governance Trends
Leadership structures in physician groups are also evolving. Traditionally, many groups have been physician-led, but administrator-led and shared governance models are gaining traction. This change reflects the increasing complexity of healthcare operations.
Emerging leadership roles, such as Chief Medical Information Officer (CMIO) and Chief Wellness Officer (CWO), are now essential. These leaders focus on technology integration and staff well-being, respectively. Inclusive decision-making, with input from all team members, has proven to improve both staff retention and organizational performance.
Collaborative leadership enables physician groups to adapt quickly and support their teams through ongoing changes in the healthcare landscape.
Team Dynamics and Communication
Strong team dynamics and communication are vital to the success of physician groups. Regular team huddles, standardized communication protocols, and the use of digital collaboration tools foster transparency and efficiency.
Secure messaging platforms and daily check-ins help bridge gaps among geographically dispersed teams. Effective conflict resolution strategies, such as structured feedback sessions, maintain a positive work environment.
Ultimately, the culture within physician groups directly impacts team performance, patient outcomes, and staff satisfaction. By prioritizing open communication and continuous improvement, these organizations can thrive amid ongoing change.
Technology Integration for Enhanced Team Performance
Adopting advanced technology is no longer optional for physician groups. In 2026, technology drives team efficiency, care quality, and patient engagement. The right integration strategy empowers physician groups to collaborate across disciplines, enhance workflows, and stay compliant in a rapidly changing landscape.
Electronic Health Records (EHR) and Interoperability
Electronic Health Records are now the backbone of physician groups’ operations. In 2026, most EHR platforms enable seamless data sharing, supporting real-time access to patient information across specialties. Interoperability standards have expanded, making care coordination more effective and reducing delays.
For example, specialists can instantly review primary care notes, lab results, and medication histories without waiting for manual transfers. According to the 2025 ONC report, 85% of physician groups now use interoperable EHRs, dramatically improving both workflow and patient safety. These advances make it easier for teams to provide consistent, high-quality care.
Artificial Intelligence and Automation in Clinical Workflows
Artificial intelligence and automation are transforming how physician groups manage clinical and administrative tasks. AI-driven tools support diagnostic decisions, automate scheduling, and predict patient risks. For instance, urgent care centers use AI triage tools to quickly direct patients to the right level of care, reducing wait times and errors.
Automation lessens the administrative burden and increases accuracy in documentation and billing. To further streamline operations, many physician groups leverage AI automation integration solutions that connect disparate systems and automate routine tasks. These improvements free up providers to focus on patient care.
Telehealth and Virtual Collaboration Tools
Telehealth has become a cornerstone of care delivery for physician groups. The post-pandemic surge in virtual services continues, with video consultations, remote patient monitoring, and secure messaging now standard. Teams use virtual tumor boards to collaborate on complex oncology cases, regardless of physical location.
Between 2020 and 2025, telehealth adoption jumped by 300%. This rapid growth enables physician groups to expand access, especially in rural or underserved areas. Virtual collaboration tools also support daily team huddles and real-time updates, fostering stronger communication and quicker decision-making.
Data Security and Compliance
Protecting patient data is a top priority for physician groups in 2026. With evolving HIPAA rules and new privacy regulations, compliance requires robust security measures. Best practices include multi-factor authentication, encrypted communications, and detailed audit trails to monitor access.
Breaches can harm both reputation and operations. Physician groups implement strict protocols for data access and regularly train staff on security awareness. By prioritizing compliance, groups maintain patient trust and avoid costly penalties, ensuring that technology integration does not compromise confidentiality.
Training and Change Management
Continuous training is essential as physician groups adopt new technologies. Staff must stay updated on EHR functionalities, telehealth platforms, and security protocols. Effective change management strategies, such as designating peer-led tech champions, help teams navigate transitions smoothly.
Feedback loops and ongoing support are critical for sustained success. Physician groups that invest in regular training sessions and encourage open dialogue see higher adoption rates and fewer disruptions. This commitment to learning ensures that technology enhances, rather than hinders, team performance.
Step-by-Step Guide: Optimizing Team Collaboration in Physician Groups
Optimizing collaboration in physician groups is essential for delivering efficient, high-quality care. This practical, step-by-step guide provides actionable strategies to help physician groups transform their team dynamics, streamline workflows, and achieve better patient outcomes.
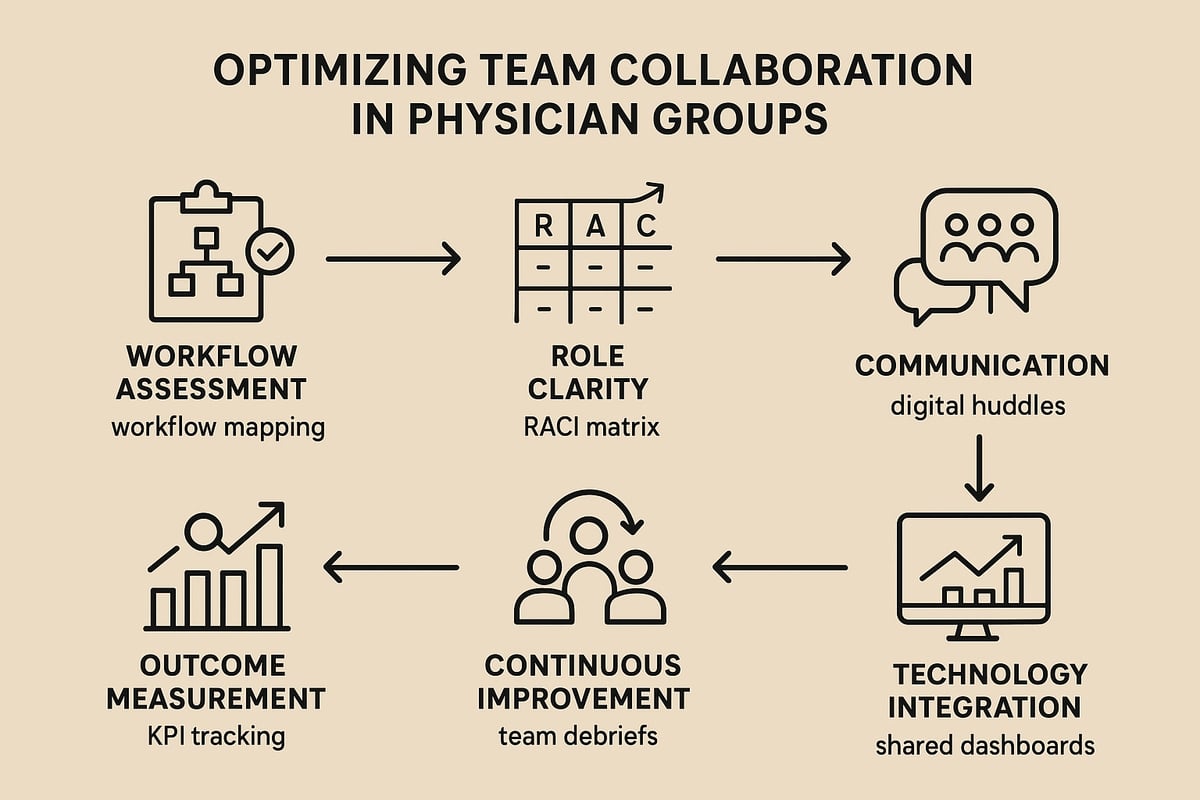
Step 1: Assess Current Team Structure and Workflow
Begin by evaluating how your physician groups currently operate. Conduct internal audits to review roles, responsibilities, and processes. Use workflow mapping tools to visualize patient movement through the system.
Identify bottlenecks and inefficiencies that slow down care or create confusion. For example, time-motion studies in outpatient clinics can reveal where delays occur most frequently.
- Map out every team member's daily tasks
- Document handoff points between staff
- Gather feedback from providers and support staff
This foundational step ensures physician groups have a clear picture of their starting point, setting the stage for meaningful improvements.
Step 2: Define Clear Roles and Responsibilities
Effective physician groups rely on well-defined roles. Establish detailed job descriptions and accountability charts so each team member understands expectations. Use a RACI matrix to clarify who is Responsible, Accountable, Consulted, and Informed for every major process.
Regularly review and update these descriptions to adapt to evolving care models. Reducing overlap and clarifying reporting lines helps teams avoid confusion and duplication of effort.
- Create visual org charts
- Assign primary and backup roles for critical tasks
- Schedule periodic role review meetings
Clarity in responsibilities enables physician groups to function more cohesively and efficiently.
Step 3: Implement Effective Communication Protocols
Strong communication is the backbone of successful physician groups. Standardize handoffs, huddles, and documentation practices to ensure consistency. Leverage secure messaging platforms for real-time updates and urgent issues.
Daily virtual team check-ins can foster alignment and address concerns quickly. Monitor the effectiveness of communication protocols through feedback and periodic audits.
- Use structured templates for shift handoffs
- Schedule brief daily huddles
- Encourage transparent, respectful dialogue
Consistent communication practices help physician groups minimize errors and improve patient care coordination.
Step 4: Leverage Technology for Coordination
Integrating technology is vital for modern physician groups. Combine EHR, scheduling, and telehealth tools to streamline coordination. Automate routine tasks to free up provider time for patient care.
For example, shared dashboards allow all team members to view patient status updates in real time. Regularly evaluate your tech stack to ensure it meets evolving needs.
Explore strategies for healthcare financial and operational excellence to maximize your group's efficiency and impact.
- Implement interoperable EHR systems
- Use automated reminders for appointments
- Track technology adoption and user satisfaction
Smart technology choices empower physician groups to deliver seamless, coordinated care.
Step 5: Foster a Culture of Continuous Improvement
Encourage a mindset of ongoing growth within physician groups. Solicit feedback from team members and patients to identify areas for improvement. Launch quality initiatives that address specific challenges or goals.
Monthly team debriefs with actionable metrics create opportunities for reflection and learning. Recognize and reward collaborative behaviors to reinforce a positive culture.
- Facilitate open forums for suggestions
- Share progress updates on improvement projects
- Celebrate team achievements publicly
A culture of improvement keeps physician groups adaptive and resilient in a changing healthcare environment.
Step 6: Measure Outcomes and Adjust Strategies
Tracking performance is essential for physician groups striving for excellence. Monitor key performance indicators such as patient satisfaction, care outcomes, and team engagement. Use data analytics to identify trends and benchmark against national standards.
Adjust strategies based on the results you observe. For example, if benchmarking reveals gaps in patient satisfaction, implement targeted interventions and reassess regularly.
- Set clear, measurable goals
- Review data in monthly or quarterly meetings
- Iterate on processes to close performance gaps
By measuring and refining their efforts, physician groups can ensure sustained collaboration and superior patient care.
Patient Engagement and Experience in Physician Group Settings
In 2026, patient engagement has become a defining factor for the success of physician groups. As healthcare becomes more collaborative, the ability to deliver a personalized, responsive, and inclusive experience is essential. Physician groups that prioritize engagement strategies not only boost patient satisfaction but also drive better clinical outcomes.
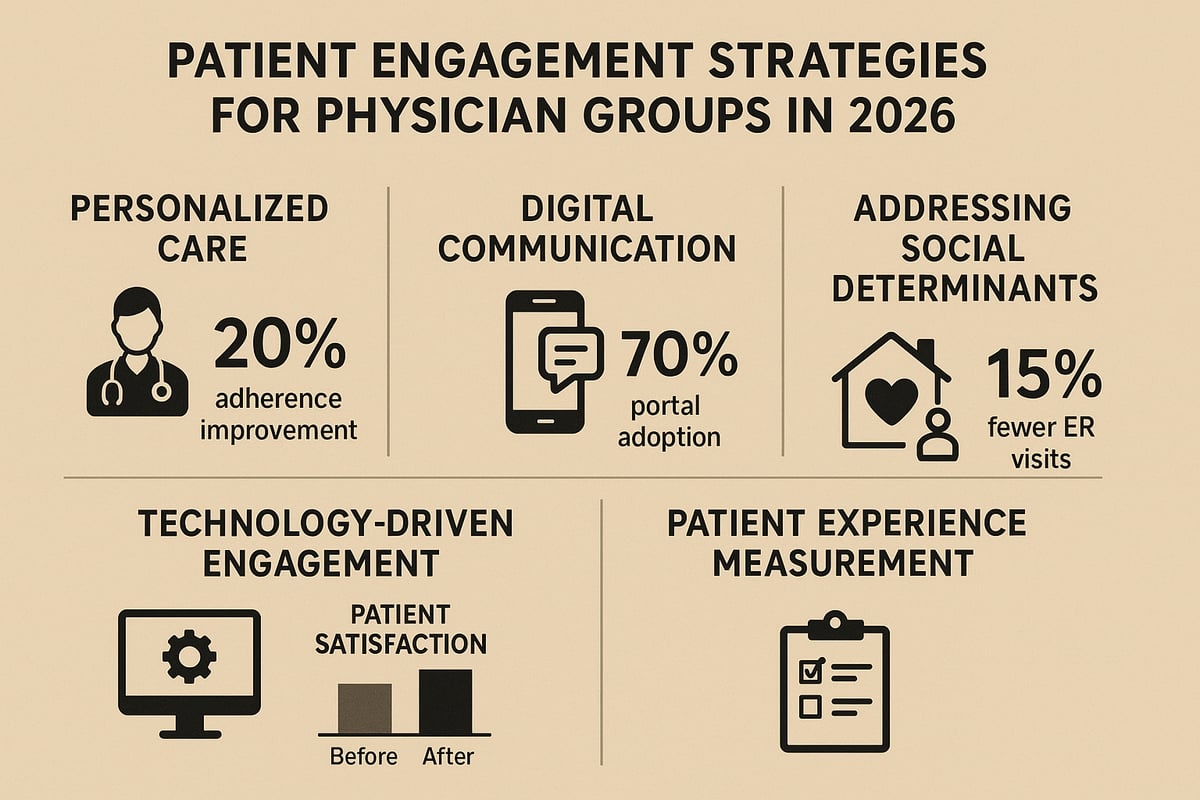
Personalized Care and Shared Decision-Making
Personalized care remains a cornerstone for physician groups aiming to deliver exceptional patient experiences. By adopting shared decision-making tools, such as digital decision aids and interactive patient portals, these groups empower individuals to take an active role in their treatment plans. For example, customized care plans for chronic disease management not only improve adherence but also foster trust between patients and providers.
According to a 2025 NEJM study, shared decision-making increased medication adherence by 20 percent. Physician groups that embed these practices into daily workflows see measurable improvements in both satisfaction and health outcomes.
Enhancing Communication with Patients
Effective communication is critical for physician groups striving to build lasting patient relationships. Digital communication tools, like automated text reminders and telehealth follow-ups, streamline appointment scheduling and care coordination. Multilingual messaging and accessible communication strategies further reduce barriers for diverse populations.
In many communities, patient navigator roles have emerged to guide individuals through complex care journeys. This approach has helped physician groups decrease no-show rates and elevate overall patient satisfaction.
Integrating Social Determinants of Health (SDOH)
Addressing social determinants of health is now a routine part of care for leading physician groups. Teams systematically screen for factors like housing, food security, and transportation. By forming partnerships with local organizations, physician groups connect patients to essential resources.
For instance, onsite social workers can intervene when patients face housing or food insecurity. Data shows that these SDOH interventions have reduced emergency room visits by 15 percent, underscoring their value in comprehensive care delivery.
Technology-Driven Patient Engagement
Technology continues to transform how physician groups engage with their patients. The widespread use of mobile apps, wearable devices, and remote monitoring tools enables real-time data sharing and personalized feedback. Patient feedback tools, such as instant surveys within patient portals, provide immediate insights into service quality.
Notably, patient portal adoption now exceeds 70 percent in 2026, making digital touchpoints a standard expectation. For more on the technology shaping this evolution, explore Healthcare Technology Trends 2026. Physician groups leveraging these platforms can respond quickly to patient needs and enhance ongoing engagement.
Measuring and Improving Patient Experience
Continuous measurement is vital for physician groups seeking to refine patient experience. Standardized surveys, like CAHPS, offer a benchmark for satisfaction and identify improvement areas. Real-time feedback loops, including rapid response teams for addressing complaints, ensure concerns are resolved promptly.
Physician groups routinely analyze patient data to drive quality initiatives. By acting on feedback and tracking outcomes, they create a culture of continuous improvement that resonates with patients and staff alike.
Regulatory, Financial, and Compliance Considerations for Physician Groups
Navigating the regulatory, financial, and compliance landscape is crucial for physician groups in 2026. With shifting policies and evolving payment models, staying informed and proactive helps ensure operational stability and growth. The following sections break down essential areas every group needs to master.
Evolving Regulatory Landscape in 2026
Physician groups face a dynamic regulatory environment in 2026. Key regulations now include value-based care mandates, MACRA updates, and new interoperability requirements. The Centers for Medicare and Medicaid Services (CMS) has introduced updated reporting standards that require enhanced documentation and data transparency.
To stay compliant, physician groups should:
- Monitor CMS updates regularly
- Develop annual compliance checklists
- Train staff on new reporting tools
Staying ahead of these changes protects accreditation status and reimbursement eligibility.
Financial Management and Revenue Cycle Optimization
Effective financial management is a top priority for physician groups. Maximizing reimbursements and reducing claim denials require accurate coding, detailed documentation, and proactive follow-up. Revenue cycle automation now helps reduce accounts receivable (A/R) days by 20 percent, boosting cash flow.
Many groups leverage end-to-end revenue cycle management solutions to streamline billing, track underpayments, and ensure compliance with payer requirements. Regular audits and technology upgrades further support financial health.
Quality Metrics and Value-Based Care
Tracking and reporting quality metrics is essential for physician groups operating in a value-based care environment. Most contracts now tie at least 60 percent of group revenue to quality outcomes rather than volume.
To align with these models, groups should focus on:
- Monitoring clinical performance indicators
- Implementing bundled payment models
- Using benchmarking data to compare outcomes
These steps help physician groups demonstrate value, improve patient care, and secure favorable reimbursement rates.
Risk Management and Legal Compliance
Risk management is integral to the operations of physician groups. Addressing malpractice risk, ensuring thorough documentation, and maintaining informed consent protocols reduce legal exposure. Proactive risk assessments, regular staff training, and up-to-date policies are critical for ongoing compliance.
Non-compliance can threaten both accreditation and payment streams. Physician groups that prioritize legal safeguards and transparent practices maintain trust with patients and regulatory bodies.
The Future of Physician Groups: Trends and Predictions for 2026
The healthcare environment is transforming rapidly, and physician groups are at the forefront of this change. Looking ahead to 2026, several emerging trends are shaping how these groups operate, collaborate, and deliver care. Understanding these developments is essential for leaders aiming to stay competitive and resilient.
Workforce Trends and Physician Well-Being
Physician groups are prioritizing clinician well-being more than ever. Flexible work arrangements, such as team-based scheduling, are now standard in many organizations. The role of Chief Wellness Officer has become common, highlighting a focus on mental health and work-life balance. According to the 2025 Medscape survey, burnout rates are declining when teams offer strong peer support. Evolving roles like the physician advisor are also shaping workforce dynamics. For more insight, explore the Physician Advisor Trends 2026 to see how these advisors support both quality and compliance within physician groups.
Expansion of Integrated, Value-Driven Care
The shift toward value-based care continues to accelerate for physician groups. Participation in Accountable Care Organizations and clinically integrated networks is on the rise, now reaching 45 percent of groups. These models encourage cross-specialty collaboration and focus on population health management. Physician groups are developing streamlined care pathways for complex patients, improving both outcomes and financial performance. This integrated approach rewards proactive care and supports long-term patient relationships.
Advanced Analytics and Predictive Modeling
Physician groups are adopting advanced analytics to enhance decision-making and patient management. Big data and artificial intelligence tools are increasingly used for population health, risk stratification, and resource optimization. Predictive modeling is especially valuable for identifying patients at risk for hospital readmission or disease progression. Studies show that analytics adoption can increase return on investment by 18 percent in group practices. Tools that blend automation with clinician oversight, such as Human-in-the-Loop Report Generation, are becoming more common in chronic disease management, ensuring accuracy and efficiency.
Patient-Centered Innovations and Digital Health
Digital health is revolutionizing how physician groups engage with patients. Remote patient monitoring, digital therapeutics, and personalized medicine are now integral to care delivery. Genomics and pharmacogenomics are helping tailor medication management to each patient’s unique profile. Patient portals and mobile apps are used by over 70 percent of patients, enabling ongoing communication and self-management. As technology and care delivery continue to converge, physician groups are well positioned to lead these innovative changes and enhance patient experience.
As you look ahead to 2026, navigating the evolving dynamics of physician groups and healthcare teams can feel daunting—but you don’t have to do it alone. We’ve explored how integrating technology, optimizing team roles, and focusing on employee well-being can transform both care quality and your organization’s bottom line. If you want to apply these strategies, streamline your processes, and empower your teams for the future, let’s connect. I invite you to Book a Consultation so we can tailor solutions that fit your unique challenges and help you lead with confidence.

