Pre-certification represents a critical checkpoint in healthcare operations and various business processes where approval must be obtained before delivering services or initiating procedures. This verification mechanism protects both providers and patients while ensuring that resources are allocated appropriately and reimbursement processes flow smoothly. Organizations that master pre-certification workflows experience fewer claim denials, accelerated revenue cycles, and improved operational efficiency across their service delivery models.
Understanding the Pre-Certification Process
Pre-certification serves as a proactive approval mechanism that confirms medical necessity and coverage eligibility before services are rendered. Healthcare revenue cycle management relies heavily on this process to secure payer commitment prior to treatment, reducing the risk of unexpected denials that can devastate cash flow and operational planning.
The fundamental purpose extends beyond simple authorization. Organizations implementing robust pre-certification protocols create predictability in their revenue streams while protecting patients from surprise billing situations. This verification step ensures that all stakeholders understand coverage parameters, financial responsibilities, and service scope before resources are committed.
Key Components of Effective Pre-Certification
Multiple elements converge to create a successful pre-certification framework:
- Clinical documentation supporting medical necessity and treatment rationale
- Insurance verification confirming active coverage and benefit eligibility
- Procedure coding ensuring accurate representation of planned services
- Timeline management meeting payer-specific submission deadlines
- Follow-up protocols tracking approval status and addressing delays
Each component requires dedicated attention and systematic execution. Organizations that treat pre-certification as an integrated workflow rather than isolated tasks achieve significantly better approval rates and faster turnaround times.
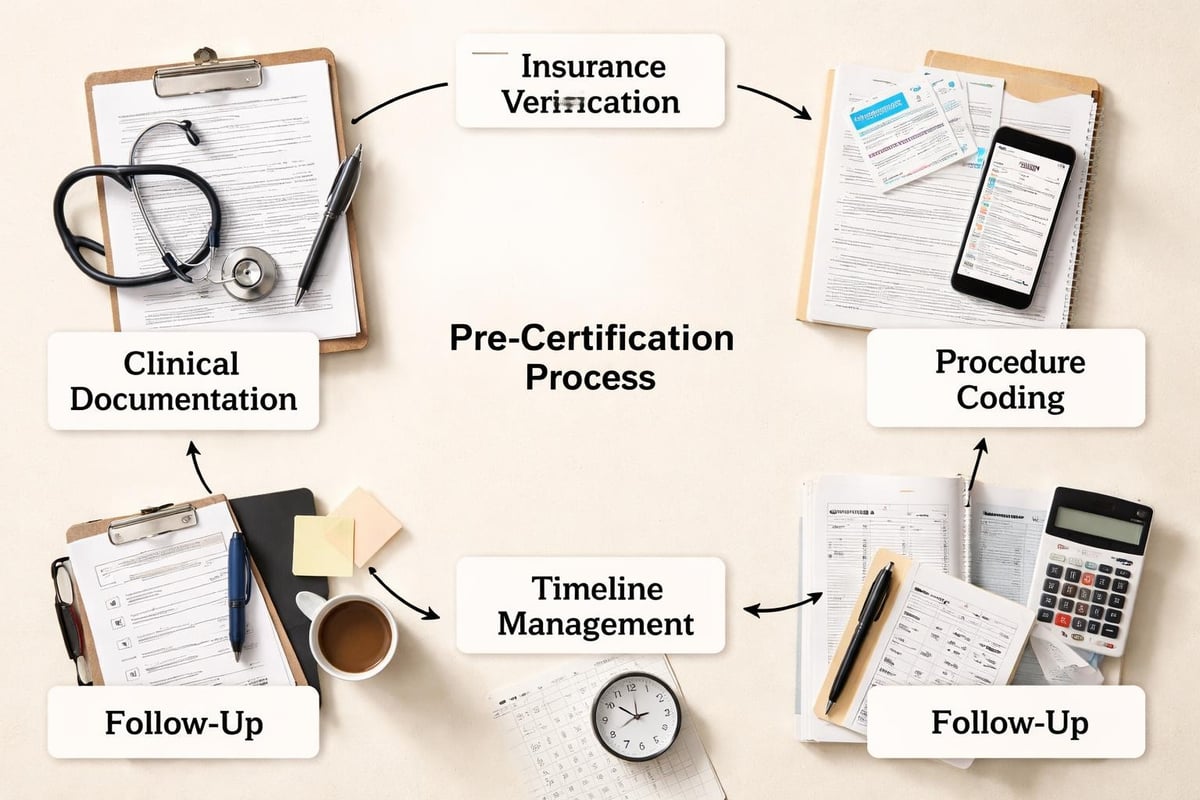
Pre-Certification in Healthcare Revenue Cycle Management
Healthcare providers face unique challenges where pre-certification directly impacts financial viability. Prior authorization requirements vary significantly across payers, creating complexity that demands specialized expertise and systematic processes.
Revenue cycle performance hinges on obtaining timely approvals. Delayed or denied pre-certifications create downstream complications including postponed procedures, patient dissatisfaction, and revenue recognition delays. Organizations serving healthcare organizations must prioritize this function to maintain operational health.
Common Pre-Certification Scenarios
Different clinical situations trigger specific pre-certification requirements:
- Elective surgical procedures requiring advance approval for hospital admission
- High-cost diagnostic imaging including MRI, CT, and PET scans
- Specialty medications particularly biologics and infusion therapies
- Durable medical equipment such as wheelchairs, oxygen systems, and prosthetics
- Mental health services including intensive outpatient and residential treatment
Pre-admission certification represents a particularly critical subset for planned inpatient stays. Failure to obtain this approval can result in complete claim denial, leaving providers without reimbursement for substantial service delivery costs.
| Pre-Certification Type | Typical Timeframe | Denial Risk if Skipped | Revenue Impact |
|---|---|---|---|
| Elective Surgery | 3-5 business days | High (80-90%) | $15,000-$50,000+ |
| Advanced Imaging | 24-48 hours | Medium-High (60-75%) | $1,500-$5,000 |
| Specialty Drugs | 5-10 business days | Very High (90%+) | $3,000-$25,000 |
| DME Equipment | 3-7 business days | Medium (50-65%) | $500-$5,000 |
Automation and Technology Solutions
Manual pre-certification processes consume thousands of employee hours annually while introducing error rates that compromise approval success. Modern organizations leverage technology to transform this bottleneck into a competitive advantage.
Artificial intelligence and automation platforms can validate insurance eligibility, cross-reference procedure codes against payer policies, and automatically submit authorization requests through electronic channels. These systems reduce submission time from hours to minutes while improving accuracy rates beyond what manual processes can achieve.
Building an Automated Pre-Certification Workflow
Strategic automation deployment follows a structured approach:
- Data integration connecting electronic health records with payer portals
- Rules engines applying payer-specific requirements automatically
- Status tracking monitoring authorization requests through approval
- Exception handling flagging complex cases requiring human intervention
- Analytics dashboards identifying bottlenecks and optimization opportunities
Organizations implementing comprehensive automation report 60-80% reductions in processing time and 40-50% improvements in first-pass approval rates. The efficiency gains translate directly to bottom-line improvements through faster revenue recognition and reduced administrative overhead.

Regulatory Compliance and Documentation Standards
Pre-certification exists within a complex regulatory framework that varies by state, payer, and service category. State regulations like Missouri's medical pre-certification requirements establish mandatory compliance standards for specific programs and procedures.
Maintaining current knowledge of regulatory requirements demands continuous education and systematic policy updates. Organizations must monitor changes across multiple jurisdictions and payer networks, incorporating new requirements into workflows before they take effect.
Documentation Best Practices
Successful pre-certification approvals depend on comprehensive, accurate documentation:
- Complete patient demographics including current insurance information
- Detailed clinical narratives explaining medical necessity
- Supporting diagnostic data such as lab results and imaging reports
- Treatment history demonstrating prior interventions attempted
- Provider credentials confirming specialist qualifications when required
Insufficient documentation represents the leading cause of pre-certification delays and denials. Providers who implement standardized templates and checklists achieve significantly higher approval rates while reducing back-and-forth communication that extends timelines.
Pre-Certification Beyond Healthcare
While healthcare represents the most prominent pre-certification application, other industries employ similar approval mechanisms. Professional services firms seeking government contracts often navigate precertification requirements that verify capabilities, financial stability, and regulatory compliance before bid eligibility.
Construction, engineering, and consulting organizations serving enterprise clients encounter pre-qualification processes that assess technical capabilities, safety records, and financial capacity. These evaluations mirror healthcare pre-certification in their requirement for comprehensive documentation and adherence to specific criteria.
Cross-Industry Pre-Certification Principles
Common success factors transcend industry boundaries:
| Success Factor | Healthcare Application | Professional Services Application |
|---|---|---|
| Early initiation | Submit requests before scheduling | Begin application well before RFP deadlines |
| Complete documentation | Clinical records and necessity justification | Capability statements and past performance |
| Payer knowledge | Understanding insurance policies | Researching client requirements |
| Status tracking | Following up on pending authorizations | Monitoring application progress |
| Appeals readiness | Preparing denial responses | Addressing qualification concerns |
Organizations operating across multiple sectors can leverage pre-certification expertise from one domain to strengthen processes in another. The systematic approach, attention to documentation, and proactive communication apply universally.
Financial Impact and Performance Metrics
Effective pre-certification management delivers measurable financial benefits that extend beyond avoiding denials. Organizations tracking key performance indicators identify optimization opportunities and quantify return on investment for process improvements.
Revenue acceleration represents perhaps the most significant benefit. When pre-certification approvals are obtained before service delivery, billing can proceed immediately following care completion. This eliminates the waiting period while retrospective authorization is pursued, improving cash flow by 15-30 days on average.
Tracking Pre-Certification Performance
Critical metrics for monitoring effectiveness include:
- Approval rate (target: 95%+ on first submission)
- Average processing time (measured from submission to decision)
- Denial rate and primary denial reasons
- Appeal success rate for overturned denials
- Staff time per authorization across different service types
- Revenue impact of delayed or denied pre-certifications
Small and medium businesses often lack dedicated pre-certification staff, forcing clinical and administrative personnel to handle authorizations alongside other responsibilities. This fragmented approach creates inefficiency and inconsistency that metrics can expose and improvement initiatives can address.

Training and Staff Development
Pre-certification expertise doesn't emerge automatically. Organizations must invest in systematic training that develops both technical knowledge and process discipline among team members responsible for authorization management.
Effective training programs cover payer-specific requirements, coding fundamentals, clinical documentation standards, and communication protocols. Staff members need to understand not just what information to submit, but why payers require specific data points and how to present clinical narratives persuasively.
Building Pre-Certification Competency
A comprehensive training approach includes:
- Foundational education on insurance principles and authorization concepts
- Payer-specific modules addressing individual insurance company requirements
- Hands-on practice with actual authorization scenarios and case studies
- Ongoing updates as requirements change and new policies emerge
- Performance coaching providing feedback on approval rates and documentation quality
Organizations implementing structured training programs report 25-40% improvements in authorization efficiency and reduced staff turnover as team members develop valuable specialized skills. Cross-training creates backup capability that prevents bottlenecks when key personnel are unavailable.
Integration with Broader Business Operations
Pre-certification cannot function effectively in isolation. The process must integrate seamlessly with scheduling systems, electronic health records, billing platforms, and patient communication channels to maximize efficiency and minimize errors.
System integration eliminates duplicate data entry that introduces errors and consumes staff time. When patient scheduling automatically triggers insurance verification and pre-certification initiation, the workflow becomes proactive rather than reactive. This integration particularly benefits hospitality sector organizations managing employee health benefits alongside operational demands.
Creating Workflow Synergy
Strategic integration points include:
- Patient registration capturing complete insurance information at first contact
- Appointment scheduling flagging services requiring pre-certification before confirmation
- Clinical documentation ensuring required information is captured during encounters
- Billing systems preventing claim submission without verified authorization
- Patient portals providing transparency about authorization status and requirements
Technology platforms that connect these systems create end-to-end visibility and accountability. Staff members can identify authorization gaps before they cause service delays, and management can monitor pipeline health across the organization.
Managing Denials and Appeals
Despite best efforts, pre-certification denials occur. Organizations need systematic approaches for analyzing denial patterns, preparing compelling appeals, and learning from unsuccessful requests to prevent future occurrences.
The appeals process requires escalated documentation standards and often peer-to-peer clinical discussions between requesting providers and medical directors at insurance companies. Success depends on thorough preparation, clear articulation of medical necessity, and persistence through multiple appeal levels when appropriate.
Denial Management Framework
Effective denial response includes:
| Appeal Stage | Timeframe | Success Rate | Required Actions |
|---|---|---|---|
| First Level | 30-60 days | 30-40% | Submit additional documentation |
| Peer Review | 15-30 days | 40-50% | Schedule physician-to-physician discussion |
| Second Level | 30-60 days | 20-30% | Present comprehensive clinical rationale |
| External Review | 60-90 days | 30-40% | Independent medical review |
Organizations should calculate the cost-benefit of pursuing appeals based on service value, likelihood of success, and staff resources required. Not every denial warrants appeal, but high-value cases deserve aggressive pursuit through available channels.
Payer Relationships and Communication
Strong relationships with insurance company representatives and medical directors facilitate smoother pre-certification processes. Regular communication helps providers understand evolving requirements and enables problem-solving before situations escalate to formal denials.
Proactive payer engagement includes participating in provider education sessions, attending policy update webinars, and establishing direct contacts for complex authorization scenarios. These relationships prove particularly valuable when time-sensitive situations require expedited review or when clinical situations don't fit standard policy templates.
Building Effective Payer Partnerships
Relationship strategies include:
- Regular communication through designated payer representatives
- Policy compliance demonstrating respect for payer requirements
- Documentation excellence reducing back-and-forth requests for information
- Constructive feedback highlighting policy areas creating unnecessary barriers
- Collaborative problem-solving when unique clinical situations arise
Organizations recognized as reliable partners often receive more favorable treatment during authorization reviews and faster processing for routine requests. This reputation develops through consistent demonstration of clinical quality and administrative competence.
Future Trends in Pre-Certification
The pre-certification landscape continues evolving as technology advances and payers seek efficiency improvements. Artificial intelligence applications increasingly handle routine authorization decisions automatically, while blockchain technology promises transparent, real-time verification of coverage and approvals.
Predictive analytics will enable organizations to identify services likely requiring pre-certification before scheduling occurs, initiating workflows proactively. Machine learning algorithms will analyze historical denial patterns to strengthen documentation for cases at higher risk of rejection.
Regulatory pressure may eventually standardize pre-certification requirements across payers, reducing the complexity organizations currently navigate. Federal initiatives exploring specialized laboratory testing authorization standardization indicate movement toward greater consistency, though full harmonization remains years away.
Organizations positioning themselves for these changes invest in flexible technology platforms that can adapt to new requirements, staff training that emphasizes critical thinking over rote process execution, and data analytics capabilities that drive continuous improvement. Those treating pre-certification as a strategic capability rather than administrative burden will maintain competitive advantages as the landscape transforms.
Pre-certification excellence requires systematic processes, technological enablement, and continuous improvement across documentation, communication, and workflow integration. Organizations that optimize authorization workflows reduce claim denials, accelerate revenue cycles, and create operational predictability that supports strategic growth. Nero and Associates, Inc. helps organizations transform pre-certification from an administrative burden into a strategic advantage through revenue cycle management solutions, process automation, and performance-based consulting that delivers measurable bottom-line impact. Contact our team to discover how we can eliminate thousands of hours from your authorization workflows while improving approval rates and financial outcomes.

