Every organization faces the risk of underpayments, whether from insurance payers, client billing discrepancies, or payroll errors. These financial gaps silently erode profitability, often going unnoticed until they accumulate into substantial losses. In 2026, businesses are increasingly recognizing that proactive underpayment recovery isn't just about reclaiming lost dollars but about establishing systematic processes that prevent future revenue leakage. For healthcare providers, professional services firms, and enterprises managing complex billing systems, understanding how to identify, document, and recover underpayments has become a critical competency that directly impacts financial sustainability and operational excellence.
Understanding the Financial Impact of Underpayments
Underpayments represent more than simple calculation errors. They reflect systemic vulnerabilities in revenue cycle management, contract enforcement, and payment reconciliation processes. Research indicates that healthcare organizations alone lose billions annually due to payer underpayments, with individual facilities often experiencing losses ranging from three to five percent of total revenue.
The hidden costs extend beyond the immediate financial shortfall:
- Staff time devoted to identifying and investigating discrepancies
- Administrative burden of appeals and documentation
- Opportunity costs from delayed revenue recognition
- Erosion of cash flow stability affecting operational planning
- Potential pattern establishment if underpayments go unchallenged
Organizations that implement end-to-end revenue cycle management solutions report significantly higher recovery rates because they establish systematic monitoring from service delivery through final payment reconciliation. The challenge isn't just finding underpayments but building infrastructure that catches them early when recovery is most achievable.
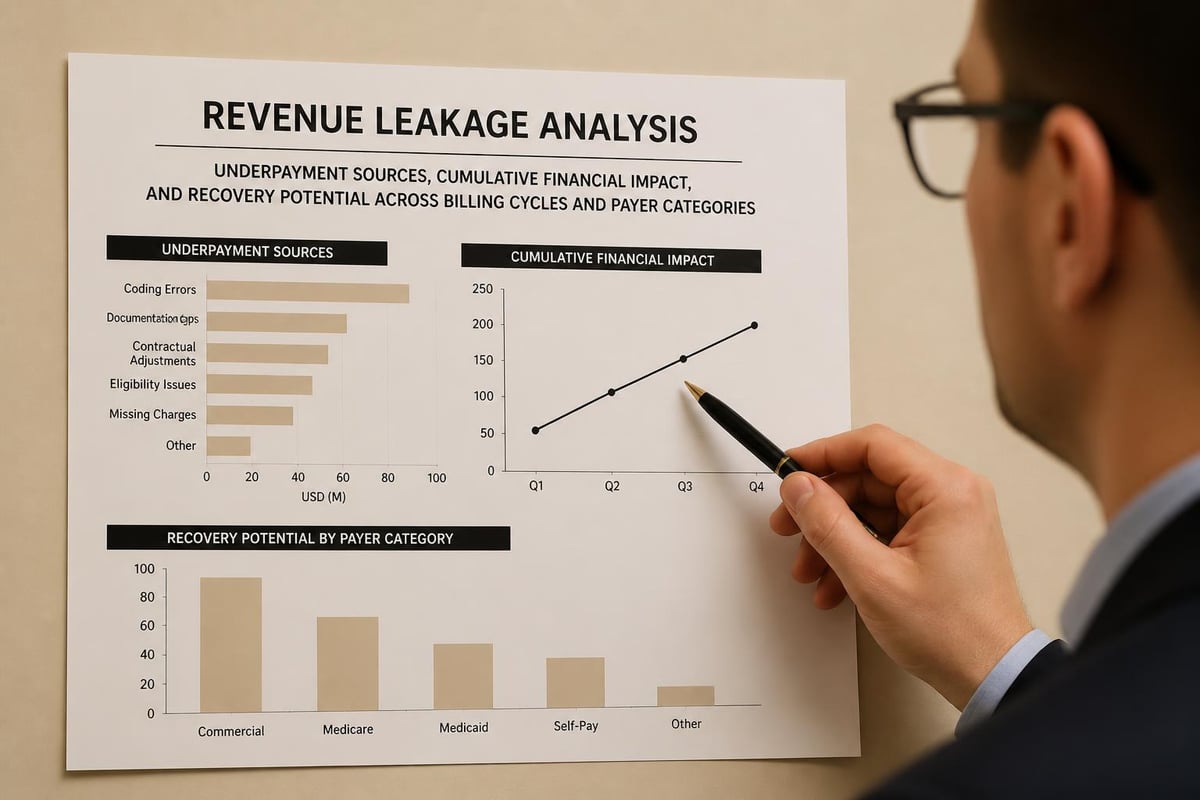
Common Sources of Underpayment Across Industries
Different sectors experience underpayments through distinct mechanisms. In healthcare, payer contract complexities and coding issues dominate. For professional services, scope creep and billable hour disputes create gaps. Manufacturing and distribution face pricing agreement violations and volume discount miscalculations.
Healthcare-specific underpayment triggers include incorrect reimbursement rates, denied or partially paid claims, bundling errors, and failure to honor contractual fee schedules. The hidden threat of underpayments often manifests through subtle contract interpretation differences that payers exploit systematically.
Professional services underpayments typically emerge from change order disputes, milestone payment disagreements, retainer misapplication, and time-and-materials calculation errors. These require meticulous documentation practices and clear contract language to resolve effectively.
Identifying Underpayments Through Systematic Analysis
Detection requires methodical comparison between expected and actual payments. Organizations must establish baseline expectations derived from contracts, fee schedules, and standard pricing agreements. Without these reference points, identifying discrepancies becomes nearly impossible.
Key identification methodologies include:
- Contract-to-payment variance analysis comparing remittance details against contractual obligations
- Historical pattern recognition flagging statistical outliers in payment amounts
- Code-level auditing verifying correct application of billing codes and modifiers
- Automated payment posting review catching system-generated errors before reconciliation
- Payer-specific trend monitoring identifying systematic underpayment patterns by source
Technology plays an increasingly vital role in 2026's underpayment recovery landscape. Machine learning algorithms can analyze thousands of transactions simultaneously, identifying subtle patterns that human reviewers miss. These systems learn from historical data to predict which claims face higher underpayment risk, allowing preemptive intervention.
| Detection Method | Effectiveness | Resource Intensity | Typical Recovery Rate |
|---|---|---|---|
| Manual review | Moderate | Very High | 45-60% |
| Rules-based automation | High | Moderate | 65-75% |
| AI-powered analysis | Very High | Low | 80-90% |
| Hybrid approach | Highest | Moderate | 85-95% |
Organizations serving healthcare facilities benefit particularly from automated detection because of the volume and complexity of claims processing. A single hospital may process tens of thousands of claims monthly, making manual review impractical for comprehensive underpayment recovery.
Building Your Underpayment Recovery Process
Successful recovery requires structured workflows that move identified underpayments from detection through resolution. The foundation begins with comprehensive documentation establishing the legitimate payment amount and proving the underpayment occurred.
Documentation Requirements
Strong documentation forms the backbone of any recovery effort. Legal requirements for underpayment documentation vary by context, but certain elements prove universally valuable. Original contracts or fee schedules, itemized service records, correspondence establishing payment terms, previous payment patterns demonstrating consistency, and payer policy manuals all strengthen recovery claims.
Healthcare providers must maintain particularly detailed records because underpayment recovery in healthcare faces stringent evidentiary standards. Claim submissions, remittance advice explanations, medical necessity documentation, prior authorization approvals, and appeals correspondence create the complete picture necessary for successful challenges.

The Appeal and Recovery Workflow
Once underpayments are identified and documented, organizations must initiate formal recovery processes. This typically begins with internal verification ensuring the underpayment is genuine rather than reflecting legitimate payment adjustments.
The standard recovery workflow progresses through these stages:
- Initial verification confirming expected payment amounts through contract review
- Informal inquiry contacting the payer for clarification before formal appeal
- First-level appeal submitting documented evidence supporting additional payment
- Escalated review requesting senior examiner or external review if denied
- Negotiated settlement exploring compromise solutions for disputed amounts
- Legal action consideration evaluating litigation for significant unresolved underpayments
Different payers maintain varying timelines and requirements for each stage. Healthcare organizations must navigate payer contracts in underpayment appeals carefully because contract language often dictates appeal procedures, timelines, and arbitration requirements. Missing a contractual deadline can forfeit recovery rights entirely.
Professional services firms often find success through direct client communication before formal processes. Building relationships with accounts payable teams facilitates resolution of honest errors without damaging client relationships or requiring expensive appeals.
Prevention Strategies to Minimize Future Underpayments
While recovery reclaims lost revenue, prevention protects margins proactively. Organizations that emphasize front-end accuracy reduce the volume of underpayments requiring later intervention.
Contract Clarity and Management
Ambiguous contract language creates underpayment opportunities. Precise definitions of deliverables, clear payment calculation methodologies, explicit milestone criteria, and unambiguous rate adjustment mechanisms eliminate interpretation disputes. When serving enterprise clients, contract precision becomes especially critical because payment volumes magnify small percentage discrepancies into substantial dollar amounts.
Regular contract audits ensure understanding remains current. Payer contracts in healthcare frequently change through amendments and policy updates. Maintaining current contract libraries and training billing staff on specific payer requirements prevents inadvertent underpayments caused by outdated information.
Technology-Enabled Prevention
Modern revenue cycle systems incorporate preventive controls that stop underpayments before they occur. Real-time eligibility verification confirms coverage details before service delivery. Automated charge capture ensures complete billing for all services rendered. Rules engines validate coding accuracy against payer-specific requirements. Predictive analytics flag high-risk claims for additional review before submission.
Integration across systems eliminates data silos that create underpayment vulnerabilities. When clinical documentation, coding, billing, and payment posting systems communicate seamlessly, information consistency reduces errors. Healthcare organizations implementing integrated platforms report underpayment reductions of twenty to thirty percent within the first year.
| Prevention Strategy | Implementation Complexity | Underpayment Reduction | ROI Timeline |
|---|---|---|---|
| Staff training | Low | 15-25% | 3-6 months |
| Contract standardization | Moderate | 20-30% | 6-12 months |
| Process automation | High | 35-50% | 12-18 months |
| AI-powered validation | Very High | 45-65% | 18-24 months |
Leveraging Performance-Based Solutions
Organizations increasingly turn to performance-based consultancies that align incentives with results. These partnerships eliminate upfront investment risk while ensuring expertise application where it generates maximum value. Unlike traditional fee-for-service arrangements, performance models tie compensation to actual underpayment recovery and prevention outcomes.
Performance-based underpayment recovery offers several advantages:
- No upfront capital investment required for sophisticated analytics tools
- Immediate access to specialized expertise without permanent headcount additions
- Scalable solutions adapting to organizational growth and complexity changes
- Risk-sharing arrangements aligning consultant and client interests
- Continuous improvement focus driven by outcome accountability
This approach particularly benefits small and mid-sized businesses lacking internal resources for comprehensive underpayment programs. Rather than choosing between accepting losses or building expensive internal capabilities, performance partnerships provide enterprise-grade solutions at proportional costs.
Measuring Recovery Program Effectiveness
Successful underpayment recovery requires quantifiable performance metrics. Organizations should track recovery rate percentages, average recovery amount per identified underpayment, time from identification to resolution, appeal success rates by payer and issue type, and prevention effectiveness through underpayment trend analysis.
Advanced programs distinguish between different recovery sources. Initial underpayments caught before payment posting cost less to resolve than those identified during reconciliation. Systematic payer issues requiring contract renegotiation demand different strategies than random processing errors. Comprehensive underpayment recovery knowledge includes understanding these distinctions and allocating resources accordingly.
Dashboard reporting provides leadership visibility into recovery program performance. Real-time metrics showing recovered amounts, outstanding appeals, and prevention impact justify continued investment while identifying improvement opportunities. Benchmarking against industry standards reveals whether internal performance meets reasonable expectations or whether external expertise could enhance results.

Addressing Wage Underpayment in Human Capital Management
Underpayment recovery extends beyond customer billing to encompass employee compensation. Wage underpayments create legal liability, damage employee morale, and expose organizations to regulatory penalties. The complexity of modern compensation including overtime calculations, shift differentials, bonus structures, and benefit valuations creates numerous error opportunities.
Understanding wage recovery and legal penalties helps organizations avoid costly mistakes. Federal and state labor laws impose strict requirements for timely, accurate wage payment. Violations trigger back pay obligations, penalty assessments, and potential litigation. In 2026, increased regulatory scrutiny and employee awareness make wage underpayment prevention more critical than ever.
Automated time and attendance systems integrated with payroll processing reduce wage underpayment risk significantly. These platforms apply complex rules consistently, maintain detailed audit trails, and flag anomalies for human review. Organizations processing payroll for hundreds or thousands of employees cannot rely on manual calculations without accepting substantial error risk.
Industry-Specific Underpayment Challenges
Different sectors face unique underpayment dynamics requiring tailored approaches. Healthcare underpayment recovery focuses heavily on payer contract enforcement and coding accuracy. Professional services emphasize change order documentation and scope definition. Hospitality industries managing employee optimization face tipping credit calculations and irregular scheduling complexities.
Healthcare Revenue Cycle Considerations
Healthcare providers navigate particularly complex underpayment landscapes. Multiple payer types including commercial insurance, Medicare, Medicaid, and self-pay patients each maintain different reimbursement methodologies. Contract negotiations establish facility-specific rates that override standard fee schedules. Medical necessity determinations affect coverage decisions. Revenue optimization strategies must account for this multidimensional complexity.
Coding accuracy directly impacts payment correctness. Diagnosis codes justify medical necessity. Procedure codes determine reimbursement amounts. Modifier application affects bundling and separate payment eligibility. Small coding errors create underpayments that multiply across hundreds of similar cases. Continuous coder education and regular auditing prevent systematic underpayment patterns from developing.
Professional Services Billing Precision
Consulting firms, legal practices, and other professional services organizations face underpayment challenges centered on time tracking accuracy, billable hour categorization, expense reimbursement documentation, and retainer application. Unlike product sales with clear unit pricing, services billing requires detailed activity documentation supporting invoiced amounts.
Scope creep represents a particular underpayment risk. When client requests expand beyond original agreements without formal change orders, professionals often deliver additional value without corresponding payment. Preventing this requires disciplined scope management, proactive client communication about out-of-scope requests, and systematic change order processes capturing additional work before delivery.
Automation and AI in Underpayment Recovery
Artificial intelligence transforms underpayment recovery from reactive investigation to proactive prevention. Machine learning models analyze payment patterns across thousands of transactions, identifying subtle anomalies indicating underpayments. Natural language processing extracts relevant details from unstructured remittance explanations. Robotic process automation handles repetitive appeal submission tasks, freeing specialized staff for complex cases.
These technologies democratize sophisticated analytics previously available only to the largest organizations. Cloud-based platforms deliver enterprise capabilities to smaller firms through subscription models eliminating capital investment barriers. Organizations can now access performance-based consultancy solutions incorporating cutting-edge technology without building internal technical expertise.
AI applications in underpayment recovery include:
- Predictive modeling identifying high-risk claims before submission
- Automated contract extraction creating searchable payment rule databases
- Pattern recognition detecting systematic payer underpayment behaviors
- Natural language generation drafting customized appeal letters
- Outcome prediction estimating appeal success probability informing pursuit decisions
The technology continues advancing rapidly. 2026 systems incorporate generative AI creating comprehensive appeal documentation from structured data inputs. Conversational interfaces allow billing staff to query underpayment databases using natural language. Integration across revenue cycle touchpoints provides holistic visibility into payment accuracy from service delivery through final reconciliation.
Underpayment recovery protects organizational financial health by reclaiming lost revenue and preventing future leakage through systematic processes, technology enablement, and performance measurement. Whether addressing healthcare payer underpayments, professional services billing discrepancies, or wage calculation errors, the fundamental principles remain consistent: detect accurately, document thoroughly, pursue persistently, and prevent proactively. Nero and Associates, Inc. helps organizations implement comprehensive underpayment recovery solutions that increase revenue, eliminate manual processes, and improve operational efficiency through performance-based consulting aligned with your success.

