Healthcare organizations face unprecedented pressure to maximize revenue while delivering exceptional patient care in an increasingly complex regulatory environment. Revenue cycle optimization has emerged as a critical strategic initiative that transforms financial operations from reactive, manual processes into proactive, automated systems that capture every dollar earned. Organizations that master this transformation not only improve their bottom line but also enhance patient satisfaction and reduce administrative burden on staff members.
Understanding the Foundation of Revenue Cycle Optimization
Revenue cycle optimization encompasses the complete financial journey of patient care, from initial appointment scheduling through final payment collection. This comprehensive approach examines every touchpoint where revenue can be captured, lost, or delayed.
The modern revenue cycle management landscape has evolved dramatically over the past decade. Traditional approaches relied heavily on manual processes, resulting in claim denials, delayed payments, and thousands of lost revenue opportunities. Today's optimization strategies leverage technology, data analytics, and process redesign to create seamless workflows that minimize friction and maximize collections.
Organizations must recognize that revenue cycle optimization is not a one-time project but an ongoing commitment to operational excellence. The most successful implementations treat it as a strategic priority that requires executive sponsorship, cross-functional collaboration, and continuous improvement.
Key Components of the Revenue Cycle
Understanding the distinct phases of the revenue cycle is essential for effective optimization. Each phase presents unique challenges and opportunities for improvement.
Front-End Operations include patient scheduling, registration, insurance verification, and authorization management. These critical first steps establish the foundation for successful revenue capture. Errors or inefficiencies at this stage cascade through the entire cycle, leading to claim denials and payment delays.
Mid-Cycle Processes encompass charge capture, coding, claim submission, and payment posting. This phase requires precise documentation and accurate coding to ensure proper reimbursement. Even minor coding errors can result in significant revenue loss or compliance issues.
Back-End Activities focus on denial management, appeals, patient collections, and final reconciliation. Organizations often overlook opportunities in this phase, leaving substantial revenue on the table due to inadequate follow-up processes.

Strategic Approaches to Revenue Cycle Optimization
Implementing effective revenue cycle optimization requires a multifaceted approach that addresses technology, processes, and people. Organizations must evaluate their current state, identify gaps, and develop a roadmap for transformation.
Automation and Technology Integration
Manual processes represent the greatest obstacle to revenue cycle efficiency. Every manual data entry point introduces the possibility of error, delay, and inconsistency. Automation eliminates these vulnerabilities while freeing staff to focus on higher-value activities.
Advanced automation solutions can handle routine tasks such as eligibility verification, claim scrubbing, and payment posting with speed and accuracy that human workers cannot match. The return on investment for these technologies often exceeds 300% within the first year of implementation.
Organizations should prioritize automation opportunities that deliver the highest impact:
- Eligibility verification systems that check insurance coverage in real-time during scheduling
- Claim scrubbing software that identifies errors before submission
- Automated payment posting that reconciles payments without manual intervention
- Denial management platforms that track patterns and trigger appropriate workflows
- Patient communication tools that send automated reminders and payment options
Artificial intelligence and machine learning capabilities have transformed revenue cycle optimization beyond basic automation. These technologies can predict claim denials before submission, identify high-risk accounts, and recommend optimal collection strategies based on historical patterns.
Front-End Process Enhancement
The adage "garbage in, garbage out" applies perfectly to revenue cycle management. Poor data quality at registration creates a cascade of problems throughout the entire cycle. Streamlining front-end processes delivers immediate improvements in clean claim rates and reduces downstream rework.
| Front-End Challenge | Optimization Strategy | Expected Improvement |
|---|---|---|
| Incomplete patient demographics | Real-time data validation tools | 40-50% reduction in errors |
| Insurance verification delays | Automated eligibility checking | 75% faster verification |
| Authorization bottlenecks | Electronic prior authorization | 60% time savings |
| Patient financial counseling gaps | Integrated estimation tools | 35% increase in upfront collections |
Implementing point-of-service collections represents one of the most effective front-end optimizations. When patients understand their financial responsibility upfront and receive convenient payment options, collection rates improve dramatically. Organizations that collect copays, deductibles, and estimated patient responsibility at the time of service typically see 30-40% higher overall collection rates.
Staff training is equally critical to front-end success. Registration team members must understand the downstream impact of their work and possess the tools and knowledge to capture accurate information consistently. Regular training updates and quality audits ensure sustained performance.
Data Analytics and Performance Monitoring
Revenue cycle optimization requires visibility into performance across all phases of the cycle. Organizations cannot improve what they do not measure. Comprehensive analytics programs provide the insights necessary for continuous improvement.
Essential Metrics and KPIs
Effective performance monitoring tracks both leading and lagging indicators. Leading indicators predict future problems and enable proactive intervention, while lagging indicators measure historical performance and outcomes.
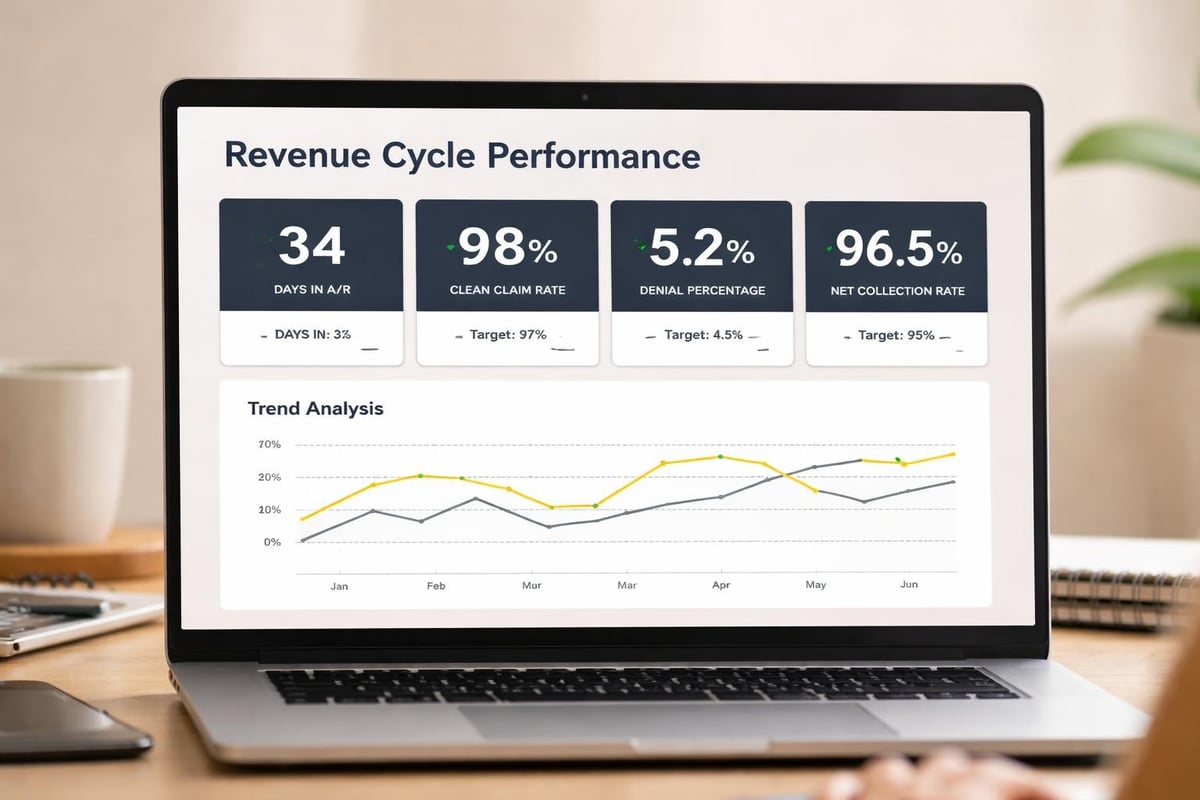
Days in Accounts Receivable (AR) remains the most fundamental revenue cycle metric. This measure indicates how quickly the organization converts services into cash. Best-in-class organizations maintain days in AR below 35, while average performers often exceed 50 days.
Clean Claim Rate measures the percentage of claims accepted on first submission without errors or rejections. Organizations should target clean claim rates above 95%. Each percentage point improvement in clean claim rate directly impacts cash flow and reduces rework costs.
Denial Rate quantifies the percentage of claims denied by payers. While some denials are inevitable, rates exceeding 5-7% indicate systemic problems requiring investigation. Implementing revenue cycle analytics helps organizations identify root causes and implement corrective actions.
Cost to collect represents the total expense of revenue cycle operations divided by total collections. This metric reveals operational efficiency and helps benchmark performance against industry standards. High-performing organizations maintain cost to collect below 3% of net patient revenue.
- Net collection rate (actual collections as percentage of expected reimbursement)
- Point-of-service cash collections
- Authorization approval rates
- Claim submission lag time
- Denial overturn rate
- Patient payment plan compliance
Leveraging Predictive Analytics
Advanced analytics capabilities transform revenue cycle optimization from reactive problem-solving to proactive risk management. Predictive models can identify claims likely to face denials, patients at high risk for non-payment, and process bottlenecks before they impact cash flow.
Machine learning algorithms analyze historical patterns to recommend optimal collection strategies for different patient segments. These tools consider factors such as payment history, demographic information, insurance type, and balance amounts to suggest personalized approaches that maximize collection rates while maintaining positive patient relationships.
Denial Management and Prevention
Claim denials represent one of the most significant revenue leakage points in healthcare organizations. Every denied claim requires additional resources to resolve, delays cash flow, and risks permanent revenue loss if not addressed promptly. Effective revenue cycle optimization transforms denial management from a reactive fire drill into a strategic prevention program.
Root Cause Analysis
Understanding why claims are denied is essential to prevention. Organizations should categorize denials and track patterns to identify systemic issues. Common denial categories include:
- Registration and eligibility issues – Incorrect patient information or insurance verification failures
- Authorization and referral problems – Missing prior authorizations or expired referrals
- Coding and documentation errors – Incorrect procedure codes or insufficient medical necessity documentation
- Timely filing failures – Claims submitted beyond payer deadlines
- Coordination of benefits issues – Incorrect primary/secondary insurance sequencing
Strategies for capturing revenue include implementing robust denial tracking systems that automatically categorize denials and assign them to appropriate resolution queues. This systematic approach ensures no denied claim falls through the cracks.
Prevention-Focused Workflows
The most effective denial management strategy is prevention. Organizations should invest resources in identifying and correcting problems before claim submission rather than dedicating staff to appeals and rework.
| Prevention Strategy | Implementation Approach | Revenue Impact |
|---|---|---|
| Pre-claim scrubbing | Automated edits checking | $150,000-$300,000 annual savings per million in revenue |
| Real-time eligibility | Point-of-service verification | 40% reduction in eligibility denials |
| Coding education | Regular training and audits | 25% improvement in coding accuracy |
| Documentation improvement | Physician feedback loops | 30% reduction in medical necessity denials |
Organizations should establish clear workflows for denied claims that include accountability, timeframes, and escalation procedures. Speed matters in denial management. Claims appealed within 30 days have significantly higher overturn rates than those delayed beyond 60 days.
Process Standardization and Best Practices
Revenue cycle optimization requires consistent processes across the organization. Variation in how different teams handle similar situations creates inefficiencies, errors, and unpredictable results. Standardization enables scaling, training, and continuous improvement.
Creating Standard Operating Procedures
Documenting best practices ensures knowledge transfer and maintains performance when staff members change roles or leave the organization. Standard operating procedures (SOPs) should cover every critical revenue cycle function, including registration protocols, charge capture workflows, coding guidelines, and collection processes.
Effective SOPs balance comprehensiveness with usability. They should be detailed enough to guide new staff members yet concise enough that experienced team members can quickly reference specific information. Visual aids, flowcharts, and decision trees enhance understanding and adoption.
Organizations should review and update SOPs regularly as payers change requirements, regulations evolve, and new technologies are implemented. Treating SOPs as living documents rather than static files ensures they remain relevant and useful.
Staff Training and Development
Technology and processes can only deliver results when operated by skilled, knowledgeable staff. Investing in comprehensive training programs pays dividends through improved performance, reduced errors, and higher employee satisfaction.
Training should extend beyond initial onboarding to include ongoing education on regulatory changes, payer requirements, technology updates, and best practice evolution. Organizations that implement regular training cadences see measurable improvements in key performance indicators.
Cross-training team members across different revenue cycle functions creates operational flexibility and deepens understanding of how individual roles impact overall performance. When registration staff understand how their work affects coding and when coders appreciate billing challenges, collaboration improves and problems get solved faster.

Technology Selection and Implementation
The revenue cycle technology landscape offers dozens of solutions claiming to solve every problem. Organizations must carefully evaluate options, select tools aligned with their specific needs, and implement them effectively to realize promised benefits.
Evaluation Criteria
Before selecting revenue cycle optimization technology, organizations should clearly define their objectives, constraints, and success criteria. Understanding current pain points and desired outcomes enables focused evaluation rather than getting distracted by impressive but irrelevant features.
Integration capabilities represent perhaps the most critical selection factor. Revenue cycle solutions must exchange data seamlessly with electronic health records, practice management systems, and other core applications. Poor integration creates data silos, manual workarounds, and defeats optimization objectives.
Scalability ensures the solution can grow with the organization without requiring replacement. Consider not only current volume but anticipated growth over a 3-5 year horizon. Solutions that perform well at lower volumes sometimes struggle when transaction counts increase significantly.
User experience directly impacts adoption and utilization. The most powerful features deliver no value if staff members find the system too complex or cumbersome to use regularly. Involve end-users in evaluation and testing to ensure solutions meet their needs.
Vendor stability and support quality matter enormously in healthcare technology. Organizations enter long-term relationships with revenue cycle technology vendors. Research the vendor's financial position, customer satisfaction ratings, and support responsiveness before committing.
Implementation Best Practices
Even the best technology fails without proper implementation. Organizations should approach revenue cycle optimization implementations as change management initiatives, not just technical projects.
Successful implementations include these critical elements:
- Executive sponsorship that demonstrates organizational commitment and removes obstacles
- Cross-functional project teams representing all affected departments and workflows
- Detailed project planning with realistic timelines and resource allocation
- Comprehensive testing using real-world scenarios before go-live
- Phased rollout approaches that manage risk and enable learning
- Robust training programs that prepare all users for new systems and workflows
- Post-implementation support that addresses issues quickly and captures lessons learned
Organizations should resist the temptation to customize solutions extensively. While some configuration is necessary, excessive customization increases implementation time, complicates upgrades, and often addresses symptoms rather than underlying process problems. Sometimes the better approach is adapting processes to align with industry best practices embedded in the software.
Integration With Broader Organizational Objectives
Revenue cycle optimization does not exist in isolation. It connects directly to broader organizational goals around patient experience, employee engagement, and operational efficiency. The most successful programs recognize and leverage these connections.
Patient Experience Considerations
Financial interactions significantly impact patient satisfaction and loyalty. Confusing bills, unexpected charges, and difficult payment processes create frustration that overshadows positive clinical experiences. Healthcare revenue cycle optimization increasingly emphasizes patient-friendly approaches that balance collection objectives with relationship preservation.
Transparent cost estimates before service delivery reduce surprise and build trust. Patients appreciate knowing their financial responsibility upfront and having time to plan for payment. Organizations that provide clear, accurate estimates see higher patient satisfaction scores and better collection rates.
Flexible payment options accommodate different patient financial situations. Offering online payment portals, automated payment plans, and multiple payment methods removes barriers to payment and demonstrates respect for patient preferences.
Clear, understandable billing statements prevent confusion and reduce call volume. Many healthcare bills confuse even financially sophisticated patients with complex coding, unexplained adjustments, and unclear balances. Investing in statement redesign that emphasizes clarity delivers measurable returns.
Organizational Efficiency Gains
Revenue cycle optimization drives efficiency improvements that extend beyond the finance department. When consulting companies implement performance-based solutions, they recognize that eliminating manual processes frees staff capacity for higher-value activities throughout the organization.
Reducing claim denials decreases workload for billing staff, clinical documentation teams, and physician advisors who support appeals. This ripple effect allows organizations to redirect resources toward growth initiatives, quality improvement, or patient access expansion.
Improved cash flow provides financial flexibility for strategic investments. Organizations no longer need to delay capital projects, technology implementations, or staff additions due to working capital constraints. Faster collections accelerate the funding cycle for organizational priorities.
Creating a Culture of Continuous Improvement
Sustainable revenue cycle optimization requires embedding continuous improvement into organizational culture. One-time projects deliver initial gains that eventually plateau or erode without ongoing attention and refinement.
Organizations should establish regular cadences for reviewing revenue cycle performance, identifying opportunities, and implementing improvements. Monthly performance reviews that engage cross-functional teams foster accountability and collaboration.
Celebrating successes reinforces desired behaviors and maintains momentum. When teams achieve clean claim rate improvements or reduce days in AR, recognize their contributions publicly and tangibly. Positive reinforcement sustains engagement far more effectively than criticism of shortfalls.
Encouraging frontline innovation taps into valuable insights from staff members closest to daily operations. Registration representatives, coders, and billing specialists often identify improvement opportunities that executives miss. Creating channels for ideas and acting on valuable suggestions builds engagement and accelerates optimization.
Benchmarking against industry standards and best performers reveals opportunities and sets aspirational targets. Organizations should participate in industry surveys and peer networks that enable performance comparison. Understanding where you rank helps prioritize improvement initiatives and justify necessary investments.
Partnering for Success
Many organizations lack the internal expertise, capacity, or technology to fully optimize their revenue cycles independently. Strategic partnerships with specialized firms can accelerate transformation and deliver capabilities beyond what's feasible to build internally.
Performance-based partnerships align incentives between organizations and their revenue cycle partners. When consultants or vendors share risk and reward based on measurable outcomes, both parties remain focused on results rather than activities. This alignment ensures proposed solutions deliver genuine value rather than impressive features that fail to improve performance.
Organizations should evaluate potential partners based on demonstrated expertise, cultural fit, and flexibility. The best partnerships feel collaborative rather than vendor-client transactional. Partners should invest time understanding unique organizational circumstances and tailoring approaches rather than applying cookie-cutter methodologies.
Revenue cycle optimization represents a critical strategic priority for healthcare organizations navigating increasingly complex financial pressures while maintaining exceptional patient care. By implementing comprehensive strategies that leverage technology, refine processes, and engage people, organizations can dramatically improve financial performance while reducing administrative burden.
Nero and Associates, Inc. specializes in performance-based revenue cycle optimization that eliminates thousands of hours of manual processes while increasing collections and improving staff satisfaction. Our proven methodologies combine AI-powered automation with process redesign to deliver measurable results quickly. Whether your organization needs comprehensive revenue cycle transformation or targeted improvements in specific areas, our team brings the expertise and technology to achieve your financial objectives while empowering your staff to focus on what matters most.

