Healthcare providers face mounting pressure to collect patient payments efficiently while maintaining positive relationships with those they serve. The shift toward high-deductible health plans has transformed patients into significant revenue sources, making effective patient collections a critical component of financial sustainability. Organizations that master collection strategies while preserving patient satisfaction position themselves for long-term success in an increasingly competitive healthcare landscape.
The Evolving Landscape of Patient Financial Responsibility
The financial dynamics between healthcare providers and patients have undergone dramatic transformation over the past decade. Patients now shoulder a larger portion of healthcare costs than ever before, with out-of-pocket expenses continuing to rise annually. This shift has fundamentally altered how medical practices, hospitals, and healthcare systems approach revenue cycle management.
Recent industry data reveals troubling trends that demand immediate attention. According to recent analysis, patient collection rates have declined by over three percentage points for commercially insured patients, signaling that traditional collection methods no longer deliver expected results. This decline represents millions in lost revenue across the healthcare industry.
Time-to-Payment Challenges
Collection timelines have extended significantly, creating cash flow obstacles for providers of all sizes. Research indicates that 74% of healthcare providers take over a month to collect patient payments, far exceeding consumer expectations for billing and payment processes. This delay strains operational budgets and diverts resources from patient care.
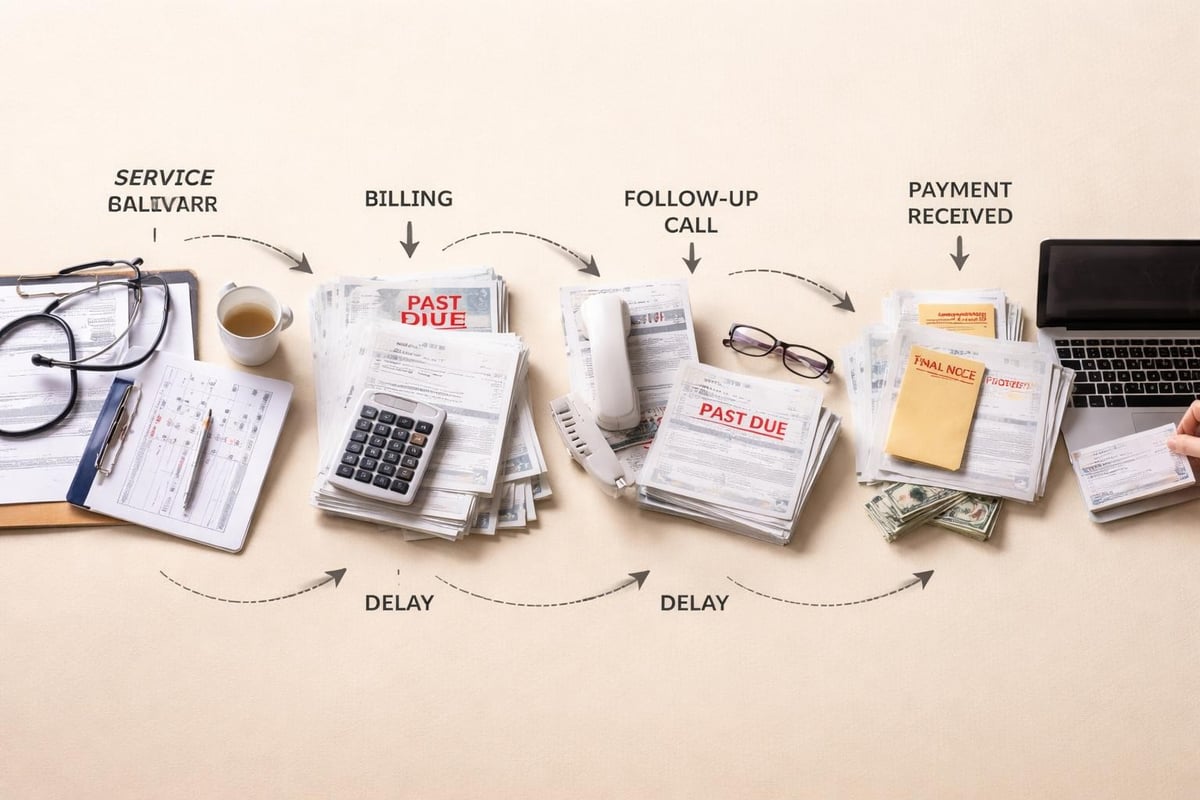
Organizations must recognize that patient collections represent more than transactional exchanges. Each interaction shapes patient perception and influences future engagement. The balance between assertive collection efforts and compassionate care delivery requires sophisticated strategies and well-trained staff.
Metrics That Drive Collection Performance
Measurement forms the foundation of improvement in any business process. Patient collections require specific key performance indicators that illuminate both successes and opportunities for enhancement. Organizations that track the right metrics gain actionable insights that transform collection outcomes.
Essential Collection Metrics
| Metric | Purpose | Target Range |
|---|---|---|
| Days in AR | Measures collection speed | 30-40 days |
| Collection Rate | Percentage of collectible revenue received | 95%+ |
| Point-of-Service Collections | Revenue collected at time of visit | 50-70% |
| Bad Debt Ratio | Uncollectible accounts as percentage of revenue | Less than 4% |
| Cost to Collect | Expenses per dollar collected | $0.12-$0.18 |
Measuring patient collections within the revenue cycle involves tracking these indicators consistently and analyzing trends over time. Monthly reviews reveal patterns that inform strategic adjustments and operational improvements.
Patient responsibility as a percentage of total charges has climbed steadily, making collection accuracy increasingly important. Organizations must calculate patient portions correctly at the point of service, reducing billing disputes and accelerating payment timelines. Verification of insurance coverage and benefits prior to scheduled services prevents surprise bills that damage patient trust.
The cost to collect metric deserves particular attention, as inefficient processes drain resources without proportional returns. Technology investments that reduce manual work and automate routine tasks typically improve this ratio while simultaneously enhancing the patient experience.
Strategies Top Performers Implement
High-performing organizations distinguish themselves through deliberate strategy deployment rather than reactive collection efforts. These providers achieve superior results by implementing proven methodologies that address both operational efficiency and patient engagement. Top performers in patient collections share common characteristics that others can replicate.
Point-of-Service Collection Excellence
Collecting payments when services are rendered delivers multiple benefits simultaneously. Patients expect to pay at the time of service in most commercial transactions, making this practice consistent with consumer norms. Staff training on financial conversations proves essential, as awkwardness or hesitation creates missed opportunities.
- Implement co-pay and deductible collection at check-in
- Provide accurate cost estimates before scheduled procedures
- Offer multiple payment methods including digital wallets
- Train front-desk staff on confident financial discussions
- Create scripts that maintain compassion while requesting payment
Organizations that excel at point-of-service collections reduce downstream collection costs significantly. The revenue cycle management solutions implemented determine success rates, as technology enables real-time eligibility verification and accurate cost estimation.
Account Segmentation and Prioritization
Not all patient accounts require identical collection approaches. Sophisticated providers segment accounts based on balance size, payment history, and likelihood of collection. This segmentation enables resource allocation toward accounts with highest return potential.
High-value accounts with balances exceeding specific thresholds receive personalized attention and flexible payment arrangements. Medium-tier accounts benefit from automated payment plans and digital communication. Lower-balance accounts may receive automated reminders with options for single-click payment, minimizing collection costs relative to revenue potential.
Digital Engagement and Payment Options
Modern patient collections leverage technology to meet consumers where they prefer to transact. Mobile-friendly payment portals, text-to-pay options, and automated payment plans eliminate friction from the payment process. Patients increasingly demand convenience matching their experiences with retailers and service providers.
Organizations should evaluate their digital payment infrastructure regularly, ensuring compatibility with emerging payment methods and maintaining security standards. The patient portal should provide clear balance information, payment history, and self-service options that reduce administrative burden.
Communication Best Practices for Collection Success
How organizations communicate about financial obligations significantly impacts collection rates and patient satisfaction scores. Effective communication starts before services are rendered and continues through final payment receipt. Transparency, clarity, and compassion characterize successful collection communications.
Pre-Service Financial Counseling
Proactive financial discussions prevent confusion and establish clear expectations. Financial counselors should review estimated costs, insurance coverage, and payment options during scheduling or pre-admission processes. This transparency allows patients to plan financially and reduces sticker shock when bills arrive.
- Verify insurance coverage and benefits before scheduled services
- Provide written cost estimates including patient responsibility
- Discuss payment plan options for large expected balances
- Confirm contact preferences for billing communications
- Document financial conversations in patient records
Clear communication about costs demonstrates respect for patients' financial situations and builds trust. Organizations that invest in robust financial counseling programs report higher collection rates and fewer billing disputes.
Post-Service Billing Clarity
Bills should communicate charges clearly without medical coding jargon that confuses patients. Plain-language descriptions of services, itemized charges, and prominent display of amounts owed facilitate quick understanding and payment. Including payment instructions with multiple options increases likelihood of prompt payment.
Statement design matters more than many organizations recognize. Testing different formats through small pilot groups reveals which designs generate fastest payment responses. Elements like color-coding of critical information, clear due dates, and simplified payment instructions improve results measurably.
Technology Integration for Automated Collections
Manual collection processes cannot scale efficiently as patient financial responsibility grows. Technology automation transforms patient collections from labor-intensive activities into streamlined workflows that require minimal staff intervention. Strategic technology investments deliver rapid returns through improved collection rates and reduced operational costs.
Automated Payment Plans
Payment plans structured through automated systems increase collections from patients facing large balances. These systems send scheduled reminders, process recurring payments, and alert staff only when intervention becomes necessary. Patients appreciate convenient automatic payments that prevent forgotten due dates.
Implementation considerations include:
- Minimum and maximum balance thresholds for plan eligibility
- Standard plan durations based on balance size
- Interest and administrative fee policies
- Automatic escalation for missed payments
- Integration with billing and accounting systems
Organizations should review common medical billing mistakes that hurt revenue cycles to ensure automation doesn't perpetuate existing errors. Clean data and accurate charge capture remain essential regardless of collection method sophistication.
Predictive Analytics for Collection Optimization
Advanced analytics identify which accounts require human intervention versus automated handling. Machine learning models analyze payment history, demographic data, and engagement patterns to predict collection probability. This intelligence guides resource deployment toward accounts where personalized attention generates highest returns.
| Analytics Application | Benefit | Implementation Complexity |
|---|---|---|
| Propensity-to-Pay Scoring | Prioritizes high-probability accounts | Medium |
| Payment Channel Preference | Matches communication to patient preference | Low |
| Optimal Contact Timing | Schedules outreach for maximum response | Medium |
| Balance Segmentation | Automates workflow routing | Low |
| Dispute Prediction | Prevents escalation through early intervention | High |

The integration of artificial intelligence into patient collections represents a significant opportunity for healthcare organizations. These technologies handle routine interactions while escalating complex situations to experienced staff, optimizing both efficiency and effectiveness.
Compliance and Compassion in Collection Activities
Patient collections occur within strict regulatory frameworks designed to protect consumers from aggressive or deceptive practices. Organizations must balance vigorous collection efforts with full compliance and genuine compassion for patients' circumstances. Violations damage reputation and invite costly legal consequences.
Regulatory Requirements
The Fair Debt Collection Practices Act establishes boundaries for collection communications and activities. Healthcare providers must understand these requirements even when collections remain in-house rather than transferring to third-party agencies. Staff training on compliant collection practices protects the organization while ensuring respectful patient treatment.
Communication restrictions include limitations on contact times, frequency, and methods. Organizations cannot contact patients at inconvenient times or places, nor can they harass or abuse individuals regarding legitimate debts. Documentation of all collection interactions provides protection if disputes arise.
Financial Assistance Programs
Comprehensive financial assistance policies demonstrate organizational commitment to community health beyond revenue generation. These programs provide relief for patients facing genuine financial hardship while maintaining collection discipline for those with ability to pay. Clear eligibility criteria and streamlined application processes ensure consistent, fair implementation.
Organizations should promote financial assistance availability proactively rather than waiting for patients to inquire. Visibility through website information, lobby signage, and billing inserts increases program utilization among qualifying patients. Strategies to optimize patient collections emphasize balancing revenue goals with compassionate care delivery.
Staff Development and Performance Management
Technology alone cannot transform patient collections without skilled, motivated staff executing collection strategies effectively. Investment in training, coaching, and performance management creates teams that achieve collection targets while preserving patient relationships. Role-specific competencies ensure each team member contributes optimally to collection success.
Training Programs for Collection Excellence
Comprehensive training covers technical skills, communication techniques, and emotional intelligence. Financial counselors need different competencies than billing specialists or customer service representatives. Tailored curricula address role-specific requirements while building shared understanding of collection goals and organizational values.
- Financial estimation accuracy and insurance verification procedures
- Difficult conversation management and conflict resolution
- Payment plan structuring and negotiation techniques
- Technology platform proficiency for all collection tools
- Compliance requirements and documentation standards
- Empathy development and patient-centered communication
Regular refresher training reinforces skills and introduces new strategies as collection best practices evolve. Organizations should track training completion rates and assess competency through observation and performance metrics.
Performance Incentives Aligned With Goals
Well-designed incentive structures motivate collection performance without encouraging inappropriate pressure on patients. Metrics-based compensation components reward outcomes like collection rates, point-of-service collection percentages, and days in accounts receivable. Team-based incentives foster collaboration rather than internal competition.
Recognition programs highlighting collection successes build positive culture around financial performance. Sharing stories of effective patient financial conversations provides learning opportunities while celebrating individual contributions. Public acknowledgment through team meetings or internal communications reinforces desired behaviors.
Vendor Partnerships for Collection Enhancement
Many organizations benefit from specialized vendor partnerships that supplement internal collection capabilities. Third-party services range from early-out collection support to bad debt recovery and everything between. Strategic vendor selection and management maximize value while protecting patient relationships and organizational reputation.
Vendor Selection Criteria
| Evaluation Factor | Key Considerations | Weight |
|---|---|---|
| Compliance Record | Regulatory violations, litigation history | High |
| Performance Metrics | Collection rates, resolution time | High |
| Patient Experience | Communication approach, complaint rates | High |
| Technology Integration | System compatibility, data security | Medium |
| Pricing Structure | Contingency rates, minimum fees | Medium |
| Service Offerings | Account segmentation, reporting capabilities | Low |
Thorough due diligence prevents partnerships with vendors whose practices might damage organizational reputation. References from similar healthcare providers offer valuable insights into vendor performance and patient experience.
Ongoing Vendor Management
Active vendor oversight ensures continued alignment with organizational standards and performance expectations. Regular performance reviews covering collection rates, patient complaints, and compliance incidents identify issues requiring corrective action. Communication protocols establish clear expectations for vendor interactions with patients.
Organizations should avoid common patient collection mistakes by maintaining direct oversight even when outsourcing collection activities. Vendor partnerships supplement rather than replace internal accountability for collection outcomes and patient satisfaction.
Innovation and Future Directions
Patient collections continue evolving as technology advances and consumer expectations shift. Forward-thinking organizations monitor emerging trends and pilot innovative approaches that might deliver competitive advantages. The willingness to experiment with new strategies positions providers as industry leaders rather than followers.
Artificial Intelligence Applications
AI-powered chatbots handle routine billing inquiries, freeing staff for complex situations requiring human judgment. Natural language processing interprets patient questions and provides accurate responses instantly, improving satisfaction while reducing administrative costs. These tools learn from interactions, continuously improving response accuracy and effectiveness.
Machine learning algorithms optimize payment plan structures based on individual patient circumstances and payment probability. Rather than offering standardized plans, AI recommends customized arrangements balancing organizational cash flow needs with patient ability to pay. This personalization increases plan completion rates and total collections.
Blockchain for Payment Security
Emerging blockchain applications in healthcare payments promise enhanced security and reduced transaction costs. While widespread adoption remains years away, pilot programs demonstrate potential for streamlining payment processes and reducing fraud. Organizations should monitor developments in this space for future implementation opportunities.
The intersection of technology innovation and patient collections presents significant opportunities for organizations willing to invest strategically. Solutions enabling businesses to achieve growth and efficiency in operations often include collection automation and process optimization components.
Effective patient collections require balanced strategies that honor financial obligations while preserving the compassionate care relationships that define exceptional healthcare. Organizations implementing proven collection methodologies, leveraging appropriate technology, and developing skilled teams position themselves for sustained financial health. Nero and Associates, Inc. helps healthcare organizations optimize revenue cycle management through performance-based consulting that delivers measurable improvements in collection rates, operational efficiency, and bottom-line results.