Healthcare organizations face mounting pressure to optimize revenue while managing increasingly complex billing requirements. One critical component that determines financial success is how effectively providers document and bill for every service delivered. Understanding charge capture and its role in Revenue Cycle Management has become essential for healthcare executives seeking to protect revenue integrity and eliminate operational inefficiencies. As healthcare continues evolving in 2026, organizations that master this process position themselves for sustainable financial health and improved operational performance.
Understanding Charge Capture Fundamentals
Charge capture represents the systematic process of recording all billable services, procedures, supplies, and encounters provided to patients within a healthcare setting. This process forms the foundation of healthcare revenue cycle management, ensuring that every clinical activity translating into a billable event gets properly documented, coded, and submitted for reimbursement.
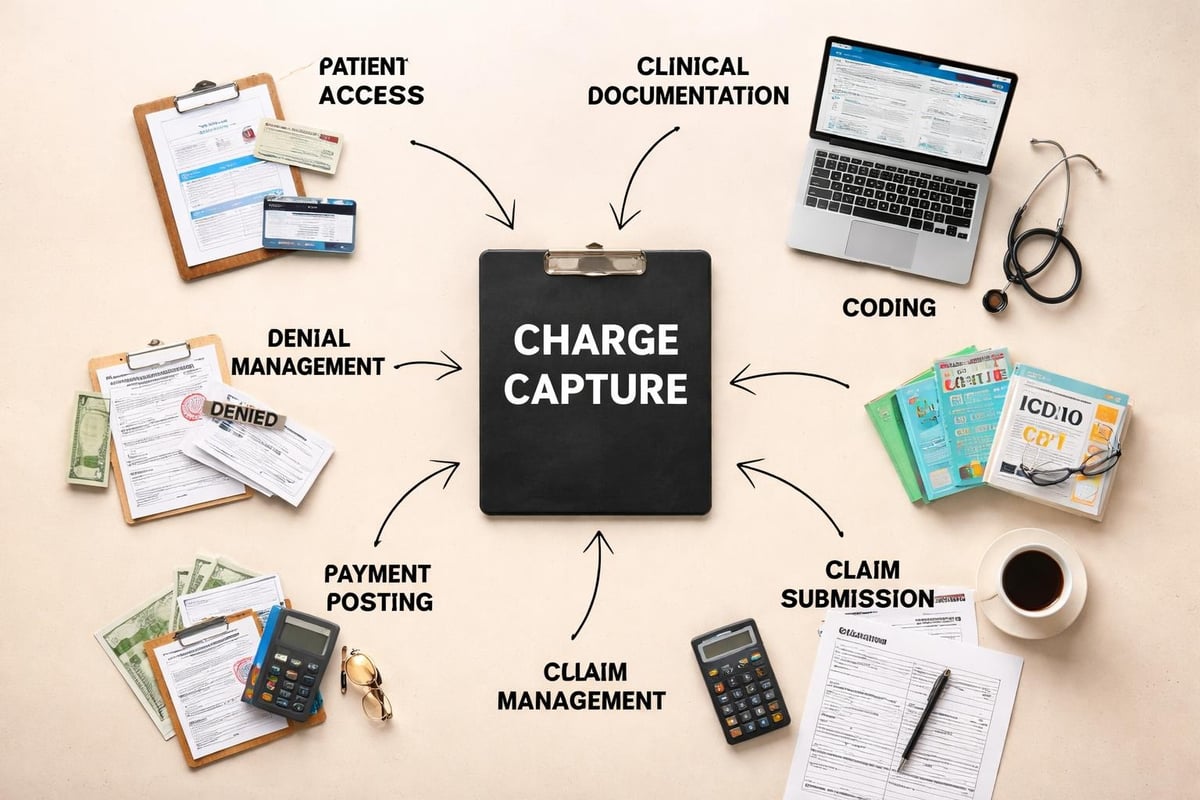
The charge capture process begins the moment a healthcare provider delivers a service and continues through documentation, coding assignment, charge entry, claim submission, and payment posting. Each step requires precision and accuracy to prevent revenue leakage and ensure compliance with regulatory requirements.
Core Components of Effective Charge Capture
Healthcare organizations must manage multiple elements to achieve comprehensive charge capture. These components work together to create a seamless revenue cycle workflow:
- Clinical documentation that accurately reflects services rendered
- Charge description master (CDM) maintenance and updates
- Coding accuracy using current CPT, ICD-10, and HCPCS codes
- Timely charge entry to minimize charge lag
- Quality assurance processes to identify missing or incorrect charges
- Staff training and education on documentation requirements
- Technology systems that support automated capture and validation

Organizations that excel in charge capture implementation typically establish clear policies defining responsibility for each step. This clarity eliminates confusion about who documents what information and when charges must be entered into billing systems.
Financial Impact and Revenue Optimization
The financial implications of charge capture extend far beyond simple billing accuracy. Healthcare organizations face significant revenue losses when charge capture processes fail to function optimally. Research indicates that inefficient charge capture can result in annual losses exceeding $100,000 per provider due to charge lag, missed charges, and documentation failures.
Quantifying Revenue Leakage
Revenue leakage occurs through multiple pathways in the charge capture process. Understanding these sources helps organizations prioritize improvement efforts:
| Revenue Leakage Source | Estimated Impact | Primary Cause |
|---|---|---|
| Charge lag (delayed entry) | 5-10% of revenue | Workflow bottlenecks |
| Missed charges | 3-7% of revenue | Documentation gaps |
| Coding errors | 2-5% of revenue | Insufficient training |
| Unbilled supplies | 1-3% of revenue | Inventory tracking issues |
| Procedure downcoding | 2-4% of revenue | Documentation quality |
Organizations implementing robust charge capture systems typically recover 8-15% of previously lost revenue within the first year. This recovery directly impacts the bottom line and improves cash flow sustainability.
The relationship between charge capture accuracy and revenue cycle performance extends to key performance indicators. Days in accounts receivable decrease when charges enter the system promptly, claim denial rates drop when coding accuracy improves, and collection rates increase when documentation supports medical necessity.
Common Challenges and Operational Barriers
Healthcare organizations encounter persistent obstacles when attempting to optimize charge capture processes. These challenges span technology limitations, human factors, and systemic issues embedded within healthcare delivery models.
Technology and Integration Issues
Modern healthcare delivery involves multiple systems that must communicate effectively to support comprehensive charge capture. Electronic health records, practice management systems, billing platforms, and departmental systems often operate in silos, creating data fragmentation.
Integration gaps between clinical and financial systems force manual data entry, increasing error rates and creating bottlenecks. When providers document services in one system and charges must be manually transferred to billing systems, opportunities for revenue leakage multiply.
Outdated technology presents another significant barrier. Legacy systems lacking real-time validation capabilities allow incorrect or incomplete charges to enter the revenue cycle, requiring costly rework and potentially resulting in claim denials.
Workflow and Human Factors
The human element in charge capture introduces both opportunities and risks. Provider documentation quality varies significantly, with some clinicians providing detailed service descriptions while others offer minimal information insufficient for accurate coding.
- Time constraints during patient encounters limit documentation thoroughness
- Lack of coding knowledge among clinical staff leads to missed charge opportunities
- Resistance to technology adoption slows implementation of automated solutions
- Insufficient training on documentation requirements creates compliance risks
- Communication gaps between clinical and revenue cycle teams prevent issue resolution
Organizations must address these human factors through comprehensive training programs, workflow optimization, and fostering collaboration between clinical and financial departments. The charge capture definition and implementation strategies require alignment across all stakeholder groups.

Best Practices for Charge Capture Excellence
Leading healthcare organizations distinguish themselves through deliberate implementation of charge capture best practices. These strategies combine technology enablement, process optimization, and cultural transformation to achieve sustainable results.
Implementing Automated Solutions
Automation represents the most significant opportunity for charge capture improvement in 2026. Artificial intelligence and machine learning technologies now identify missing charges, validate coding accuracy, and flag documentation deficiencies in real-time.
Computer-assisted coding (CAC) systems analyze clinical documentation and suggest appropriate codes based on services rendered. These systems reduce coding errors and accelerate the charge entry process while maintaining compliance with regulatory requirements.
Charge capture software integrated with electronic health records automatically creates charges based on documented clinical activities, eliminating manual charge entry for many routine services. This automation reduces charge lag and minimizes human error.
Organizations implementing automated charge capture solutions report 25-40% reductions in manual processing time and 30-50% decreases in charge entry errors. These improvements translate directly to revenue protection and operational efficiency gains.
Establishing Robust Monitoring Systems
Continuous monitoring separates high-performing organizations from those experiencing persistent revenue leakage. Effective monitoring systems track multiple dimensions of charge capture performance:
- Charge lag monitoring identifies delays between service delivery and charge entry
- Charge volume analysis detects abnormal patterns suggesting missed charges
- Coding accuracy audits ensure compliance and optimize reimbursement
- Provider-level reporting highlights documentation improvement opportunities
- Denial tracking connects claim rejections to charge capture failures
These monitoring activities should occur daily or weekly rather than monthly or quarterly. Real-time visibility enables rapid intervention before small issues become significant revenue problems.
Optimizing Specific Charge Capture Scenarios
Different healthcare settings present unique charge capture challenges requiring tailored approaches. Understanding these variations enables organizations to develop targeted improvement strategies.
Ambulatory and Outpatient Settings
Outpatient environments typically feature high patient volumes and rapid encounter turnover. This pace creates pressure on documentation and charge capture processes. Point-of-service charge capture becomes critical in these settings, where providers or staff enter charges immediately following service delivery.
Mobile charge capture applications enable providers to document and submit charges from tablets or smartphones during patient encounters. This real-time approach eliminates transcription delays and reduces charge lag to near zero.
Supply and medication charges represent particular vulnerability in outpatient settings. Organizations must implement inventory management systems that automatically trigger charges when supplies are consumed or medications administered.
Hospital Inpatient Charge Capture
Inpatient settings involve complex, multi-day encounters with numerous billable events occurring across departments. Charge capture in healthcare hospital environments requires coordination between nursing units, ancillary departments, pharmacy, supply chain, and central billing.
Bedside charge capture systems integrated with barcode scanning ensure that supplies, medications, and procedures generate charges immediately upon use. This approach prevents the common problem of supplies consumed but never billed.
Department-specific charge capture workflows must account for unique requirements in areas such as operating rooms, emergency departments, imaging centers, and laboratories. Each department may maintain its own charge capture systems requiring integration with central billing platforms.
| Setting Type | Primary Challenge | Recommended Solution |
|---|---|---|
| Emergency Department | High volume, rapid turnover | Automated charge triggers from EHR orders |
| Operating Room | Complex procedures, multiple supplies | Integrated preference card management |
| Imaging Centers | Technical vs. professional components | Automated charge splitting logic |
| Pharmacy | Medication tracking accuracy | Barcode scanning with automated dispensing |
Revenue Cycle Integration and Optimization
Charge capture does not exist in isolation but rather functions as one component within the broader revenue cycle ecosystem. Organizations achieve optimal results when they view charge capture within Revenue Cycle Management as an integrated process connected to patient access, coding, billing, collections, and payment posting.
Upstream Dependencies
Charge capture effectiveness depends heavily on processes occurring before service delivery. Patient registration accuracy ensures that charges associate with correct patient accounts and insurance information. Pre-authorization verification prevents charges from being submitted for non-covered services that will ultimately result in denials.
Scheduling systems that capture appropriate service codes and expected procedures enable pre-population of charge entry screens, reducing manual work and accelerating the charge capture timeline.
Downstream Impacts
Charge capture quality directly influences every subsequent revenue cycle step. Accurate, complete charges submitted promptly enable clean claim creation with minimal errors. Claims scrubbing systems identify fewer issues when charges contain correct codes, appropriate modifiers, and supporting documentation references.
The coding and billing teams experience reduced workload when charge capture processes incorporate front-end validation. Rather than identifying and correcting charge errors during claim preparation, these teams can focus on complex coding scenarios and denial management activities.
Collection performance improves when charges accurately reflect services rendered with appropriate supporting documentation. Payers process claims faster and deny fewer charges when medical necessity is clearly established through complete clinical information linked to each charge.
Compliance and Regulatory Considerations
Healthcare charge capture operates within a complex regulatory environment requiring strict adherence to federal and state requirements. Organizations face significant financial and legal risks when charge capture processes fail to maintain compliance standards.
Documentation Requirements and Medical Necessity
Every charge submitted for reimbursement must be supported by documentation establishing medical necessity and accurately describing services rendered. The charge capture and documentation relationship forms the foundation of compliance programs.
Documentation must contain sufficient detail to justify the level of service billed, including relevant patient history, examination findings, clinical decision-making, and treatment provided. Insufficient documentation creates vulnerability to payer audits and potential fraud allegations.
Medical necessity requirements vary by payer and service type. Organizations must maintain current knowledge of coverage policies and ensure that charges align with documented diagnoses and clinical indications. Automated systems can validate medical necessity by comparing procedure codes against diagnosis codes and payer-specific policies.
Avoiding Upcoding and Unbundling Violations
Compliance programs must specifically address risks related to upcoding and unbundling. Upcoding occurs when providers bill higher-level services than documentation supports, while unbundling involves separately billing component services that should be reported under a single comprehensive code.
Education programs should train clinical and coding staff on proper code selection, modifier usage, and bundling rules. Regular auditing identifies patterns suggesting inadvertent compliance violations before they escalate to regulatory investigations.
Performance Metrics and Continuous Improvement
Organizations committed to charge capture excellence establish comprehensive measurement frameworks tracking performance across multiple dimensions. These metrics drive accountability and guide continuous improvement efforts.
Key Performance Indicators
Effective charge capture measurement incorporates both financial and operational indicators:
- Charge lag time (average hours between service delivery and charge entry)
- Charge capture rate (percentage of services generating charges)
- Coding accuracy rate (percentage of charges coded correctly on first submission)
- Denied charge percentage (charges rejected due to capture or coding errors)
- Revenue per encounter (trending to identify missed charge opportunities)
- Charge correction rate (percentage requiring post-submission amendments)
Organizations should establish benchmarks for each metric and monitor trends monthly. Improvement targets should be realistic yet ambitious, driving incremental gains over time rather than expecting immediate perfection.
Building a Culture of Revenue Integrity
Sustainable charge capture improvement requires cultural transformation beyond mere process changes. Clinical staff must understand how their documentation directly impacts organizational financial health and their own compensation in value-based payment models.
Revenue integrity programs foster collaboration between clinical and financial teams, breaking down traditional silos that prevent effective communication. Regular meetings bringing together providers, coders, billers, and revenue cycle leaders enable shared learning and rapid problem resolution.
Recognition programs celebrating documentation excellence and charge capture accuracy reinforce desired behaviors. When organizations publicly acknowledge providers who consistently deliver high-quality documentation supporting complete charge capture, others are motivated to improve their own performance.
Technology Evolution and Future Trends
Charge capture technology continues evolving rapidly, with artificial intelligence and automation creating unprecedented opportunities for improvement. Organizations planning their 2026 technology investments should consider emerging capabilities transforming charge capture processes.
Artificial Intelligence Applications
Machine learning algorithms now analyze historical charge patterns to identify probable missing charges. These systems compare typical charges associated with specific diagnoses or procedures against actual charges submitted, flagging anomalies for investigation.
Natural language processing extracts billable services from unstructured clinical documentation, automatically suggesting charges based on provider notes. This technology reduces documentation burden while improving charge capture completeness.
Predictive analytics identify providers or departments at highest risk for charge capture failures, enabling targeted interventions before revenue leakage occurs. Organizations implementing AI-powered charge capture report 15-30% increases in identified billable services.
Mobile and Cloud-Based Solutions
Cloud-based charge capture platforms offer flexibility and scalability impossible with traditional on-premise systems. These solutions support remote access, enabling providers to review and approve charges from any location.
Mobile applications bring charge capture directly to the point of care, eliminating delays associated with returning to workstations. Voice-enabled charge capture allows providers to dictate charges using natural language, which systems then translate into appropriate billing codes.
Effective charge capture represents a critical foundation for healthcare revenue integrity, requiring coordinated efforts across clinical documentation, technology implementation, staff training, and continuous monitoring. Organizations that invest in optimizing these processes protect revenue, reduce administrative burden, and position themselves for long-term financial sustainability. Nero and Associates, Inc. partners with healthcare organizations to transform revenue cycle operations through intelligent automation, process optimization, and comprehensive performance improvement strategies that eliminate manual inefficiencies while maximizing revenue capture and operational excellence.

