In 2026, electronic claims are transforming healthcare administration with faster payments, fewer errors, and unmatched efficiency. As organizations seek new ways to optimize their revenue cycles, understanding the latest in electronic claims technology has never been more critical.
This guide delivers a comprehensive, step-by-step roadmap for mastering electronic claims submission, payment, and remittance. You will discover the evolution of electronic claims, new compliance standards, streamlined submission processes, payment and remittance innovations, best practices for integration, and future trends.
Ready to unlock greater efficiency and accuracy? Dive in to see how your organization can lead the way in electronic claims management.
The Evolution of Electronic Claims: 2026 Landscape
Electronic claims have fundamentally changed how healthcare organizations manage billing and reimbursement. In the early days, claims processing relied on paper forms, manual data entry, and postal delivery. Over time, the industry transitioned to Electronic Data Interchange (EDI), setting the stage for digital transformation. By 2026, regulatory requirements, cost pressures, and the pursuit of efficiency have driven nearly all major payers and providers to adopt advanced EDI and AI-powered workflows. Organizations like CMS and PerformCare now process over 90% of claims electronically. For a deeper look at industry projections, see Experian Health’s 2026 Revenue Cycle Management Predictions.
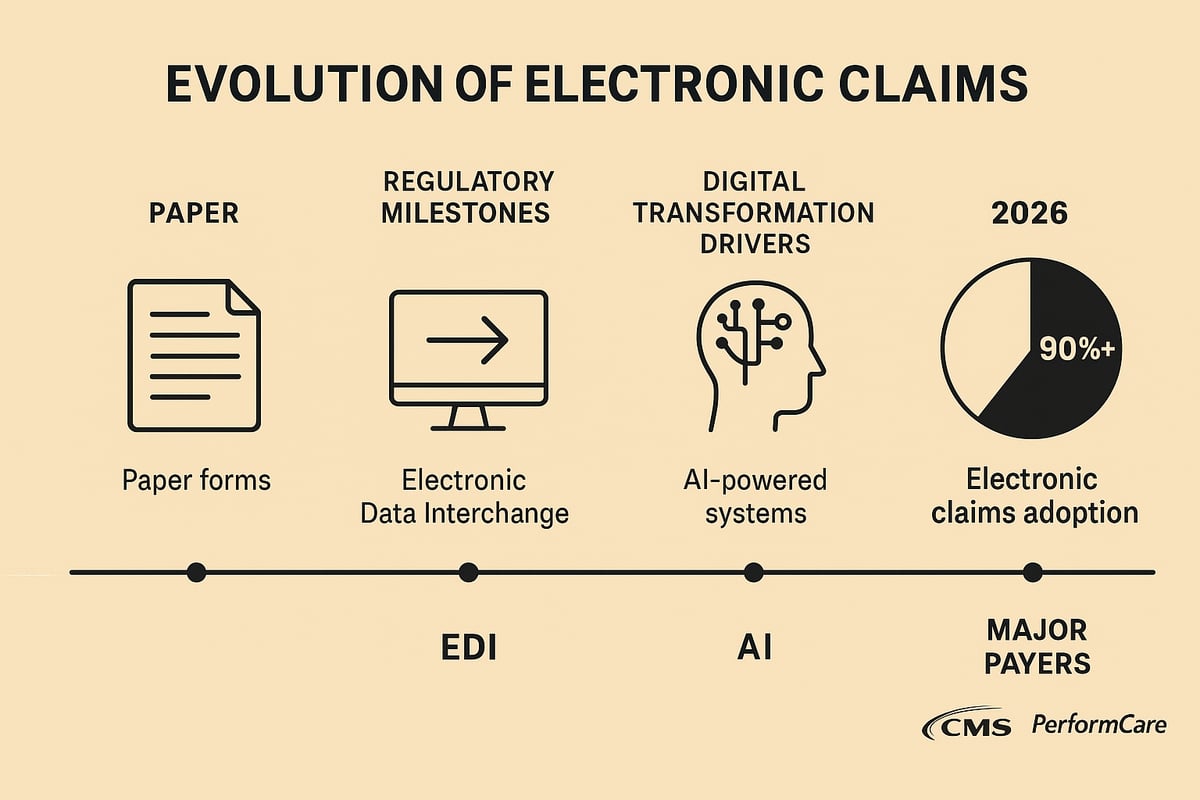
The Shift from Paper to Digital
The journey from paper-based claims to electronic claims has been shaped by the need for speed, accuracy, and cost control. Historically, claims were mailed, often resulting in long payment cycles and frequent errors. The adoption of EDI brought automation, enabling direct data transmission between providers and payers. In 2026, this shift is nearly complete, with organizations like CMS and major commercial payers leveraging automated, fully digital workflows. Regulatory mandates, technological advances, and the demand for efficiency have made this transformation possible. Today, over 90% of claims are processed electronically, reflecting the widespread embrace of electronic claims.
Regulatory Changes and Compliance Requirements
The regulatory landscape for electronic claims in 2026 is more complex and robust than ever. HIPAA, CMS, and individual payers have updated their requirements, mandating the use of standards like ANSI 5010 ASC X12 and the 837/835 EDI formats. The 275 transaction is now standard for claim attachments, ensuring all supporting documents are transmitted securely. Payer IDs and clearinghouse registration are required for compliance, and CMS demands secure .gov and HTTPS submissions. With increased compliance audits, providers face higher penalties for non-electronic submissions, making adherence to electronic claims standards essential for every healthcare organization.
Key Benefits of Electronic Claims in 2026
The adoption of electronic claims delivers tangible benefits across the revenue cycle. Providers now experience faster reimbursement cycles, with payments arriving in days rather than weeks. Real-time claim validation tools reduce errors and denials, improving cash flow and operational efficiency. Enhanced data security safeguards patient information, supporting HIPAA compliance. Cost savings are significant as paper, postage, and manual labor are eliminated. Organizations using solutions like ConnectCenter or Availity report substantial reductions in claim rejections, underscoring the value of modern electronic claims technology.
Common Challenges and How They’re Addressed
Despite the advantages, healthcare organizations often encounter challenges when implementing electronic claims. Integration with legacy systems can be complex, creating workflow bottlenecks. Staff require training to adapt to new platforms and processes. Handling attachments and payer-specific requirements adds another layer of complexity. To address these issues, vendors offer robust support, including online tutorials and real-time claim correction tools. These resources empower providers to quickly resolve errors, streamline onboarding, and ensure that electronic claims processes are efficient and compliant.
Step-by-Step Guide to Electronic Claims Submission
Mastering electronic claims in 2026 means understanding every step, from selecting the right submission channel to ensuring all supporting documentation is in place. This guide breaks down the process, making it easier to optimize your workflow and reduce denials.
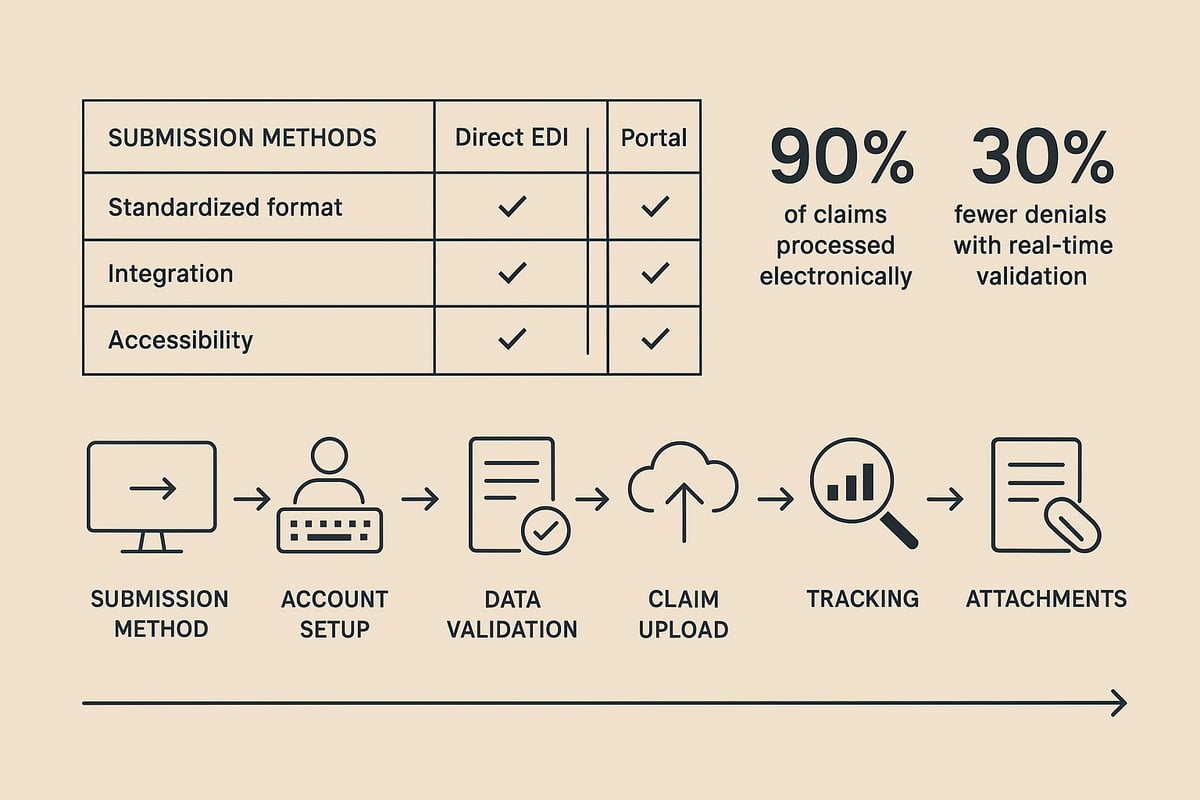
Choosing the Right Submission Method
Selecting the best way to submit electronic claims is crucial for efficiency. Providers can choose between direct EDI connections, clearinghouses, or payer portals. Each option offers unique benefits and challenges.
| Method | Pros | Cons |
|---|---|---|
| Direct EDI | Fast, direct, customizable | Complex setup, IT required |
| Clearinghouse | Multi-payer, validation | Fees, sometimes slower |
| Portal | No IT needed, easy access | Manual entry, time-consuming |
Consider your claim volume, specialty, payer mix, and integration needs. Most organizations use multiple channels for redundancy, ensuring their electronic claims reach payers even if one route fails.
Registering and Setting Up Accounts
Before submitting electronic claims, you must register with your chosen vendors and payers. Start by selecting a clearinghouse or portal, then create accounts using your NPI, TIN, and payer IDs, such as 65391 for PerformCare.
For example, the Availity registration process is straightforward and includes enabling 275 attachments if required. It is essential to use secure logins and follow proper data handling procedures during setup. Ensuring all accounts are correctly configured lays the foundation for seamless electronic claims processing.
Preparing and Validating Claims Data
Accurate data is the backbone of successful electronic claims. Gather patient demographics, provider details, and service information. Use correct ICD-10, CPT, and HCPCS codes, along with place of service codes.
Leverage real-time validation tools like ConnectCenter to catch errors before submission. Proper coding is critical, so following medical coding best practices helps reduce rejections and denials. For institutional and professional claims, ensure data is formatted correctly to meet payer requirements.
Submitting Claims Electronically
Once your data is ready, enter it into your system, upload any required attachments, and choose between batch or portal submission. Most electronic claims use the 837 EDI file format, while attachments may be PDF, TIFF, JPEG, or DOCX.
Submitting via platforms like ConnectCenter, Availity, or PCH Global is intuitive. Use claim correction screens and dashboard tracking tools for an extra layer of oversight. Consistent process adherence helps maintain high first-pass acceptance rates for your electronic claims.
Tracking Claims and Managing Rejections
Effective tracking is essential for electronic claims success. Use dashboards, work lists, and automated notifications to monitor claim status. Address denials quickly by using real-time correction tools and resubmitting as needed.
Integrated claim reports with correction screens make managing rejections simpler. Providers who use real-time validation typically see up to 30 percent fewer denials, highlighting the importance of prompt follow-up in your electronic claims workflow.
Attaching and Managing Supporting Documentation
Many electronic claims require supporting documentation, handled through 275 claim attachment transactions. You can submit attachments in batches or via portal uploads, adhering to file size and format restrictions, such as 10 files at 10MB each.
Use report codes to link attachments to claims for easier tracking. Platforms like Availity provide user-friendly attachment processes and offer training demos to help staff stay current. Proper management of documentation ensures your electronic claims meet all payer requirements and avoid unnecessary delays.
Innovations in Electronic Payment and Remittance
Electronic claims in 2026 are reshaping the healthcare payment landscape, introducing greater speed, security, and automation across the revenue cycle. Innovations in payment and remittance processes are not only improving cash flow but also reducing administrative burdens for providers and payers.
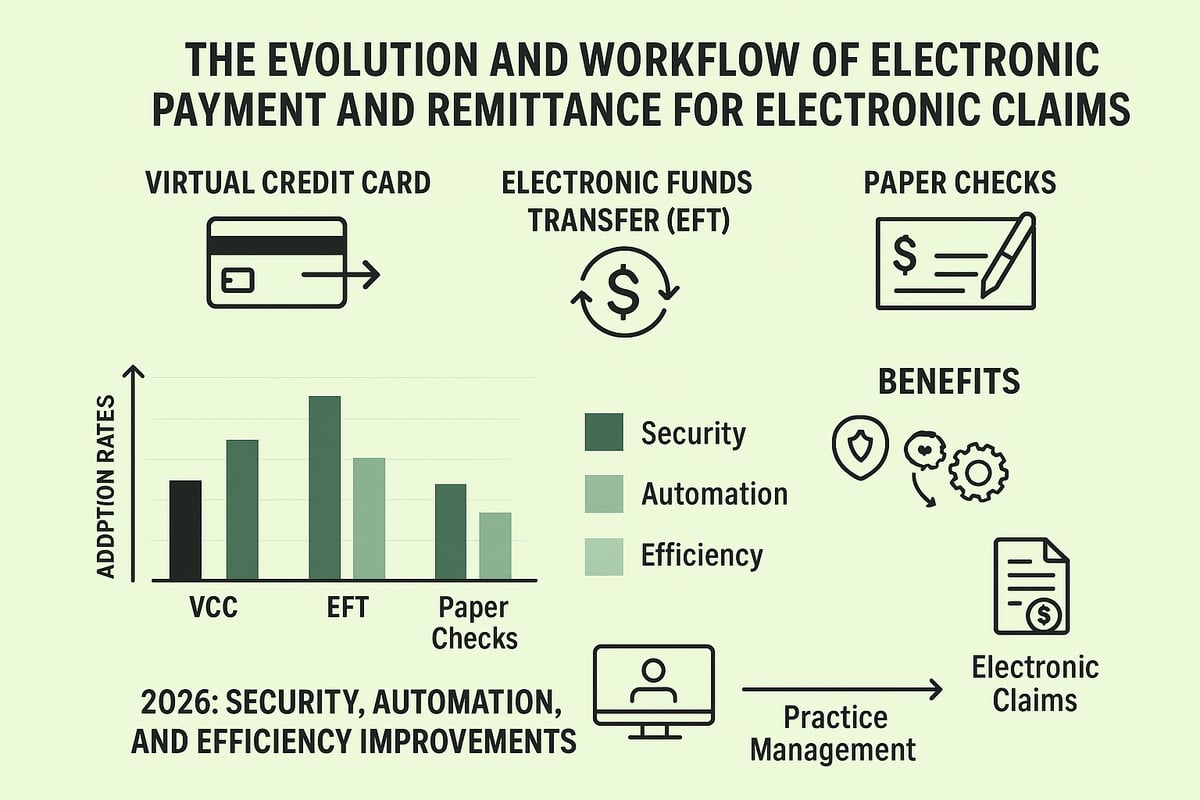
Electronic Payment Options: VCC, EFT, and Beyond
Healthcare providers managing electronic claims now have access to several payment methods, each with distinct advantages. Virtual Credit Card (VCC) payments offer quick funds but may come with processing fees. Electronic Funds Transfer (EFT) is the preferred method for most, providing direct, secure deposits into provider accounts with minimal delay. Paper checks, while still available, are rapidly declining as more organizations shift to digital-first strategies.
| Payment Method | Speed | Security | Cost | Adoption Trend |
|---|---|---|---|---|
| VCC | Fast | High | Fees | Rising |
| EFT | Fastest | Highest | Low | Dominant |
| Paper Check | Slow | Moderate | Higher | Declining |
With over 80 percent of payments for electronic claims now processed through EFT or VCC, the industry is clearly prioritizing digital efficiency.
Enrolling for Electronic Payments
To take full advantage of electronic claims innovations, providers must enroll for electronic payments with their payers or third-party partners. The process typically includes:
- Selecting a payment vendor or clearinghouse, such as ECHO Health.
- Completing an EFT enrollment form with organization details and banking information.
- Submitting documentation, like a voided check, for verification.
- Awaiting confirmation and activation of electronic payment services.
Security is a core component, as electronic claims payment systems use encryption and verification steps to protect sensitive data. Direct deposit and electronic remittance advice further reduce risk compared to paper checks.
Understanding Electronic Remittance Advice (ERA)
Electronic Remittance Advice (ERA), delivered as an 835 file, streamlines the reconciliation process for electronic claims. ERAs provide detailed explanations of payments, adjustments, and denials, making it easier to match payments to submitted claims.
Providers can access and download ERAs directly from payer portals or integrate them with practice management systems. For example, Change Healthcare and ECHO Health offer seamless ERA delivery, which can reduce manual posting times by up to 50 percent. This efficiency is a major benefit for organizations handling high volumes of electronic claims.
Integrating Payments with Practice Management Systems
Successful management of electronic claims relies on integrating payment and remittance data with practice management or billing software. When ERAs and EFTs feed directly into these systems, providers can automate posting, minimize reconciliation errors, and improve financial reporting.
Dashboards now link remittance advice to individual electronic claims, allowing staff to track payments and resolve discrepancies quickly. Ensuring that your systems are compatible with major vendors, such as Optum or Availity, is essential for a smooth workflow.
Troubleshooting Payment and Remittance Issues
Even with advanced electronic claims systems, payment delays, VCC opt-out requests, or ERA download problems can occur. Providers should:
- Keep detailed records of all electronic claims and payments.
- Use customer support resources, including live chat and knowledge bases.
- Regularly reconcile accounts to identify missing or incorrect payments.
For underpayments or denied claims, leveraging expert resources can be invaluable. Providers can efficiently recover underpayments using proven strategies that address the root causes within electronic claims workflows. Staying proactive with support and analytics ensures ongoing payment accuracy.
Integrating Electronic Claims into Your Organization’s Workflow
Every healthcare organization has a unique journey when it comes to electronic claims integration. To maximize efficiency, it is essential to evaluate current workflows, choose the right technology, invest in staff training, monitor ongoing performance, and consider specialized consulting for optimization. Let us break down each step for seamless adoption.
Assessing Your Current Claims Process
Start by mapping out your organization’s current electronic claims workflow. Identify manual steps, bottlenecks, and redundant processes that slow down claims processing. Common pain points include data entry delays, frequent errors, and high staff workload.
A simple table can help visualize areas for improvement:
| Step | Manual (hrs/wk) | Electronic Claims (hrs/wk) |
|---|---|---|
| Data Entry | 10 | 3 |
| Error Correction | 5 | 1 |
| Status Monitoring | 8 | 2 |
Time studies show that switching to electronic claims can eliminate thousands of manual hours each year. Regular workflow assessments set the foundation for future enhancements.
Selecting and Implementing the Right Technology
Choosing the right technology is crucial for successful electronic claims integration. Evaluate your EHR/EMR and practice management systems for compatibility with clearinghouses and payer portals. Look for solutions that offer seamless integration and vendor-neutral options to future-proof your investment.
Consider platforms that support end-to-end revenue cycle management to streamline electronic claims from submission to payment. Integration with leading vendors ensures your organization can adapt to payer requirements and industry updates efficiently.
Staff Training and Change Management
Successful electronic claims adoption relies on well-trained staff. Invest in comprehensive onboarding for new technology, and provide ongoing education for process updates. Use online tutorials, user guides, and demo videos to build confidence and minimize errors.
Avoiding common medical billing mistakes is vital for smooth electronic claims processing. Well-trained employees can reduce claim errors by up to 40 percent, leading to faster payments and improved accuracy.
Monitoring Performance and Continuous Improvement
Track key metrics to measure the success of your electronic claims workflow. Focus on first-pass acceptance rates, denial rates, and payment turnaround times. Use dashboards and analytics to visualize performance and set benchmarks for improvement.
Regular audits help identify trends and areas for process adjustment. Encourage feedback from staff to address bottlenecks and maintain a culture of continuous improvement. Consistent monitoring ensures your electronic claims process remains efficient and compliant.
How Performance-Based Consulting Accelerates Claims Efficiency
Performance-based consultancies bring specialized expertise to your electronic claims journey. Firms like Nero & Associates, Inc. use AI, automation, and integration to optimize revenue cycle management. Their end-to-end services include claims workflow analysis, denials management, and staff empowerment.
Organizations that leverage these consulting models see reduced administrative burdens and increased revenue, all without up-front fees. The performance-based approach ties payment to measurable results, making it a strategic option for scaling electronic claims efficiency and improving satisfaction across your team.
Future Trends and Best Practices in Electronic Claims
The future of electronic claims is being shaped by rapid advancements in technology, regulatory changes, and a growing focus on patient and provider experience. As organizations look to optimize their claims processes, understanding the trends and best practices for 2026 is essential. Below, we explore six key areas driving the next generation of electronic claims.
The Rise of AI and Automation in Claims Processing
Artificial intelligence is fundamentally changing how electronic claims are processed. AI-driven tools can now validate claims, automate coding, and flag potential denials before submission. For example, predictive analytics help organizations identify patterns in rejections, allowing for proactive corrections.
By automating repetitive tasks, AI reduces manual intervention and the risk of human error. In fact, studies show that AI can decrease manual claim touchpoints by up to 60 percent. This means claims are processed faster, with higher accuracy, and staff can focus on more complex cases. As AI becomes more accessible, its integration into electronic claims workflows will only accelerate.
Advanced Interoperability and Data Exchange
Interoperability is at the core of modern electronic claims management. The adoption of FHIR standards and robust API integrations enables real-time sharing of data between providers and payers. This leads to smoother eligibility checks, faster prior authorizations, and fewer delays.
The industry is responding to new regulatory mandates, including CMS Final Rule on Electronic Prior Authorization Requirements, which sets standards for electronic prior authorization processes in 2026. Improved interoperability reduces rework and enhances transparency across the electronic claims lifecycle, helping organizations achieve seamless data exchange.
Security, Privacy, and Compliance in 2026
Security and privacy are non-negotiable as electronic claims become the norm. Enhanced encryption protocols, secure portals, and multi-factor authentication are now standard requirements. Compliance with updated HIPAA, CMS, and payer-specific mandates is critical to protecting sensitive health information.
Organizations must conduct regular audits and invest in ongoing staff training to stay ahead of evolving threats. Secure data exchange, such as that required by CMS.gov, ensures that electronic claims are processed safely and in accordance with all regulations. Maintaining robust security protocols preserves trust and minimizes risk.
Patient Engagement and Digital Access
Patient engagement is playing a greater role in the electronic claims environment. Digital portals give patients real-time access to claim status, explanation of benefits, and payment options. Mobile-friendly interfaces and transparent billing help reduce confusion and improve satisfaction.
Providing digital access to claim information can significantly decrease billing-related inquiries and complaints. As patients become more accustomed to self-service tools, healthcare organizations must ensure their electronic claims systems are accessible, user-friendly, and responsive to patient needs.
Preparing for Regulatory and Industry Changes
The landscape for electronic claims is constantly evolving with new EDI standards, coding updates, and payer requirements. Organizations must remain agile by developing transition plans for anticipated regulatory shifts, such as changes to ANSI or X12 formats.
Staying compliant requires proactive strategies like subscribing to industry news, participating in training sessions, and maintaining open communication with payers. By anticipating changes, organizations can avoid disruptions and keep their electronic claims processes efficient and compliant.
Building a Culture of Continuous Claims Improvement
Continuous improvement is the foundation of successful electronic claims management. Collaboration between billing, IT, and clinical teams helps identify gaps and streamline workflows. Leveraging analytics to monitor denial trends and performance metrics drives better outcomes.
Regular team reviews and feedback loops foster a culture of innovation. Data shows that organizations committed to continuous improvement achieve lasting efficiency gains and higher first-pass acceptance rates. By prioritizing ongoing learning and adaptation, healthcare organizations can maximize the benefits of electronic claims.
Now that you have a clear roadmap for streamlining electronic claims in 2026, you may be wondering how to put these strategies into practice for your organization. The right guidance can make all the difference—from optimizing workflows and integrating new technologies to empowering your team for lasting efficiency and improved outcomes. If you’re ready to boost your bottom line, save valuable time, and create a healthier workplace, let’s talk about how tailored solutions can work for you.
Book a Consultation
and take the next step toward a smarter, more effective claims process.