Healthcare providers and organizations face mounting pressure to optimize revenue cycles while managing increasingly complex administrative workflows. Insurance verification stands as one of the most critical yet time-consuming processes in healthcare administration, directly impacting cash flow, claim approval rates, and overall operational efficiency. When executed properly, this process can mean the difference between smooth reimbursement and costly denials that drain resources and frustrate patients. Understanding how to streamline and automate insurance verification has become essential for organizations seeking to maintain financial health in 2026's challenging healthcare landscape.
The Financial Impact of Effective Insurance Verification
Organizations lose millions annually due to inadequate verification processes. Claim denials resulting from eligibility issues represent one of the largest preventable revenue losses in healthcare, with studies showing that up to 30% of denials stem from registration and eligibility problems.
The cost extends beyond denied claims. Staff spend countless hours reworking rejected claims, contacting insurance companies, and managing patient billing disputes. These manual processes create bottlenecks that slow cash flow and divert resources from patient care.
Quantifying the True Cost
Consider the operational expenses associated with manual verification:
- Staff time: Average 15-20 minutes per patient verification
- Rework costs: $25-30 per claim resubmission
- Delayed payments: 30-60 day cash flow interruptions
- Administrative overhead: 10-15% of total revenue cycle costs
| Cost Category | Manual Process | Automated Process | Savings |
|---|---|---|---|
| Time per verification | 15-20 minutes | 2-3 minutes | 85% reduction |
| Error rate | 12-18% | 2-4% | 70% improvement |
| Cost per verification | $8-12 | $1-2 | 85% savings |
| Claim denial rate | 15-20% | 3-5% | 75% reduction |
Organizations implementing robust verification systems report significant improvements in first-pass claim acceptance rates, often seeing increases from 65-70% to 90-95%.

Best Practices for Real-Time Verification
Real-time insurance verification represents the gold standard for 2026. Rather than batch processing or delayed verification, real-time insurance eligibility verification enables organizations to confirm coverage at the point of scheduling or registration.
Implementing effective real-time systems requires strategic planning. Organizations must integrate verification workflows into existing scheduling and registration platforms, ensuring that staff can access eligibility information without switching between multiple systems.
Essential Components of Effective Verification
Successful verification processes incorporate several key elements:
- Pre-appointment verification conducted 48-72 hours before scheduled visits
- Multi-payer connectivity supporting major insurance carriers and regional plans
- Automated eligibility checks that run without manual intervention
- Alert systems flagging coverage issues or discrepancies
- Documentation protocols capturing verification details for compliance
The importance of accurate patient eligibility verification cannot be overstated. Organizations that verify coverage before service delivery position themselves to address issues proactively rather than discovering problems after treatment.
Integration with existing systems ensures seamless data flow. When verification systems connect directly with practice management software, electronic health records, and billing platforms, staff avoid duplicate data entry and reduce transcription errors.
Overcoming Common Verification Challenges
Healthcare organizations encounter numerous obstacles when managing insurance verification workflows. Patient information accuracy remains a persistent challenge, with outdated contact details, incorrect policy numbers, and name discrepancies creating verification failures.
Insurance plan complexity adds another layer of difficulty. With thousands of plan variations, benefit structures, and coverage rules, staff struggle to navigate the nuances of each carrier's requirements. The challenges in insurance eligibility verification often stem from this complexity combined with manual processes.
Standardization and Consistency
Creating standardized verification checklists ensures consistency across team members. Every verification should confirm:
- Patient demographic accuracy
- Current insurance policy status
- Coverage effective dates
- Benefit limitations and exclusions
- Prior authorization requirements
- Co-payment and deductible amounts
- Out-of-network status and implications
Documentation standards prove equally important. Organizations should maintain detailed records of verification attempts, including date, time, representative contacted, and information obtained. This documentation protects against disputes and supports compliance audits.
Training programs must address both technical skills and soft skills. Staff need proficiency with verification software while also developing communication techniques for discussing coverage limitations with patients sensitively.
Leveraging Technology and Automation
Artificial intelligence and automation have transformed insurance verification from a manual, error-prone process into a streamlined, accurate system. Modern solutions can process thousands of verifications daily with minimal human intervention.
Machine learning algorithms improve over time, learning from historical data to predict coverage issues and flag high-risk accounts. These systems identify patterns that human reviewers might miss, such as seasonal coverage changes or recurring authorization requirements.
AI-Powered Verification Solutions
AI addresses non-standardized data issues that plague manual processes. Natural language processing enables systems to extract relevant information from diverse insurance portals, carrier responses, and policy documents.
The services offered through end-to-end revenue cycle management increasingly incorporate AI-driven verification as a core component. Organizations adopting these solutions report dramatic reductions in verification time and error rates.
Automation benefits extend throughout the revenue cycle:
- Reduced administrative burden on front-office staff
- Faster patient check-in processes
- Fewer claim denials and rejections
- Improved cash flow predictability
- Enhanced patient satisfaction through transparency
| Verification Method | Processing Speed | Accuracy Rate | Staff Required | Cost Efficiency |
|---|---|---|---|---|
| Manual phone calls | 15-20 min/patient | 82-88% | High | Low |
| Web portal checks | 8-12 min/patient | 88-92% | Medium | Medium |
| Batch electronic | 3-5 min/patient | 92-95% | Low | High |
| Real-time AI | 1-2 min/patient | 96-98% | Minimal | Very High |

Building Effective Verification Workflows
Implementing effective eligibility verification workflows requires careful process design. Organizations must map current workflows, identify bottlenecks, and redesign processes around patient and operational needs.
Workflow optimization begins with understanding touchpoints. From initial appointment scheduling through final payment posting, insurance verification intersects with multiple departments and systems. Each interaction represents an opportunity for improvement or a potential failure point.
Designing Patient-Centric Processes
Patient experience considerations should guide workflow design. Nobody wants to arrive for an appointment only to discover insurance issues that could have been resolved in advance. Proactive verification demonstrates respect for patient time and reduces anxiety about coverage.
Timing proves critical. Verifying insurance too early risks capturing outdated information, while verifying too late leaves insufficient time to address issues. Most organizations find that 48-72 hours before appointments provides the optimal balance.
Communication protocols should address both internal and external stakeholders:
- Internal alerts notify scheduling staff, providers, and billing teams of coverage issues
- Patient notifications inform individuals of verification results and required actions
- Carrier communications document all interactions with insurance companies
- Escalation procedures define when and how to involve management
Cross-departmental collaboration ensures seamless handoffs. When scheduling staff verify coverage, clinical teams confirm authorization, and billing departments validate claims, everyone must access the same accurate information.
Certificate of Insurance Verification for Business Partnerships
Beyond patient coverage verification, organizations managing vendor relationships and business partnerships must verify certificates of insurance. This parallel verification process protects companies from liability exposure and ensures contractual compliance.
Best practices for efficient COI tracking emphasize proactive monitoring and automated renewal alerts. Organizations should maintain a centralized repository of all vendor certificates with clear expiration tracking.
Risk Mitigation Through Thorough Verification
Business insurance verification protects against:
- Liability gaps where vendors lack adequate coverage
- Financial exposure from uninsured incidents or accidents
- Contractual violations resulting in legal disputes
- Reputational damage from association with uninsured partners
The verification process should confirm coverage amounts meet contractual requirements, policy dates encompass service periods, and the organization appears as an additional insured when appropriate. Regular audits ensure ongoing compliance rather than relying on initial verification alone.
Performance Metrics and Continuous Improvement
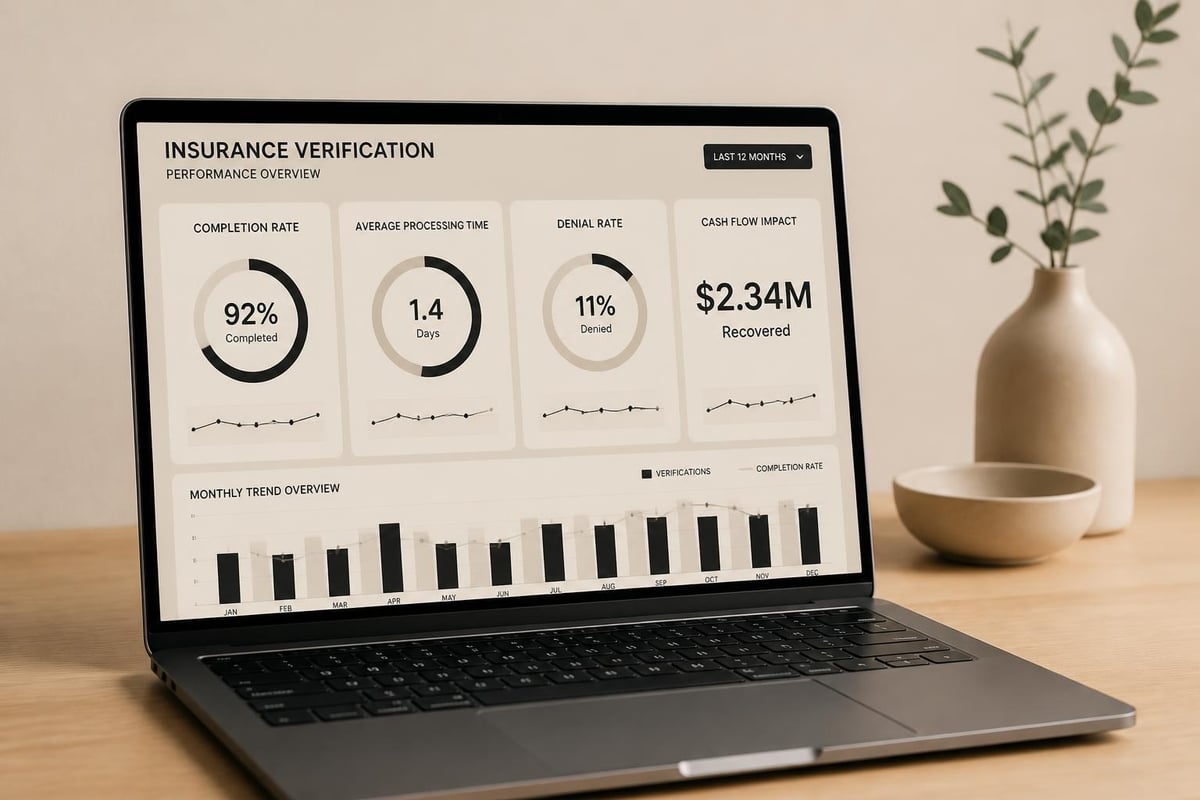
Measuring verification performance enables data-driven optimization. Organizations should track key performance indicators that reveal both efficiency and effectiveness.
Essential metrics include:
- Verification completion rate (percentage of patients verified before service)
- Average time to complete verification
- Error rate and rework frequency
- First-pass claim acceptance rate
- Days in accounts receivable
- Denial rate attributable to eligibility issues
| KPI | Industry Baseline | High Performers | Target Goal |
|---|---|---|---|
| Pre-service verification rate | 65-75% | 92-98% | >95% |
| Eligibility-related denials | 12-18% | 2-4% | <5% |
| Verification error rate | 10-15% | 1-3% | <3% |
| Average verification time | 12-15 min | 2-3 min | <5 min |
Regular performance reviews identify trends and improvement opportunities. Monthly dashboard reviews should involve stakeholders from scheduling, clinical, and financial teams to ensure comprehensive perspective.
Training and Staff Development
Technology alone cannot guarantee verification success. Staff competency and engagement prove equally important. Comprehensive training programs should address both initial onboarding and ongoing skill development.
New team members require foundational knowledge covering insurance basics, verification procedures, system navigation, and communication skills. Experienced staff benefit from advanced training on complex scenarios, new carrier requirements, and emerging technologies.
Creating a Culture of Accuracy
Organizations with superior verification performance cultivate cultures that value precision and patient service. This cultural foundation supports:
- Accountability for verification quality
- Collaboration across departments
- Continuous learning and improvement
- Problem-solving rather than blame
- Recognition of excellence
Regular feedback loops help staff understand how their verification work impacts broader organizational outcomes. When team members see how accurate verification improves cash flow and patient satisfaction, they become invested in excellence.
Integration with Revenue Cycle Management
Insurance verification functions as a critical component within comprehensive revenue cycle management. Organizations achieving optimal results integrate verification with scheduling, registration, authorization, coding, billing, and collections.
The AI and automation solutions transforming revenue cycle operations increasingly incorporate intelligent verification as a foundational capability. When verification systems share data seamlessly with downstream processes, the entire cycle operates more efficiently.
Strategic integration delivers compounding benefits:
- Reduced claim denials decrease billing department workload
- Faster payments improve cash flow and financial planning
- Better data quality supports accurate coding and charge capture
- Enhanced patient communication builds satisfaction and loyalty
Organizations should view verification not as an isolated task but as an integral part of a comprehensive strategy to optimize revenue cycle performance. Investment in verification technology and processes yields returns throughout the financial ecosystem.
Regulatory Compliance and Documentation
Healthcare organizations must balance efficiency with compliance requirements. Insurance verification processes must satisfy regulatory standards while maintaining operational speed.
HIPAA privacy rules govern how organizations collect, use, and disclose patient insurance information. Verification staff require training on permissible uses and necessary safeguards. All systems should incorporate appropriate security controls and audit trails.
Documentation requirements vary by payer and service type. Organizations should develop standardized templates that capture essential information while minimizing administrative burden. Electronic documentation systems with structured data fields ensure consistency and completeness.
Audit Preparedness
Maintaining thorough verification records supports both internal quality assurance and external audits. Organizations should retain:
- Verification attempt logs with timestamps
- Eligibility responses from carriers
- Authorization documentation
- Patient communication records
- Exception handling notes
Regular internal audits identify process gaps before external reviews. Sampling verification records monthly helps ensure procedures follow established protocols and documentation meets standards.
Effective insurance verification directly impacts organizational financial health, operational efficiency, and patient satisfaction. By implementing real-time verification systems, leveraging automation and AI, standardizing workflows, and maintaining rigorous quality standards, healthcare organizations can dramatically reduce claim denials and accelerate cash flow. The transformation from manual, error-prone processes to intelligent, automated systems represents one of the highest-value improvements available to healthcare administrators today. Nero and Associates, Inc. specializes in helping organizations optimize revenue cycle operations through AI-powered automation and integration solutions that eliminate manual processes, reduce costs, and improve financial performance across healthcare enterprises.

