The healthcare industry has undergone a fundamental transformation over the past decade, shifting from a purely clinical focus to a holistic approach that prioritizes the entire journey of care. This evolution recognizes that medical expertise alone cannot guarantee optimal outcomes. Organizations that understand this shift are investing heavily in understanding and improving every interaction, communication, and touchpoint that shapes how individuals perceive and engage with their care. The result is a measurable impact on clinical outcomes, operational efficiency, and financial performance.
Understanding the Core Components of Patient Experience
Patient experience encompasses every interaction an individual has with a healthcare organization, from scheduling appointments to billing processes and clinical care delivery. Research on patient experiences across multiple hospitals reveals that these interactions form a comprehensive picture extending far beyond basic satisfaction metrics.
The distinction between satisfaction and experience is critical. Satisfaction measures whether expectations were met, while patient experience captures what actually happened during care delivery. This difference matters because two patients can report identical satisfaction scores while having vastly different experiences in terms of communication quality, wait times, and care coordination.
Key Elements That Shape Perception
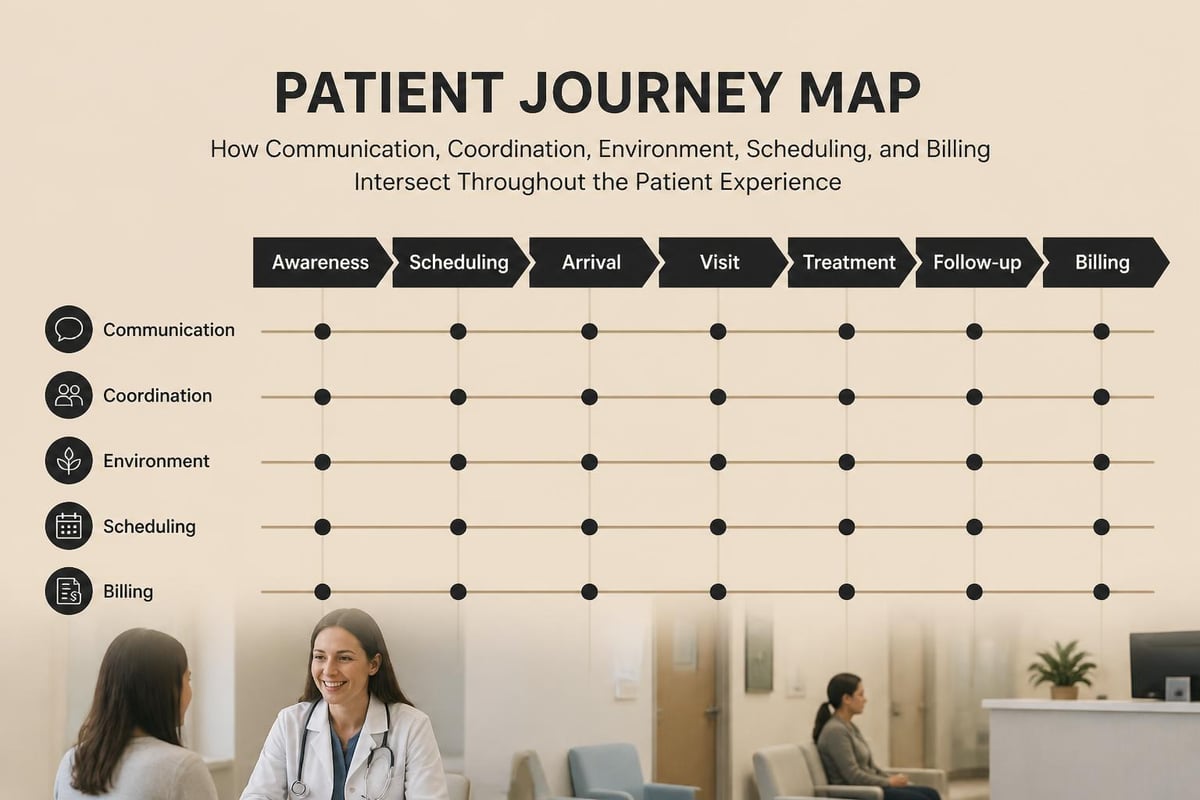
Several foundational elements consistently emerge as primary drivers of positive patient experience:
- Communication quality between providers, staff, and patients
- Care coordination across different departments and specialties
- Physical environment cleanliness, comfort, and accessibility
- Wait times for appointments, procedures, and results
- Billing transparency and financial communication clarity
These elements interconnect to create either seamless care journeys or frustrating obstacles that erode trust and compliance. Organizations that excel in patient experience recognize these connections and design systems that address multiple touchpoints simultaneously rather than treating each element in isolation.
The Business Case for Prioritizing Patient Experience
Healthcare organizations face increasing pressure to demonstrate value while managing costs and regulatory requirements. Patient experience directly influences financial performance through multiple channels that extend beyond traditional revenue streams.
Financial Impact and Operational Efficiency
Organizations with superior patient experience metrics consistently outperform peers in several measurable areas:
| Performance Metric | High Experience Organizations | Average Organizations | Impact Difference |
|---|---|---|---|
| Patient Retention | 87-92% | 68-74% | +19-24% |
| Referral Rates | 64-71% | 42-49% | +22% average |
| No-Show Rates | 4-7% | 12-18% | -8% average |
| Complaint Resolution Time | 2-4 days | 8-14 days | 65% faster |
These metrics translate directly to bottom-line results. Higher retention reduces acquisition costs, while improved referral rates drive organic growth without additional marketing investment. Lower no-show rates optimize provider schedules and eliminate wasted capacity that erodes profitability.
The strategies hospitals implement to improve patient experience often focus on systemic changes rather than superficial improvements. This approach requires investment in technology infrastructure, staff training, and process redesign, but delivers returns that compound over time.
Technology's Role in Transforming Patient Experience
Digital transformation has fundamentally altered expectations for healthcare interactions. Patients who manage banking, shopping, and communication through intuitive mobile applications expect similar convenience from healthcare providers. Organizations that fail to meet these expectations face competitive disadvantages that worsen as technology adoption accelerates.
Automation and Integration Solutions
Modern patient experience improvement relies heavily on technology that eliminates manual processes and reduces friction throughout care journeys. Automation tools address several critical pain points:
- Appointment scheduling through self-service portals and intelligent booking systems
- Pre-registration processes that gather information before facility visits
- Automated reminders reducing no-shows and improving preparation
- Digital check-in eliminating redundant paperwork and waiting room time
- Real-time communication keeping patients informed during wait periods
Organizations implementing AI and automation solutions report significant improvements in patient satisfaction scores while simultaneously reducing administrative burden on staff. This dual benefit creates virtuous cycles where employees can focus on high-value interactions rather than repetitive tasks.
The integration of disparate systems creates seamless experiences that patients notice immediately. When scheduling systems communicate with electronic health records, billing platforms, and communication tools, patients avoid repeating information and experience smoother transitions between care stages.

Human Capital Management and Experience Quality
Technology enables efficiency, but human interactions remain central to patient experience quality. The correlation between employee satisfaction and patient satisfaction is well-documented and consistently strong across healthcare settings. Organizations that invest in workforce development, wellbeing, and empowerment see measurable improvements in how patients perceive their care.
Empowering Healthcare Teams
Healthcare organizations focused on excellence recognize that frontline staff need more than clinical training to deliver exceptional experiences. They require:
- Decision-making authority to resolve patient concerns immediately
- Mental health support to manage the emotional demands of healthcare work
- Clear communication protocols ensuring consistent information delivery
- Recognition systems that reinforce patient-centered behaviors
The connection between employee empowerment and patient experience extends beyond soft skills. When staff members have access to complete patient information, appropriate technology tools, and authority to make decisions, they can anticipate needs and resolve issues proactively rather than reactively.
Financial wellness programs for healthcare employees also impact patient experience indirectly. Staff members experiencing financial stress demonstrate lower engagement, higher absenteeism, and reduced emotional capacity for patient interactions. Organizations addressing these underlying issues through comprehensive human capital management solutions create more stable, attentive workforces capable of sustaining high-quality patient interactions.
Revenue Cycle Management and Patient Experience
The financial aspects of healthcare often generate the most significant patient experience challenges. Surprise bills, confusing statements, and opaque pricing create anxiety and erode trust even when clinical care quality is excellent. Organizations that recognize billing and revenue cycle processes as core experience touchpoints gain competitive advantages through transparency and simplicity.
Redesigning Financial Interactions
Best practices for improving patient experience consistently emphasize financial communication clarity. Leading organizations implement several strategies:
- Upfront cost estimates before services are delivered
- Plain-language billing statements avoiding medical coding jargon
- Flexible payment options including payment plans and digital wallets
- Proactive financial counseling helping patients understand coverage and obligations
These changes require significant transformation in revenue cycle operations, but the return on investment manifests through higher collection rates, reduced bad debt, and improved patient loyalty. When patients understand costs before receiving care and receive clear, accurate bills afterward, their willingness to pay increases substantially.
Organizations implementing end-to-end revenue cycle management solutions often discover that process improvements designed to enhance patient experience simultaneously improve cash flow and reduce administrative costs. This alignment between patient-centered design and business objectives represents the optimal approach to revenue cycle transformation.
Measuring and Monitoring Experience Quality
Effective patient experience improvement requires systematic measurement, analysis, and action based on data insights. Organizations serious about experience quality implement comprehensive monitoring systems that capture feedback at multiple touchpoints and translate that feedback into actionable improvement initiatives.
Key Metrics and Measurement Approaches
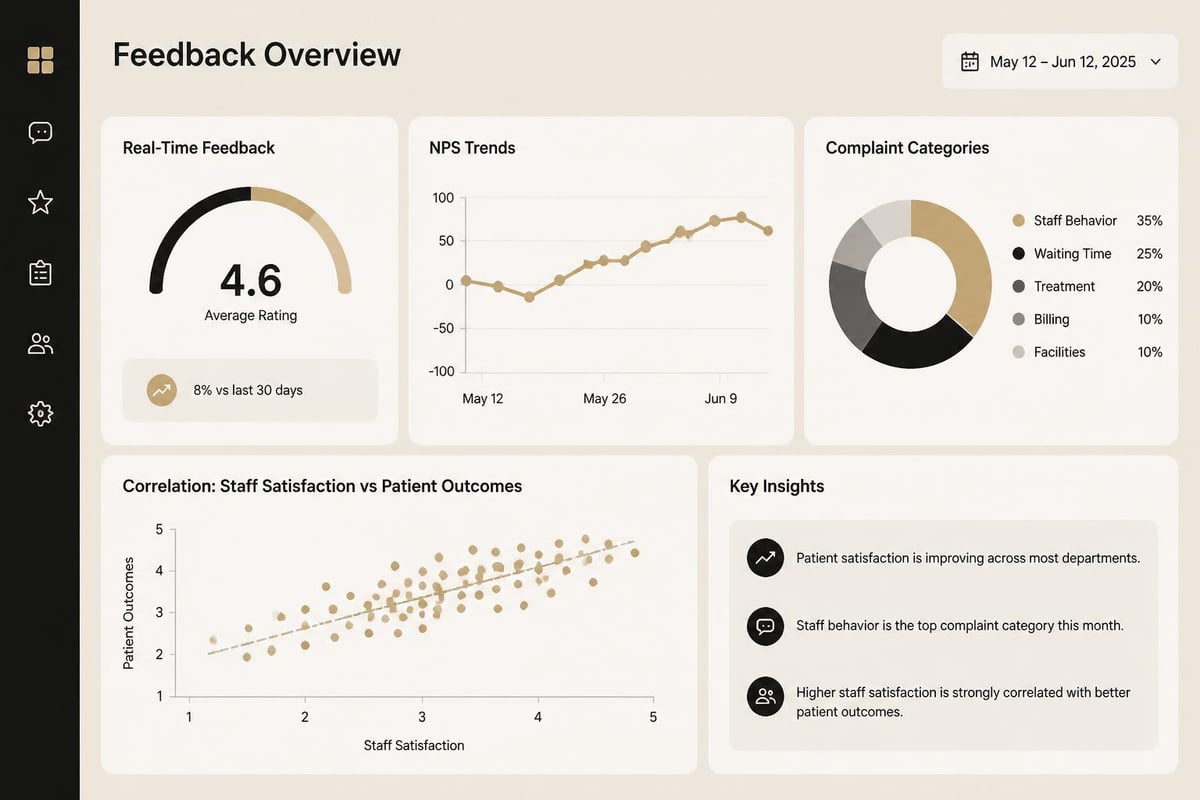
Patient experience measurement extends far beyond annual satisfaction surveys. Comprehensive programs incorporate:
- Real-time feedback collection at specific touchpoints throughout care journeys
- Net Promoter Score (NPS) tracking likelihood to recommend services
- Complaint analysis identifying systemic issues requiring attention
- Staff satisfaction metrics recognizing the employee-patient experience connection
- Operational metrics linking experience to wait times, errors, and outcomes
| Measurement Type | Collection Frequency | Primary Value | Response Rate |
|---|---|---|---|
| Post-visit surveys | After each encounter | Immediate issue detection | 18-25% |
| Annual comprehensive surveys | Yearly | Trend identification | 32-41% |
| Real-time feedback kiosks | Continuous | Service recovery opportunities | 8-14% |
| Online reviews monitoring | Continuous | Public perception tracking | N/A |
The Cleveland Clinic’s Office of Patient Experience programs demonstrate how leading organizations structure measurement and improvement systems. They combine quantitative metrics with qualitative feedback, ensuring that data reveals not just what is happening but why experiences fall short of expectations.
Advanced analytics capabilities allow organizations to identify patterns across thousands of interactions, revealing root causes of negative experiences that individual feedback cannot illuminate. These insights drive targeted interventions that address systemic issues rather than treating symptoms.
Creating Cultural Transformation Around Patient Experience
Sustainable patient experience improvement requires more than new processes and technology implementations. It demands cultural transformation where every organizational member recognizes their role in shaping patient perceptions and takes ownership for continuous improvement.
Leadership and Organizational Alignment
Cultural change begins with leadership commitment that extends beyond policy statements to tangible resource allocation and accountability structures. Organizations demonstrating genuine commitment to patient experience embed it into strategic planning, performance evaluations, and investment decisions.
Effective approaches to cultural transformation include:
- Executive rounding where senior leaders regularly interact with patients and frontline staff
- Experience champions embedded in each department to drive local improvements
- Transparent performance sharing making experience metrics visible across the organization
- Reward systems recognizing teams and individuals who exemplify patient-centered behaviors
The transition from compliance-based culture to experience-focused culture requires patience and persistence. Organizations must acknowledge that initial improvements often come from addressing obvious deficiencies, while sustainable excellence requires changing how people think about their work rather than just what they do.
Cross-Industry Lessons for Healthcare Organizations
Healthcare organizations can accelerate patient experience improvement by studying how other industries have transformed customer experience. Retail, hospitality, and financial services sectors have pioneered approaches that translate effectively to healthcare contexts when adapted appropriately.
Applying Service Excellence Principles
The hospitality industry offers particularly relevant insights for healthcare organizations. Both sectors serve people during vulnerable, high-stakes moments where emotional responses matter as much as technical competence. Optimization strategies from the hospitality sector emphasize several transferable principles:
- Anticipatory service meeting needs before they are expressed
- Personalization recognizing individuals rather than treating everyone identically
- Recovery protocols turning service failures into opportunities for building loyalty
- Environment design creating physical spaces that reduce stress and promote comfort
Financial services demonstrate how to build trust through transparency and proactive communication, particularly around complex transactions. Healthcare billing shares many characteristics with banking, including regulatory complexity, high stakes, and customer anxiety about costs. Organizations that adopt financial services communication practices often see dramatic improvements in patient satisfaction with billing processes.
Addressing Barriers to Experience Improvement
Despite widespread recognition of patient experience importance, many organizations struggle to achieve meaningful progress. Understanding common barriers helps organizations anticipate challenges and design implementation strategies that overcome resistance and resource constraints.
Common Implementation Challenges
Several obstacles consistently emerge across healthcare organizations attempting experience transformation:
| Barrier Category | Specific Challenges | Mitigation Strategies |
|---|---|---|
| Resource Constraints | Limited budgets, competing priorities | Phased implementation, ROI demonstration |
| Technology Limitations | Legacy systems, integration complexity | Incremental upgrades, middleware solutions |
| Cultural Resistance | Change fatigue, skepticism | Early wins, staff involvement in design |
| Measurement Complexity | Data silos, attribution difficulty | Unified analytics platforms, clear baselines |
Successful organizations address these barriers through strategic approaches that balance ambition with pragmatism. They recognize that transformation occurs incrementally rather than through single initiatives, building momentum through visible early successes that demonstrate value and generate organizational support for continued investment.
The role of consultancy partnerships becomes crucial when internal resources lack specific expertise or capacity for large-scale transformation projects. External partners bring cross-industry perspectives, technical capabilities, and change management experience that accelerate progress while building internal competencies for sustained improvement.
Future Trends Shaping Patient Experience
The patient experience landscape continues evolving as technology advances, demographic shifts occur, and consumer expectations rise. Organizations that anticipate these trends position themselves to lead rather than follow as the healthcare industry transforms.
Emerging Technologies and Approaches
Several developments will significantly impact patient experience over the next five years:
- Artificial intelligence for personalized care recommendations and predictive engagement
- Telehealth expansion extending convenient access while maintaining relationship quality
- Wearable device integration enabling continuous monitoring and proactive interventions
- Voice-activated interfaces simplifying information access for diverse patient populations
- Blockchain applications improving data security and patient control over health information
These technologies create opportunities for differentiation, but also raise the stakes for organizations that fail to adopt them. As leading providers implement advanced capabilities, patient expectations adjust upward, making what was innovative yesterday become standard tomorrow.
The integration of behavioral health support into primary care settings represents another significant trend. Patients increasingly expect healthcare organizations to address mental, physical, and financial wellness holistically rather than treating these dimensions separately. Organizations that develop integrated approaches to employee and patient wellness will differentiate themselves as comprehensive health partners rather than transactional service providers.
Transforming patient experience requires strategic vision, technological capability, and cultural commitment working in concert to create healthcare journeys that patients value and recommend. Organizations that approach this challenge systematically, measuring progress and adapting strategies based on evidence, position themselves for sustainable competitive advantage in an increasingly consumer-driven healthcare marketplace. Nero and Associates, Inc. partners with healthcare organizations to implement the technology infrastructure, process optimization, and workforce development strategies that elevate patient experience while improving operational efficiency and financial performance. Our performance-based approach ensures that transformation initiatives deliver measurable value across clinical, operational, and financial dimensions.

