Healthcare organizations face mounting pressure to optimize revenue while managing increasingly complex billing requirements. Every claim submission represents potential revenue, but errors, omissions, and compliance issues can derail reimbursement and strain operational resources. This challenge has made claim scrubbing an essential component of modern revenue cycle management, enabling providers to identify and correct issues before they result in costly denials or delays. Understanding how this critical process works and implementing effective strategies can transform financial performance across healthcare operations.
Understanding the Fundamentals of Claim Scrubbing
Claim scrubbing represents a systematic review process that validates medical claims against payer-specific requirements, industry standards, and compliance regulations before submission. This proactive quality control measure examines every element of a claim, from patient demographics and insurance information to procedure codes, diagnosis codes, and supporting documentation. Claim scrubbing technology helps healthcare providers catch errors that would otherwise trigger denials or rejections from insurance companies.
The process operates on multiple validation levels. First-level checks verify basic data integrity, ensuring all required fields contain properly formatted information. Second-level validation applies payer-specific rules, checking for coverage limitations, pre-authorization requirements, and coding combinations that specific insurers flag. Third-level scrutiny examines medical necessity, ensuring procedure codes align with documented diagnoses and meet industry standards for appropriate care.
Why Traditional Manual Review Falls Short
Manual claim review once served as the standard approach, with billing specialists examining each submission individually. This method consumed tremendous staff hours while still allowing errors to slip through. Human reviewers struggle to maintain consistent accuracy across hundreds of payer-specific rules that change regularly. Fatigue, distraction, and simple oversight create vulnerabilities that cost organizations money and time.

Organizations processing thousands of claims monthly cannot afford the labor intensity manual review demands. A single billing specialist might handle 50-75 claims daily through manual review, whereas automated systems process thousands in minutes. The medical billing process requires precision that human-only workflows simply cannot sustain at scale.
Financial Impact of Effective Claim Scrubbing
Revenue leakage through denied or rejected claims directly impacts organizational financial health. Industry data shows that hospitals and medical practices lose billions annually to preventable claim issues. Each denial creates cascading costs: staff time to identify the problem, resources to correct and resubmit, delayed cash flow, and potential write-offs when claims age beyond filing limits.
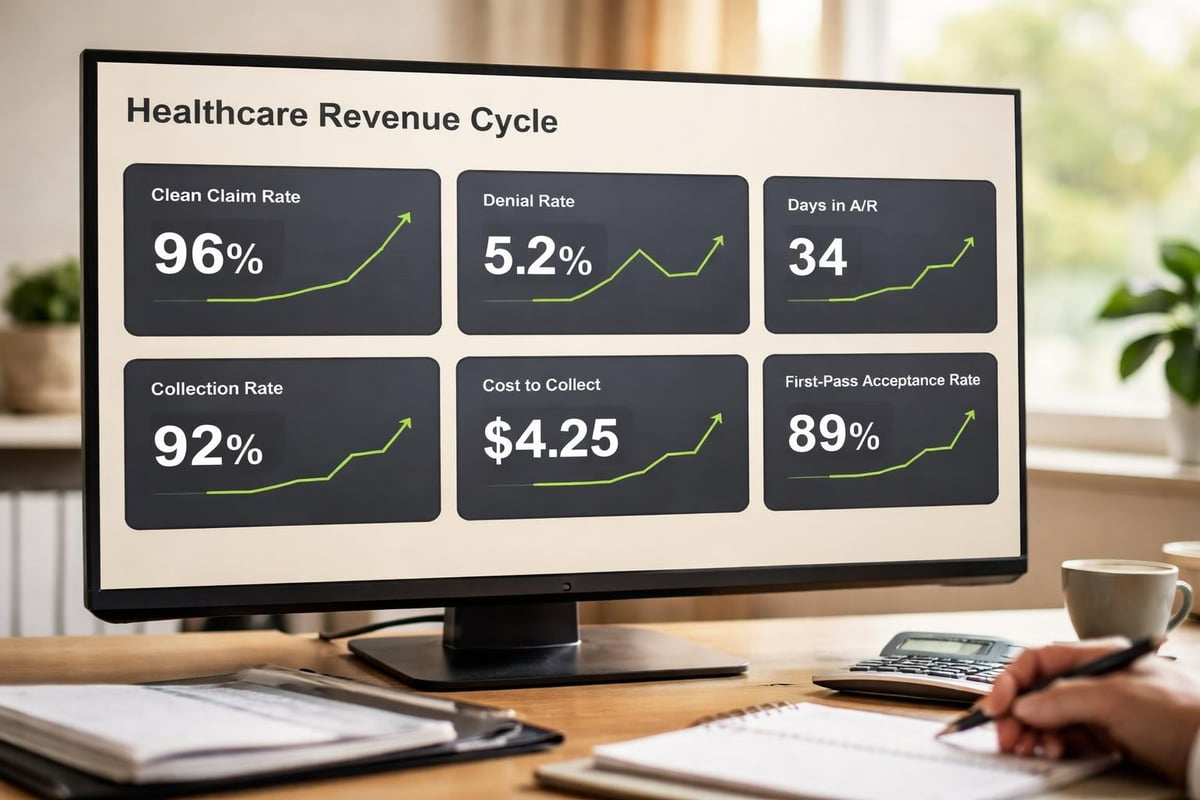
Key financial metrics improved through claim scrubbing include:
- First-pass acceptance rates increasing from 75-85% to 95-98%
- Days in accounts receivable decreasing by 15-30 days
- Denial rates dropping from 8-12% to 2-4%
- Collection rates improving by 3-7 percentage points
- Administrative costs reducing by 20-40% per claim processed
Organizations that implement comprehensive claim scrubbing solutions experience measurable improvements in working capital. When clean claims reach payers on the first submission, reimbursement arrives within standard processing windows rather than being delayed weeks or months. This acceleration compounds across thousands of claims, creating significant cash flow improvements that strengthen operational stability.
Real-World Revenue Recovery
Consider a mid-sized healthcare system processing 50,000 claims monthly with an average reimbursement of $800 per claim. At a 10% denial rate, this organization faces 5,000 denied claims monthly representing $4 million in delayed revenue. If claim scrubbing reduces denials to 3%, that represents 3,500 fewer denials and approximately $2.8 million in accelerated cash flow each month. Over a year, this improvement translates to improved financial positioning and reduced borrowing needs.
Beyond immediate revenue impact, claim scrubbing helps reduce denials and maximize revenue by preventing the administrative burden associated with rework. Every denied claim requires investigation, correction, and resubmission. Staff members must review remittance advice, identify denial reasons, obtain additional documentation when needed, update claim information, and resubmit through proper channels. This cycle diverts resources from other value-generating activities.
| Metric | Before Claim Scrubbing | After Implementation | Improvement |
|---|---|---|---|
| First-Pass Rate | 82% | 96% | +14 percentage points |
| Average Days to Payment | 42 days | 28 days | 14 days faster |
| Denial Rate | 9.5% | 2.8% | 70% reduction |
| Cost per Claim | $6.20 | $3.80 | 39% decrease |
Technology-Driven Claim Scrubbing Solutions
Modern claim scrubbing leverages sophisticated technology platforms that combine rules engines, artificial intelligence, and real-time payer connectivity. These systems maintain constantly updated rule sets reflecting the latest payer requirements, coding guidelines, and regulatory mandates. Rather than relying on periodic manual updates, cloud-based platforms receive continuous updates ensuring validation against current standards.
Artificial intelligence capabilities enhance traditional rules-based scrubbing by identifying patterns that indicate potential issues even when claims technically pass standard validation. Machine learning algorithms analyze historical denial data to predict which claim characteristics correlate with higher rejection probability. This predictive capability enables organizations to address risks proactively rather than reactively.
Integration Across the Revenue Cycle
Effective claim scrubbing solutions integrate seamlessly with existing practice management systems, electronic health records, and billing platforms. This integration enables real-time validation during the charge capture and coding process rather than waiting until the final submission stage. Early intervention prevents errors from propagating through downstream processes, reducing rework and accelerating the overall revenue cycle.
AI-powered claim scrubbing systems can process massive claim volumes while maintaining validation accuracy. Organizations handling 100,000+ claims monthly benefit from automation that human teams cannot replicate. These platforms work continuously without fatigue, applying consistent logic to every claim regardless of submission time or volume spikes.

Essential features in advanced claim scrubbing platforms:
- Real-time eligibility verification during patient registration
- Automated coding validation against current CPT, ICD-10, and HCPCS standards
- Payer-specific rule libraries covering 1,000+ insurance carriers
- Medical necessity screening based on LCD/NCD guidelines
- Duplicate claim detection preventing accidental resubmissions
- Compliance monitoring for HIPAA, Stark Law, and Anti-Kickback requirements
- Customizable business rules reflecting organizational policies
- Detailed error reporting with correction guidance
- Integration capabilities with clearinghouses and payer portals
- Analytics dashboards tracking scrubbing performance metrics
Implementing Claim Scrubbing Best Practices
Successful implementation requires more than simply activating software. Organizations must approach claim scrubbing as a strategic initiative involving process redesign, staff training, and continuous improvement. The transition from manual or basic automated review to comprehensive scrubbing demands change management that addresses workflow adjustments and role evolution.
Begin by establishing baseline metrics that quantify current performance. Track denial rates by payer, procedure type, and denial reason. Measure average days to payment, first-pass acceptance rates, and cost per claim processed. These baselines provide benchmarks against which to measure improvement and demonstrate return on investment to stakeholders.
Staff Training and Workflow Optimization
Billing staff require training not just on operating scrubbing software but on interpreting results and making informed decisions about claim submission. When systems flag potential issues, staff must understand whether to investigate further, override warnings with appropriate justification, or correct identified errors. This judgment requires clinical and coding knowledge that develops through structured education programs.
Medical billing clearinghouses employ claim scrubbing techniques that reduce errors significantly, but organizations must configure these tools appropriately. Generic settings may miss organization-specific patterns or create excessive false positives that burden staff. Customization based on your payer mix, specialty focus, and historical denial patterns optimizes validation effectiveness.
Establish regular review cycles examining claims that pass scrubbing but still receive denials. This feedback loop identifies gaps in scrubbing rules that need adjustment. Similarly, analyze claims that fail scrubbing but would have been paid if submitted. Over-aggressive scrubbing can delay legitimate claims unnecessarily, so balancing sensitivity and specificity requires ongoing refinement.
Advanced Strategies for Scrubbing Excellence
Organizations achieving industry-leading results implement strategies beyond basic automated validation. They treat claim scrubbing as part of a holistic revenue cycle optimization approach that addresses root causes of errors rather than simply catching mistakes downstream. This proactive stance reduces the volume of issues requiring scrubbing intervention in the first place.
Provider education programs ensure clinicians understand documentation requirements that support proper coding. When physicians document medical necessity clearly and completely, coders can assign accurate codes that withstand payer scrutiny. This upstream intervention reduces coding errors that scrubbing must catch later.
Payer-Specific Optimization
Different insurance carriers maintain unique requirements, preferences, and denial patterns. High-performing organizations develop payer-specific strategies that go beyond standard scrubbing rules. They maintain relationships with payer representatives, participate in provider education sessions, and study remittance patterns to understand each carrier's particular sensitivities.
Payer optimization tactics include:
- Creating customized scrubbing rule sets for top 10-20 payers by volume
- Monitoring payer policy updates and adjusting rules proactively
- Analyzing denial trends by payer to identify emerging issues
- Establishing direct communication channels with payer billing specialists
- Participating in payer webinars and training programs
- Testing claims through payer portals before official submission
| Optimization Strategy | Implementation Effort | Expected Impact | Timeline to Results |
|---|---|---|---|
| Payer-specific rules | Medium | 4-6% denial reduction | 2-3 months |
| Provider documentation training | High | 3-5% denial reduction | 4-6 months |
| Real-time eligibility verification | Low | 2-3% denial reduction | 1 month |
| Coding quality audits | Medium | 5-7% denial reduction | 3-4 months |
| Clearinghouse integration | Low | 3-4% denial reduction | 1-2 months |
Organizations processing high claim volumes benefit from dedicated staff monitoring scrubbing queues and resolving flagged issues rapidly. Rather than allowing claims to sit in suspended status, immediate resolution maintains revenue cycle velocity. This requires adequate staffing levels and clear escalation procedures when complex issues arise requiring clinical or compliance expertise.
Measuring Return on Investment
Claim scrubbing solutions require investment in technology, implementation, and ongoing maintenance. Justifying these costs demands clear demonstration of financial returns that exceed expenses. Organizations should establish comprehensive ROI frameworks capturing both hard dollar savings and operational efficiency gains.
Direct financial benefits include reduced denial rates, faster payment cycles, decreased write-offs, and lower administrative costs. Calculate the value of each denied claim avoided by considering both the claim amount and the cost of rework. A $1,000 claim requiring three hours of staff time to research, correct, and resubmit carries total costs exceeding the face value when accounting for labor at loaded rates.
Indirect benefits prove equally valuable though harder to quantify precisely. Staff morale improves when employees spend less time on frustrating rework and more time on productive activities. Patient satisfaction increases when billing runs smoothly without confusing denials or collection notices. Organizational reputation benefits when payer relationships remain positive rather than adversarial over constant claim disputes.
ROI calculation components:
- Reduction in denied claim dollars (denial rate × claim volume × average claim value)
- Savings from faster payment (improved cash flow value × borrowing costs)
- Labor cost reduction (hours saved × average staff loaded rate)
- Write-off prevention (reduction in uncollectible accounts)
- Technology and service costs (software licensing, implementation, support)
- Staff training and change management expenses
Typical ROI timelines for comprehensive claim scrubbing implementations range from 6-12 months depending on organization size and baseline performance. Organizations with higher initial denial rates see faster returns as greater improvement opportunity exists. Smaller practices may experience longer payback periods due to fixed implementation costs spread across lower claim volumes, though cloud-based solutions with per-claim pricing models improve economics for all organization sizes.
Regulatory Compliance and Risk Mitigation
Beyond financial optimization, claim scrubbing serves critical compliance functions. Healthcare billing operates under extensive regulatory oversight including HIPAA privacy and security requirements, Stark Law self-referral prohibitions, Anti-Kickback Statute restrictions, and False Claims Act provisions. Submitting claims containing errors or inappropriate coding creates legal exposure that extends beyond simple denial.
Understanding what claim scrubbing is and why it matters helps organizations recognize its role in compliance programs. Scrubbing systems validate that services billed meet medical necessity standards, that documentation supports code selection, and that claim combinations avoid prohibited unbundling or upcoding. This validation creates audit trails demonstrating good faith efforts to submit accurate claims.
Office of Inspector General audits, Recovery Audit Contractor reviews, and payer post-payment audits all examine claim accuracy and appropriateness. Organizations facing scrutiny benefit from documented scrubbing processes showing systematic validation occurred before submission. This evidence demonstrates compliance intent even when occasional errors slip through, potentially reducing penalties or adverse findings.
Documentation and Audit Support
Modern scrubbing platforms maintain detailed logs showing which validations were applied to each claim, what issues were identified, how they were resolved, and who approved final submission. This documentation proves invaluable during audits, providing clear evidence of quality control processes. Organizations can demonstrate that identified errors were corrected and that claims passing scrubbing met all applicable standards at submission time.
Regular internal audits examining scrubbing effectiveness ensure systems operate as intended. Sample claims from scrubbing queues and verify that validation logic correctly identifies issues. Test edge cases and complex scenarios to confirm rules address unusual situations appropriately. This proactive quality assurance prevents scrubbing blind spots that could allow systematic errors to pass undetected.
Future Trends in Claim Scrubbing Technology
Claim scrubbing continues evolving as technology advances and healthcare billing grows more complex. Several emerging trends promise to further enhance accuracy, efficiency, and integration across revenue cycle operations. Organizations planning long-term strategies should consider these developments in their technology roadmaps.
Artificial intelligence capabilities extend beyond current applications. Natural language processing will enable systems to analyze clinical documentation directly, validating that narrative notes support selected codes without requiring manual coder review. Predictive analytics will identify high-risk claims likely to face scrutiny, enabling preemptive additional documentation gathering or alternative coding approaches.
Blockchain technology may revolutionize claim tracking and validation. Distributed ledgers could create immutable audit trails showing exactly when claims were scrubbed, what validations occurred, and how payer adjudication proceeded. This transparency benefits both providers and payers by reducing disputes over processing timelines and validation completion.
Emerging capabilities to monitor:
- Real-time payer connectivity for instant validation against current eligibility and benefits
- Integrated prior authorization automation reducing manual intervention
- Advanced pattern recognition identifying fraud and abuse indicators
- Voice-enabled documentation assistance ensuring complete clinical notes
- Robotic process automation handling routine scrubbing queue management
- Interoperability standards enabling seamless data exchange across platforms
Organizations like Nero and Associates, Inc. help healthcare providers navigate these technological advancements, ensuring implementations align with strategic objectives while delivering measurable performance improvements. The consulting expertise needed to optimize claim scrubbing extends beyond software configuration to encompass process redesign, change management, and continuous improvement methodologies.
Integration with Broader Revenue Cycle Management
Claim scrubbing delivers maximum value when integrated within comprehensive revenue cycle management strategies rather than operating as an isolated function. Leading organizations view scrubbing as one component in an end-to-end approach spanning patient access, charge capture, coding, billing, collections, and denials management. This holistic perspective identifies how improvements in upstream processes reduce scrubbing burden while scrubbing insights inform process enhancements.
Patient access functions benefit from scrubbing data showing common eligibility issues. When registration staff understand which insurance verification gaps most frequently cause claim problems, they can emphasize those areas during patient intake. Real-time eligibility checking integrated with scrubbing platforms catches coverage issues before services are rendered, preventing downstream billing complications.
Coding quality improves through feedback loops between scrubbing results and coder education. When scrubbing consistently flags certain code combinations or medical necessity issues for specific providers, targeted training addresses these patterns. This proactive intervention reduces future error rates more effectively than simply catching and fixing individual claim mistakes.
Denials Management Synergies
Organizations implementing claim scrubbing alongside robust denials management programs achieve superior results compared to either initiative alone. Scrubbing prevents many denials from occurring initially, while denials management provides intelligence about which issues slip through scrubbing. Together, these functions create a continuous improvement cycle steadily raising clean claim rates.
Track denial reasons systematically and correlate them with scrubbing results. Claims that passed scrubbing but received denials indicate gaps in validation rules requiring attention. Conversely, analyze whether denied claims showed scrubbing warnings that were overridden, potentially indicating staff need better guidance on when overrides are appropriate.
Integration success factors:
- Unified data platforms connecting all revenue cycle systems
- Cross-functional teams including access, coding, billing, and collections staff
- Regular performance reviews examining metrics across the complete cycle
- Technology investments prioritizing interoperability and data exchange
- Leadership commitment to process improvement culture
- Vendor partnerships supporting integrated solution architectures
Organizations achieving best-in-class revenue cycle performance recognize that technology alone cannot solve operational challenges. Claim scrubbing tools provide capabilities, but realizing their potential requires strategic implementation, staff engagement, process optimization, and continuous refinement based on performance data. This comprehensive approach transforms scrubbing from a technical function into a strategic asset driving financial performance.
Vendor Selection and Implementation Planning
Choosing appropriate claim scrubbing solutions requires careful evaluation of organizational needs, existing technology infrastructure, and vendor capabilities. The market offers diverse options ranging from integrated revenue cycle management platforms with built-in scrubbing to specialized point solutions focused exclusively on claim validation. Each approach presents distinct advantages and limitations depending on organizational context.
Large health systems with complex IT environments may prefer enterprise platforms offering comprehensive functionality across all revenue cycle domains. These integrated solutions eliminate interface requirements and provide unified data repositories supporting analytics and reporting. However, they typically require significant implementation efforts and substantial financial investments.
Smaller practices and specialty groups often benefit from cloud-based scrubbing services requiring minimal IT infrastructure and offering rapid deployment. These solutions provide sophisticated validation capabilities without demanding extensive technical resources. Per-claim or subscription pricing models align costs with claim volumes, improving economic viability for organizations processing modest claim quantities.
Vendor evaluation criteria:
- Rule library breadth covering relevant payers and specialties
- Update frequency ensuring current coding and payer requirements
- Integration capabilities with existing practice management and billing systems
- User interface design supporting efficient workflow
- Reporting and analytics functionality tracking performance metrics
- Implementation support and training resources
- Ongoing customer service and technical support quality
- Pricing structure alignment with organizational budget and claim volumes
- Vendor financial stability and market reputation
- Customer references from similar organizations
Request demonstrations using actual claim data reflecting your organization's characteristics. Generic demonstrations may not reveal how solutions handle your specific payer mix, procedure types, or documentation patterns. Evaluate how systems handle edge cases and complex scenarios rather than just standard claim processing.
Effective claim scrubbing represents a cornerstone of modern revenue cycle management, delivering measurable improvements in cash flow, operational efficiency, and compliance positioning. Organizations implementing comprehensive validation strategies supported by advanced technology platforms consistently outperform peers relying on manual processes or basic automated checks.
Nero and Associates, Inc. partners with healthcare organizations to optimize revenue cycle performance through strategic consulting, technology implementation, and process transformation. Our performance-based approach ensures claim scrubbing initiatives deliver documented financial returns while positioning organizations for sustained operational excellence. Contact us today to discover how our Revenue Cycle Management solutions can help your organization maximize reimbursement, reduce administrative burden, and achieve industry-leading financial performance.

